Korean Circ J.
2020 May;50(5):443-457. 10.4070/kcj.2019.0296.
Anti-Inflammatory Effect for Atherosclerosis Progression by Sodium-Glucose Cotransporter 2 (SGLT-2) Inhibitor in a Normoglycemic Rabbit Model
- Affiliations
-
- 1Yonsei Cardiovascular Research Institute, Yonsei University College of Medicine, Seoul, Korea. KJS1218@yuhs.ac
- 2Cardiology Division, Severance Cardiovascular Hospital, Yonsei University College of Medicine, Seoul, Korea.
- 3Graduate Program in Science for Aging, Yonsei University, Seoul, Korea.
- 4Cardiovascular Product Evaluation Center, Yonsei University College of Medicine, Seoul, Korea.
- 5Division of Cardiology, Yongin Severance Hospital, Yonsei University College of Medicine, Yongin, Korea.
- 6Department of Cardiology, Ewha Womans University Seoul Hospital, Seoul, Korea.
- 7Division of Cardiology, Department of Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea.
- 8Division of Endocrinology and Metabolism, Department of Internal Medicine, Severance Hospital, Yonsei University College of Medicine, Seoul, Korea.
- KMID: 2471785
- DOI: http://doi.org/10.4070/kcj.2019.0296
Abstract
- BACKGROUND AND OBJECTIVES
We sought to investigate an anti-atherosclerotic and anti-inflammatory effect of sodium-glucose cotransporter-2 (SGLT-2) inhibitors in normoglycemic atherosclerotic rabbit model.
METHODS
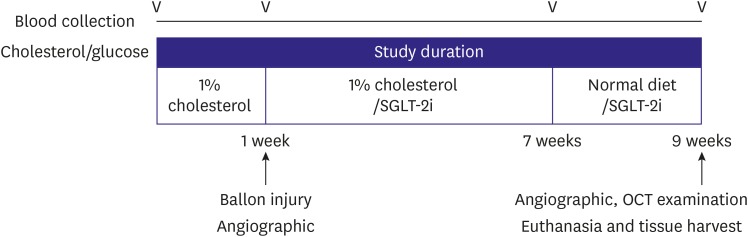
Male New Zealand white rabbits (n=26) were fed with a 1% high-cholesterol diet for 7 weeks followed by normal diet for 2 weeks. After balloon catheter injury, the rabbits were administered with the Dapagliflozin (1mg/kg/day) or control-medium for 8 weeks (n=13 for each group). All lesions were assessed with angiography, optical coherence tomography (OCT), and histological assessment.
RESULTS
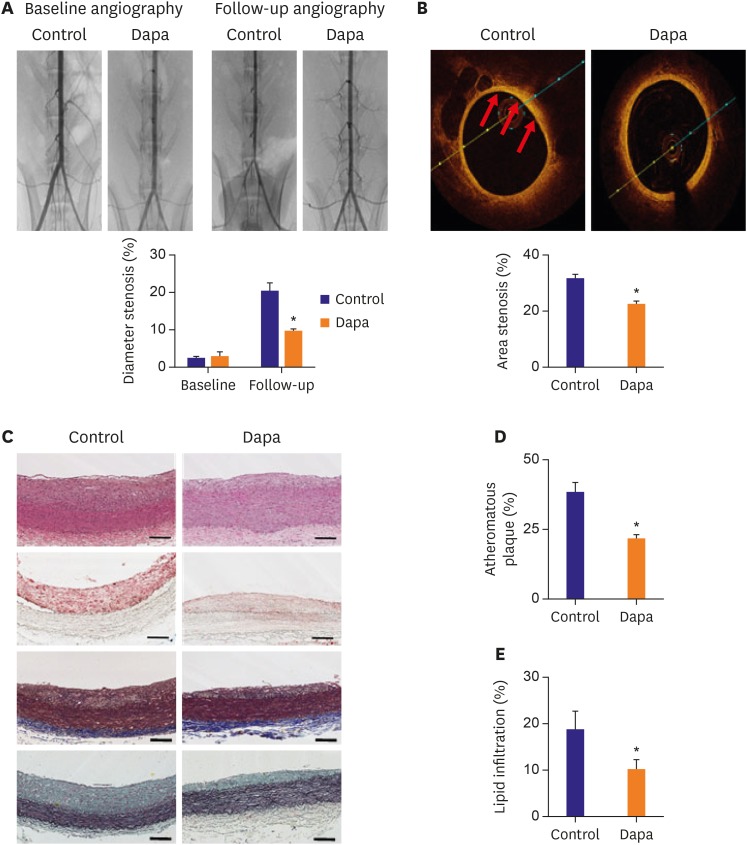
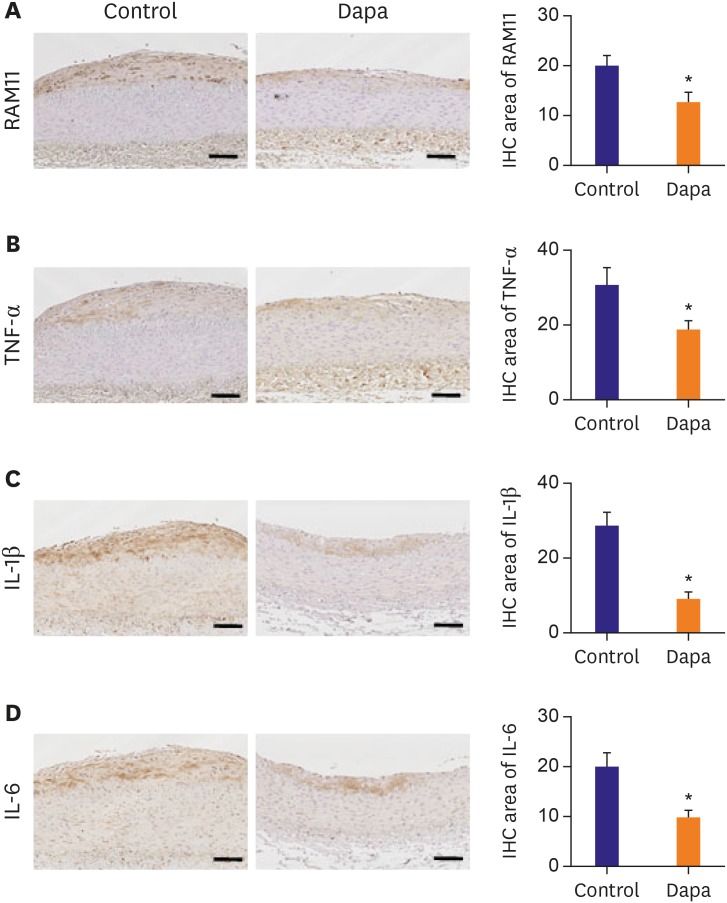
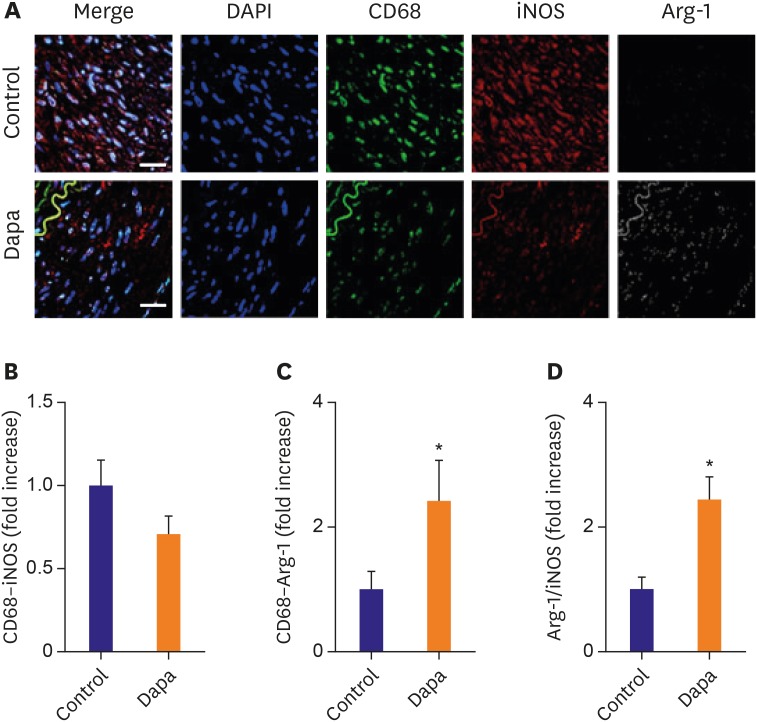
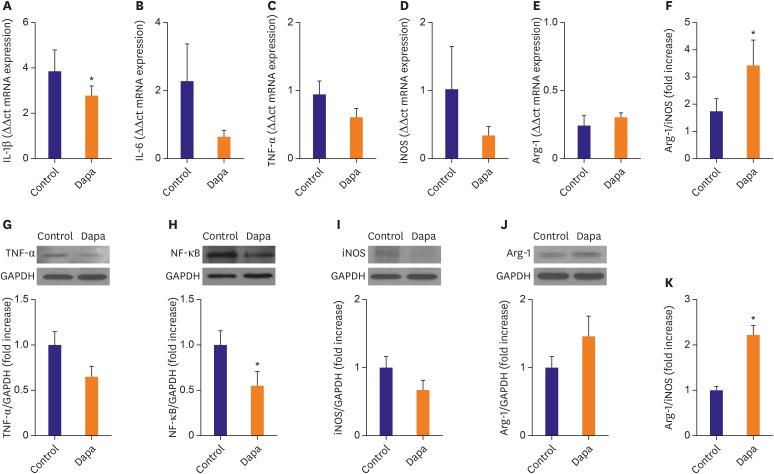
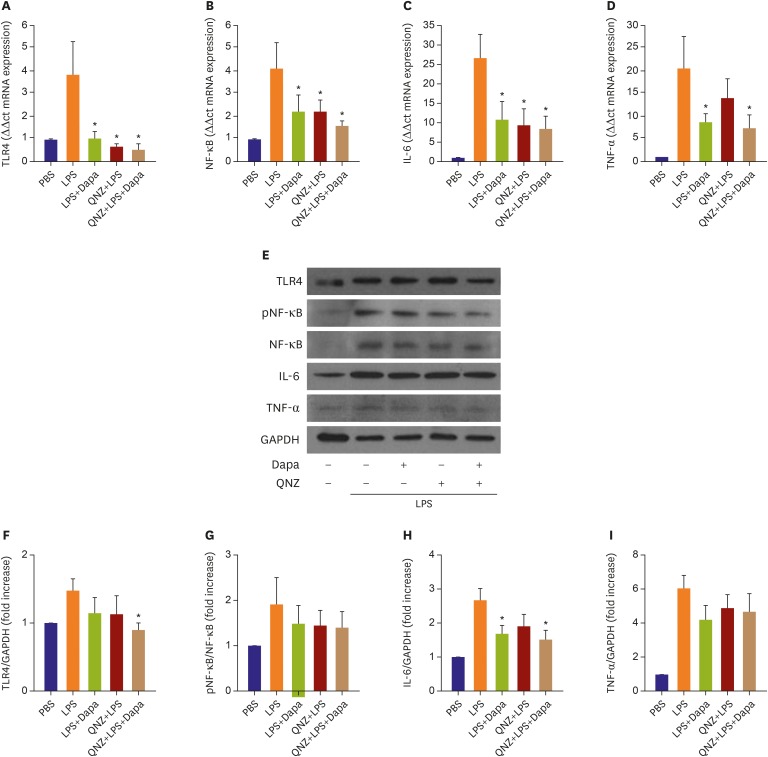
