J Gastric Cancer.
2019 Sep;19(3):254-277. 10.5230/jgc.2019.19.e29.
Biomarkers for Evaluating the Inflammation Status in Patients with Cancer
- Affiliations
-
- 1Department of Surgery, Yonsei University College of Medicine, Seoul, Korea. cairus@yuhs.ac
- 2Department of General Surgery, Faculty of Medicine, Karadeniz Technical University, Trabzon, Turkey.
- 3Department of Biostatistics and Medical Informatics, Institute of Medical Science, Karadeniz Technical University, Trabzon, Turkey.
- 4Open NBI Convergence Technology Research Laboratory, Severance Hospital, Yonsei University Health System, Seoul, Korea.
- 5Gastric Cancer Center, Yonsei Cancer Hospital; Seoul, Korea.
- KMID: 2458827
- DOI: http://doi.org/10.5230/jgc.2019.19.e29
Abstract
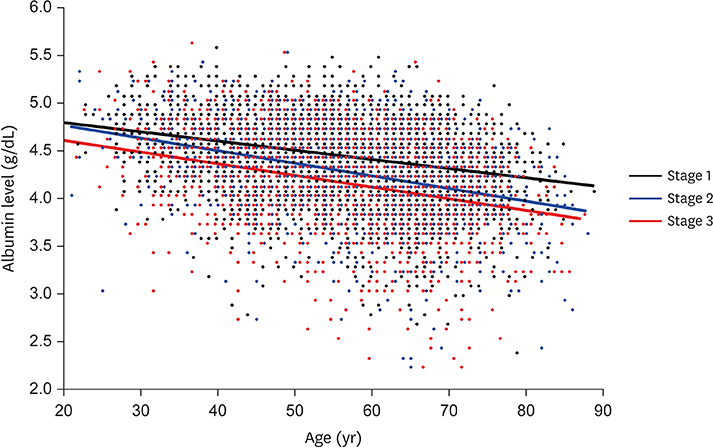
- Inflammation can be a causative factor for carcinogenesis or can result from a consequence of cancer progression. Moreover, cancer therapeutic interventions can also induce an inflammatory response. Various inflammatory parameters are used to assess the inflammatory status during cancer treatment. It is important to select the most optimal biomarker among these parameters. Additionally, suitable biomarkers must be examined if there are no known parameters. We briefly reviewed the published literature for the use of inflammatory parameters in the treatment of patients with cancer. Most studies on inflammation evaluated the correlation between host characteristics, effect of interventions, and clinical outcomes. Additionally, the levels of C-reactive protein, albumin, lymphocytes, and platelets were the most commonly used laboratory parameters, either independently or in combination with other laboratory parameters and clinical characteristics. Furthermore, the immune parameters are classically examined using flow cytometry, immunohistochemical staining, and enzyme-linked immunosorbent assay techniques. However, gene expression profiling can aid in assessing the overall peri-interventional immune status. The checklists of guidelines, such as STAndards for Reporting of Diagnostic accuracy and REporting recommendations for tumor MARKer prognostic studies should be considered when designing studies to investigate the inflammatory parameters. Finally, the data should be interpreted after adjusting for clinically important variables, such as age and cancer stage.
Keyword
MeSH Terms
Figure
Reference
-
1. Hensler T, Hecker H, Heeg K, Heidecke CD, Bartels H, Barthlen W, et al. Distinct mechanisms of immunosuppression as a consequence of major surgery. Infect Immun. 1997; 65:2283–2291.
Article2. Zeltsman M, Mayor M, Jones DR, Adusumilli PS. Surgical immune interventions for solid malignancies. Am J Surg. 2016; 212:682–690.e5.
Article3. Guner A, Kim SY, Yu JE, Min IK, Roh YH, Roh C, et al. Parameters for predicting surgical outcomes for gastric cancer patients: simple is better than complex. Ann Surg Oncol. 2018; 25:3239–3247.
Article4. Pennell LM, Galligan CL, Fish EN. Sex affects immunity. J Autoimmun. 2012; 38:J282–J291.
Article5. Roved J, Westerdahl H, Hasselquist D. Sex differences in immune responses: Hormonal effects, antagonistic selection, and evolutionary consequences. Horm Behav. 2017; 88:95–105.
Article6. Ono S, Tsujimoto H, Hiraki S, Takahata R, Kinoshita M, Mochizuki H. Sex differences in cytokine production and surface antigen expression of peripheral blood mononuclear cells after surgery. Am J Surg. 2005; 190:439–444.
Article7. Kosuga T, Ichikawa D, Okamoto K, Komatsu S, Konishi H, Takeshita H, et al. Impact of age on early surgical outcomes of laparoscopy-assisted gastrectomy with suprapancreatic nodal dissection for clinical stage I gastric cancer. Anticancer Res. 2015; 35:2191–2198.8. Kudoh A, Katagai H, Takazawa T, Matsuki A. Plasma proinflammatory cytokine response to surgical stress in elderly patients. Cytokine. 2001; 15:270–273.
Article9. Milner JJ, Beck MA. The impact of obesity on the immune response to infection. Proc Nutr Soc. 2012; 71:298–306.
Article10. Kolb R, Sutterwala FS, Zhang W. Obesity and cancer: inflammation bridges the two. Curr Opin Pharmacol. 2016; 29:77–89.
Article11. Gunderson CC, Java J, Moore KN, Walker JL. The impact of obesity on surgical staging, complications, and survival with uterine cancer: a Gynecologic Oncology Group LAP2 ancillary data study. Gynecol Oncol. 2014; 133:23–27.12. Khoury W, Lavery IC, Kiran RP. Effects of chronic immunosuppression on long-term oncologic outcomes for colorectal cancer patients undergoing surgery. Ann Surg. 2011; 253:323–327.
Article13. Moulin CM, Marguti I, Peron JP, Halpern A, Rizzo LV. Bariatric surgery reverses natural killer (NK) cell activity and NK-related cytokine synthesis impairment induced by morbid obesity. Obes Surg. 2011; 21:112–118.
Article14. Kotani N, Hashimoto H, Sessler DI, Yoshida H, Kimura N, Okawa H, et al. Smoking decreases alveolar macrophage function during anesthesia and surgery. Anesthesiology. 2000; 92:1268–1277.
Article15. Na YM, Kim MY, Kim YK, Ha YR, Yoon DS. Exercise therapy effect on natural killer cell cytotoxic activity in stomach cancer patients after curative surgery. Arch Phys Med Rehabil. 2000; 81:777–779.
Article16. Ukkonen M, Karlsson S, Laukkarinen J, Rantanen T, Paajanen H. Finnsepsis Study Group. Severe sepsis in elderly patients undergoing gastrointestinal surgery-a prospective multicenter follow-up study of Finnish Intensive Care Units. J Gastrointest Surg. 2016; 20:1028–1033.
Article17. Solaini L, Atmaja BT, Arumugam P, Hutchins RR, Abraham AT, Bhattacharya S, et al. The role of perioperative inflammatory-based prognostic systems in patients with colorectal liver metastases undergoing surgery. A cohort study. Int J Surg. 2016; 36:8–12.
Article18. Kudoh A, Katagai H, Takazawa T. Plasma inflammatory cytokine response to surgical trauma in chronic depressed patients. Cytokine. 2001; 13:104–108.
Article19. Sutter PM, Spagnoli GC, Marx A, Gürke L, Troeger H, Fricker R, et al. Increased surface expression of CD18 and CD11b in leukocytes after tourniquet ischemia during elective hand surgery. World J Surg. 1997; 21:179–184.
Article20. Weighardt H, Heidecke CD, Emmanuilidis K, Maier S, Bartels H, Siewert JR, et al. Sepsis after major visceral surgery is associated with sustained and interferon-gamma-resistant defects of monocyte cytokine production. Surgery. 2000; 127:309–315.21. Sammour T, Kahokehr A, Chan S, Booth RJ, Hill AG. The humoral response after laparoscopic versus open colorectal surgery: a meta-analysis. J Surg Res. 2010; 164:28–37.
Article22. Evans C, Galustian C, Kumar D, Hagger R, Melville DM, Bodman-Smith M, et al. Impact of surgery on immunologic function: comparison between minimally invasive techniques and conventional laparotomy for surgical resection of colorectal tumors. Am J Surg. 2009; 197:238–245.
Article23. Zawadzki M, Krzystek-Korpacka M, Gamian A, Witkiewicz W. Comparison of inflammatory responses following robotic and open colorectal surgery: a prospective study. Int J Colorectal Dis. 2017; 32:399–407.