Atheroma burden (38.51±3.16% vs. 21.91±1.22%, p<0.01) and lipid accumulation (18.90±3.63% vs. 10.20±2.03%, p=0.047) was significantly decreased by SGLT-2 inhibitor treatment. The SGLT-2 inhibitor group showed lower macrophage infiltration (20.23±1.89% vs. 12.72±1.95%, p=0.01) as well as tumor necrosis factor (TNF)-α expression (31.17±4.40% vs. 19.47±2.10%, p=0.025). Relative area of inducible nitric oxide synthase+ macrophages was tended to be lower in the SGLT-2 inhibitor-treated group (1.00±0.16% vs. 0.71±0.10%, p=0.13), while relative proportion of Arg1⺠macrophage was markedly increased (1.00±0.27% vs. 2.43±0.64%, p=0.04). As a result, progression of atherosclerosis was markedly attenuated in SGLT-2 inhibitor treated group (OCT area stenosis, 32.13±1.20% vs. 22.77±0.88%, p<0.01). Mechanistically, SGLT-2 treatment mitigated the inflammatory responses in macrophage. Especially, Toll-like receptor 4/nuclear factor-kappa B signaling pathway, and their downstream effectors such as interleukin-6 and TNF-α were markedly suppressed by SGLT-2 inhibitor treatment.