Article24. Pilka R, Marek R, Adam T, Kudela M, Ondrová D, Neubert D, et al. Systemic inflammatory response after open, laparoscopic and robotic surgery in endometrial cancer patients. Anticancer Res. 2016; 36:2909–2922.25. Schneider C, von Aulock S, Zedler S, Schinkel C, Hartung T, Faist E. Perioperative recombinant human granulocyte colony-stimulating factor (Filgrastim) treatment prevents immunoinflammatory dysfunction associated with major surgery. Ann Surg. 2004; 239:75–81.
Article26. Crozier JE, Leitch EF, McKee RF, Anderson JH, Horgan PG, McMillan DC. Relationship between emergency presentation, systemic inflammatory response, and cancer-specific survival in patients undergoing potentially curative surgery for colon cancer. Am J Surg. 2009; 197:544–549.
Article27. Kimura A, Ono S, Hiraki S, Takahata R, Tsujimoto H, Miyazaki H, et al. The postoperative serum interleukin-15 concentration correlates with organ dysfunction and the prognosis of septic patients following emergency gastrointestinal surgery. J Surg Res. 2012; 175:e83–e88.
Article28. Aosasa S, Ono S, Mochizuki H, Tsujimoto H, Osada S, Takayama E, et al. Activation of monocytes and endothelial cells depends on the severity of surgical stress. World J Surg. 2000; 24:10–16.
Article29. Flohé S, Lendemans S, Schade FU, Kreuzfelder E, Waydhas C. Influence of surgical intervention in the immune response of severely injured patients. Intensive Care Med. 2004; 30:96–102.
Article30. Gu CY, Zhang J, Qian YN, Tang QF. Effects of epidural anesthesia and postoperative epidural analgesia on immune function in esophageal carcinoma patients undergoing thoracic surgery. Mol Clin Oncol. 2015; 3:190–196.
Article31. Chen WK, Ren L, Wei Y, Zhu DX, Miao CH, Xu JM. General anesthesia combined with epidural anesthesia ameliorates the effect of fast-track surgery by mitigating immunosuppression and facilitating intestinal functional recovery in colon cancer patients. Int J Colorectal Dis. 2015; 30:475–481.
Article32. Sacerdote P, Bianchi M, Gaspani L, Manfredi B, Maucione A, Terno G, et al. The effects of tramadol and morphine on immune responses and pain after surgery in cancer patients. Anesth Analg. 2000; 90:1411–1414.
Article33. Martínez AB, Longás J, Ramírez JM. A model for lymphocyte activation in open versus laparoscopic surgery in colorectal cancer patients in enhanced recovery after surgery (ERAS) protocols. Int J Colorectal Dis. 2017; 32:913–916.
Article34. Veenhof AA, Vlug MS, van der Pas MH, Sietses C, van der Peet DL, de Lange-de Klerk ES, et al. Surgical stress response and postoperative immune function after laparoscopy or open surgery with fast track or standard perioperative care: a randomized trial. Ann Surg. 2012; 255:216–221.35. Yang D, He W, Zhang S, Chen H, Zhang C, He Y. Fast-track surgery improves postoperative clinical recovery and immunity after elective surgery for colorectal carcinoma: randomized controlled clinical trial. World J Surg. 2012; 36:1874–1880.
Article36. Heiss MM, Fasol-Merten K, Allgayer H, Ströhlein MA, Tarabichi A, Wallner S, et al. Influence of autologous blood transfusion on natural killer and lymphokine-activated killer cell activities in cancer surgery. Vox Sang. 1997; 73:237–245.
Article37. Theodoraki K, Markatou M, Rizos D, Fassoulaki A. The impact of two different transfusion strategies on patient immune response during major abdominal surgery: a preliminary report. J Immunol Res. 2014; 2014:945829.
Article38. Fukuda T, Seto Y, Yamada K, Hiki N, Fukunaga T, Oyama S, et al. Can immune-enhancing nutrients reduce postoperative complications in patients undergoing esophageal surgery? Dis Esophagus. 2008; 21:708–711.
Article39. Giger U, Büchler M, Farhadi J, Berger D, Hüsler J, Schneider H, et al. Preoperative immunonutrition suppresses perioperative inflammatory response in patients with major abdominal surgery-a randomized controlled pilot study. Ann Surg Oncol. 2007; 14:2798–2806.