CONCLUSIONS
These results together suggest that SGLT-2 inhibitor exerts an anti-atherosclerotic effect through favorable modulation of inflammatory response as well as macrophage characteristics in non-diabetic situation.
Keyword
MeSH Terms
Figure
Cited by 1 articles
-
Heart Failure with Preserved Ejection Fraction: the Major Unmet Need in Cardiology
Chi Young Shim
Korean Circ J. 2020;50(12):1051-1061. doi: 10.4070/kcj.2020.0338.
Reference
-
1. Murray CJ, Lopez AD. Measuring the global burden of disease. N Engl J Med. 2013; 369:448–457. PMID: 23902484.2. Libby P. Inflammation in atherosclerosis. Nature. 2002; 420:868–874. PMID: 12490960.3. Glass CK, Witztum JL. Atherosclerosis. The road ahead. Cell. 2001; 104:503–516. PMID: 11239408.4. Allahverdian S, Pannu PS, Francis GA. Contribution of monocyte-derived macrophages and smooth muscle cells to arterial foam cell formation. Cardiovasc Res. 2012; 95:165–172. PMID: 22345306.5. Rieg T, Masuda T, Gerasimova M, et al. Increase in SGLT1-mediated transport explains renal glucose reabsorption during genetic and pharmacological SGLT2 inhibition in euglycemia. Am J Physiol Renal Physiol. 2014; 306:F188–93. PMID: 24226519.6. Ferrannini E, Solini A. SGLT2 inhibition in diabetes mellitus: rationale and clinical prospects. Nat Rev Endocrinol. 2012; 8:495–502. PMID: 22310849.7. Heerspink HJ, Perkins BA, Fitchett DH, Husain M, Cherney DZ. Sodium glucose cotransporter 2 inhibitors in the treatment of diabetes mellitus: cardiovascular and kidney effects, potential mechanisms, and clinical applications. Circulation. 2016; 134:752–772. PMID: 27470878.8. Bhartia M, Tahrani AA, Barnett AH. SGLT-2 inhibitors in development for type 2 diabetes treatment. Rev Diabet Stud. 2011; 8:348–354. PMID: 22262072.9. Abdul-Ghani M, Del Prato S, Chilton R, DeFronzo RA. SGLT2 inhibitors and cardiovascular risk: lessons learned from the EMPA-REG OUTCOME study. Diabetes Care. 2016; 39:717–725. PMID: 27208375.10. Henry RR, Rosenstock J, Edelman S, et al. Exploring the potential of the SGLT2 inhibitor dapagliflozin in type 1 diabetes: a randomized, double-blind, placebo-controlled pilot study. Diabetes Care. 2015; 38:412–419. PMID: 25271207.11. Han JH, Oh TJ, Lee G, et al. The beneficial effects of empagliflozin, an SGLT2 inhibitor, on atherosclerosis in ApoE −/− mice fed a western diet. Diabetologia. 2017; 60:364–376. PMID: 27866224.12. Terasaki M, Hiromura M, Mori Y, et al. Amelioration of hyperglycemia with a sodium-glucose cotransporter 2 inhibitor prevents macrophage-driven atherosclerosis through macrophage foam cell formation suppression in type 1 and type 2 diabetic mice. PLoS One. 2015; 10:e0143396. PMID: 26606676.13. Leng W, Ouyang X, Lei X, et al. The SGLT-2 inhibitor dapagliflozin has a therapeutic effect on atherosclerosis in diabetic ApoE−/− mice. Mediators Inflamm. 