Article40. Arumugam S, Lau CS, Chamberlain RS. Probiotics and Synbiotics Decrease Postoperative Sepsis in Elective Gastrointestinal Surgical Patients: a Meta-Analysis. J Gastrointest Surg. 2016; 20:1123–1131.
Article41. Liu Z, Li C, Huang M, Tong C, Zhang X, Wang L, et al. Positive regulatory effects of perioperative probiotic treatment on postoperative liver complications after colorectal liver metastases surgery: a double-center and double-blind randomized clinical trial. BMC Gastroenterol. 2015; 15:34.
Article42. Braga M, Gianotti L, Vignali A, Di Carlo V. Immunonutrition in gastric cancer surgical patients. Nutrition. 1998; 14:831–835.
Article43. Furukawa K, Tashiro T, Yamamori H, Takagi K, Morishima Y, Sugiura T, et al. Effects of soybean oil emulsion and eicosapentaenoic acid on stress response and immune function after a severely stressful operation. Ann Surg. 1999; 229:255–261.
Article44. Wang WP, Yan XL, Ni YF, Guo K, Ke CK, Cheng QS, et al. Effects of lipid emulsions in parenteral nutrition of esophageal cancer surgical patients receiving enteral nutrition: a comparative analysis. Nutrients. 2013; 6:111–123.45. Schmidt SC, Hamann S, Langrehr JM, Höflich C, Mittler J, Jacob D, et al. Preoperative high-dose steroid administration attenuates the surgical stress response following liver resection: results of a prospective randomized study. J Hepatobiliary Pancreat Surg. 2007; 14:484–492.
Article46. Pratschke S, von Dossow-Hanfstingl V, Dietz J, Schneider CP, Tufman A, Albertsmeier M, et al. Dehydroepiandrosterone modulates T-cell response after major abdominal surgery. J Surg Res. 2014; 189:117–125.
Article47. Li H, Wang C, Yu J, Cao S, Wei F, Zhang W, et al. Dendritic cell-activated cytokine-induced killer cells enhance the anti-tumor effect of chemotherapy on non-small cell lung cancer in patients after surgery. Cytotherapy. 2009; 11:1076–1083.
Article48. Brivio F, Lissoni P, Gilardi R, Ferrante R, Vigore L, Curzi L, et al. Abrogation of surgery-induced decline in circulating dendritic cells by subcutaneous preoperative administration of IL-2 in operable cancer patients. J Biol Regul Homeost Agents. 2000; 14:200–203.49. Nishiyama J, Matsuda M, Ando S, Hirasawa M, Suzuki T, Makuuchi H. The effects of the early administration of sivelestat sodium, a selective neutrophil elastase inhibitor, on the postoperative course after radical surgery for esophageal cancer. Surg Today. 2012; 42:659–665.
Article50. Ono S, Aosasa S, Mochizuki H. Effects of a protease inhibitor on reduction of surgical stress in esophagectomy. Am J Surg. 1999; 177:78–82.
Article51. Kerr SF, Klonizakis M, Glynne-Jones R. Suppression of the postoperative neutrophil leucocytosis following neoadjuvant chemoradiotherapy for rectal cancer and implications for surgical morbidity. Colorectal Dis. 2010; 12:549–554.
Article52. Tanis E, Julié C, Emile JF, Mauer M, Nordlinger B, Aust D, et al. Prognostic impact of immune response in resectable colorectal liver metastases treated by surgery alone or surgery with perioperative FOLFOX in the randomised EORTC study 40983. Eur J Cancer. 2015; 51:2708–2717.
Article53. Westerterp M, Boermeester MA, Omloo JM, Hulshof MC, Vervenne WL, Lutter R, et al. Differential responses of cellular immunity in patients undergoing neoadjuvant therapy followed by surgery for carcinoma of the oesophagus. Cancer Immunol Immunother. 2008; 57:1837–1847.
Article54. Wang D, Yang XL, Chai XQ, Shu SH, Zhang XL, Xie YH, et al. A short-term increase of the postoperative naturally circulating dendritic cells subsets in flurbiprofen-treated patients with esophageal carcinoma undergoing thoracic surgery. Oncotarget. 2016; 7:18705–18712.
Article55. Liakopoulos OJ, Dörge H, Schmitto JD, Nagorsnik U, Grabedünkel J, Schoendube FA. Effects of preoperative statin therapy on cytokines after cardiac surgery. Thorac Cardiovasc Surg. 2006; 54:250–254.
Article56. Amar D, Zhang H, Park B, Heerdt PM, Fleisher M, Thaler HT. Inflammation and outcome after general thoracic surgery. Eur J Cardiothorac Surg. 2007; 32:431–434.
Article57. De Lorenzo A, Pittella F, Rocha A. Increased preoperative C-reactive protein levels are associated with inhospital death after coronary artery bypass surgery. Inflammation. 2012; 35:1179–1183.
Article58. Ishizuka M, Kubota K, Kita J, Shimoda M, Kato M, Sawada T. Usefulness of a modified inflammation-based prognostic system for predicting postoperative mortality of patients undergoing surgery for primary hepatocellular carcinoma. J Surg Oncol. 2011; 103:801–806.
Article59. Josse JM, Cleghorn MC, Ramji KM, Jiang H, Elnahas A, Jackson TD, et al. The neutrophil-to-lymphocyte ratio predicts major perioperative complications in patients undergoing colorectal surgery. Colorectal Dis. 2016; 18:O236–O242.
Article60. Mokart D, Capo C, Blache JL, Delpero JR, Houvenaeghel G, Martin C, et al. Early postoperative compensatory anti-inflammatory response syndrome is associated with septic complications after major surgical trauma in patients with cancer. Br J Surg. 2002; 89:1450–1456.
Article61. Rettig TC, Verwijmeren L, Dijkstra IM, Boerma D, van de Garde EM, Noordzij PG. Postoperative interleukin-6 level and early detection of complications after elective major abdominal surgery. Ann Surg. 2016; 263:1207–1212.
Article62. Saeed K, Dale AP, Leung E, Cusack T, Mohamed F, Lockyer G, et al. Procalcitonin levels predict infectious complications and response to treatment in patients undergoing cytoreductive surgery for peritoneal malignancy. Eur J Surg Oncol. 2016; 42:234–243.
Article63. Weighardt H, Heidecke CD, Westerholt A, Emmanuilidis K, Maier S, Veit M, et al. Impaired monocyte IL-12 production before surgery as a predictive factor for the lethal outcome of postoperative sepsis. Ann Surg. 2002; 235:560–567.
Article64. Anitei MG, Zeitoun G, Mlecnik B, Marliot F, Haicheur N, Todosi AM, et al. Prognostic and predictive values of the immunoscore in patients with rectal cancer. Clin Cancer Res. 2014; 20:1891–1899.
Article65. Matsutani S, Shibutani M, Maeda K, Nagahara H, Fukuoka T, Nakao S, et al. Significance of tumor-infiltrating lymphocytes before and after neoadjuvant therapy for rectal cancer. Cancer Sci. 2018; 109:966–979.
Article66. Ishizuka M, Nagata H, Takagi K, Iwasaki Y, Kubota K. Systemic inflammatory response predicts perioperative central venous catheter-related bloodstream infection in patients Undergoing colorectal cancer surgery with administration of parenteral nutrition. Anticancer Res. 2012; 32:4045–4050.67. Strohmeyer JC, Blume C, Meisel C, Doecke WD, Hummel M, Hoeflich C, et al. Standardized immune monitoring for the prediction of infections after cardiopulmonary bypass surgery in risk patients. Cytometry B Clin Cytom. 2003; 53:54–62.
Article68. Song B, Zhen S, Meng F. T cell inflammation profile after surgical resection may predict tumor recurrence in HBV-related hepatocellular carcinoma. Int Immunopharmacol. 2016; 41:35–41.
Article69. Chan AW, Chan SL, Wong GL, Wong VW, Chong CC, Lai PB, et al. Prognostic nutritional index (PNI) predicts tumor recurrence of very early/early stage hepatocellular carcinoma after surgical resection. Ann Surg Oncol. 2015; 22:4138–4148.
Article70. Lindenmann J, Fink-Neuboeck N, Avian A, Pichler M, Habitzruther M, Maier A, et al. Preoperative Glasgow prognostic score as additional independent prognostic parameter for patients with esophageal cancer after curative esophagectomy. Eur J Surg Oncol. 2017; 43:445–453.