2016; 2016:6305735. PMID: 28104929.14. Kim JS, Lee SG, Oh J, et al. Development of advanced atherosclerotic plaque by injection of inflammatory proteins in a rabbit iliac artery model. Yonsei Med J. 2016; 57:1095–1105. PMID: 27401639.15. Lee SG, Lee SJ, Thuy NV, et al. Synergistic protective effects of a statin and an angiotensin receptor blocker for initiation and progression of atherosclerosis. PLoS One. 2019; 14:e0215604. PMID: 31050669.16. Tsunoda F, Asztalos IB, Horvath KV, Steiner G, Schaefer EJ, Asztalos BF. Fenofibrate, HDL, and cardiovascular disease in type-2 diabetes: the DAIS trial. Atherosclerosis. 2016; 247:35–39. PMID: 26854974.17. Kohan DE, Fioretto P, Tang W, List JF. Long-term study of patients with type 2 diabetes and moderate renal impairment shows that dapagliflozin reduces weight and blood pressure but does not improve glycemic control. Kidney Int. 2014; 85:962–971. PMID: 24067431.18. Marx N, McGuire DK. Sodium-glucose cotransporter-2 inhibition for the reduction of cardiovascular events in high-risk patients with diabetes mellitus. Eur Heart J. 2016; 37:3192–3200. PMID: 27153861.19. Chinetti-Gbaguidi G, Colin S, Staels B. Macrophage subsets in atherosclerosis. Nat Rev Cardiol. 2015; 12:10–17. PMID: 25367649.20. Peled M, Fisher EA. Dynamic aspects of macrophage polarization during atherosclerosis progression and regression. Front Immunol. 2014; 5:579. PMID: 25429291.21. Rőszer T. Understanding the mysterious M2 macrophage through activation markers and effector mechanisms. Mediators Inflamm. 2015; 2015:816460. PMID: 26089604.22. Pourcet B, Pineda-Torra I. Transcriptional regulation of macrophage arginase 1 expression and its role in atherosclerosis. Trends Cardiovasc Med. 2013; 23:143–152. PMID: 23375628.23. McKellar GE, McCarey DW, Sattar N, McInnes IB. Role for TNF in atherosclerosis? Lessons from autoimmune disease. Nat Rev Cardiol. 2009; 6:410–417. PMID: 19421244.24. Moriya J. Critical roles of inflammation in atherosclerosis. J Cardiol. 2019; 73:22–27. PMID: 29907363.25. Xu C, Wang W, Zhong J, et al. Canagliflozin exerts anti-inflammatory effects by inhibiting intracellular glucose metabolism and promoting autophagy in immune cells. Biochem Pharmacol. 2018; 152:45–59. PMID: 29551587.26. Mancini SJ, Boyd D, Katwan OJ, et al. Canagliflozin inhibits interleukin-1β-stimulated cytokine and chemokine secretion in vascular endothelial cells by AMP-activated protein kinase-dependent and -independent mechanisms. Sci Rep. 2018; 8:5276. PMID: 29588466.27. Yan ZQ. Regulation of TLR4 expression is a tale about tail. Arterioscler Thromb Vasc Biol. 2006; 26:2582–2584. PMID: 17110607.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- The Side Effects of Sodium Glucose Cotransporter 2 (SGLT2) Inhibitor
- Sodium-Glucose Cotransporter 2 Inhibitors for People with Type 1 Diabetes
- Sodium Glucose Cotransporter-2 Inhibitors as an Add-on Therapy to Metformin Plus Dipeptidyl Peptidase-4 Inhibitor in Patients with Type 2 Diabetes
- Comparative Effects of Sodium-Glucose Cotransporter 2 Inhibitor and Thiazolidinedione Treatment on Risk of Stroke among Patients with Type 2 Diabetes Mellitus
- Cardiovascular Outcome Trials of Sodium Glucose Cotransporter 2 Inhibitor and Its Possible Cardioprotective Mechanism