Article71. Toiyama Y, Inoue Y, Saigusa S, Kawamura M, Kawamoto A, Okugawa Y, et al. C-reactive protein as predictor of recurrence in patients with rectal cancer undergoing chemoradiotherapy followed by surgery. Anticancer Res. 2013; 33:5065–5074.72. Wei IH, Harmon CM, Arcerito M, Cheng DF, Minter RM, Simeone DM. Tumor-associated macrophages are a useful biomarker to predict recurrence after surgical resection of nonfunctional pancreatic neuroendocrine tumors. Ann Surg. 2014; 260:1088–1094.
Article73. Galizia G, Lieto E, Auricchio A, Cardella F, Mabilia A, Podzemny V, et al. Naples prognostic score, based on nutritional and inflammatory status, is an independent predictor of long-term outcome in patients undergoing surgery for colorectal cancer. Dis Colon Rectum. 2017; 60:1273–1284.
Article74. He YF, Luo HQ, Wang W, Chen J, Yao YW, Yan Y, et al. Preoperative NLR and PLR in the middle or lower ESCC patients with radical operation. Eur J Cancer Care (Engl). 2017; 26:e12445.
Article75. Ishizuka M, Nagata H, Takagi K, Iwasaki Y, Shibuya N, Kubota K. Clinical significance of the C-reactive protein to albumin ratio for survival after surgery for colorectal cancer. Ann Surg Oncol. 2016; 23:900–907.
Article76. Ishizuka M, Oyama Y, Abe A, Kubota K. Combination of platelet count and neutrophil to lymphocyte ratio is a useful predictor of postoperative survival in patients undergoing surgery for gastric cancer. J Surg Oncol. 2014; 110:935–941.
Article77. Malietzis G, Giacometti M, Askari A, Nachiappan S, Kennedy RH, Faiz OD, et al. A preoperative neutrophil to lymphocyte ratio of 3 predicts disease-free survival after curative elective colorectal cancer surgery. Ann Surg. 2014; 260:287–292.
Article78. Mimatsu K, Fukino N, Ogasawara Y, Saino Y, Oida T. Utility of inflammatory marker- and nutritional status-based prognostic factors for predicting the prognosis of stage IV gastric cancer patients undergoing non-curative surgery. Anticancer Res. 2017; 37:4215–4222.
Article79. Watt DG, Martin JC, Park JH, Horgan PG, McMillan DC. Neutrophil count is the most important prognostic component of the differential white cell count in patients undergoing elective surgery for colorectal cancer. Am J Surg. 2015; 210:24–30.
Article80. Yamamoto T, Yanagimoto H, Satoi S, Toyokawa H, Yamao J, Kim S, et al. Circulating myeloid dendritic cells as prognostic factors in patients with pancreatic cancer who have undergone surgical resection. J Surg Res. 2012; 173:299–308.
Article81. Zikos TA, Donnenberg AD, Landreneau RJ, Luketich JD, Donnenberg VS. Lung T-cell subset composition at the time of surgical resection is a prognostic indicator in non-small cell lung cancer. Cancer Immunol Immunother. 2011; 60:819–827.
Article82. Jin Z, Li R, Liu J, Lin J. Long-term prognosis after cancer surgery with inhalational anesthesia and total intravenous anesthesia: a systematic review and meta-analysis. Int J Physiol Pathophysiol Pharmacol. 2019; 11:83–94.83. Weng M, Chen W, Hou W, Li L, Ding M, Miao C. The effect of neuraxial anesthesia on cancer recurrence and survival after cancer surgery: an updated meta-analysis. Oncotarget. 2016; 7:15262–15273.
Article84. Giger-Pabst U, Lange J, Maurer C, Bucher C, Schreiber V, Schlumpf R, et al. Short-term preoperative supplementation of an immunoenriched diet does not improve clinical outcome in well-nourished patients undergoing abdominal cancer surgery. Nutrition. 2013; 29:724–729.
Article85. Klek S, Sierzega M, Szybinski P, Szczepanek K, Scislo L, Walewska E, et al. The immunomodulating enteral nutrition in malnourished surgical patients - a prospective, randomized, double-blind clinical trial. Clin Nutr. 2011; 30:282–288.
Article86. Chen L, Sun L, Lang Y, Wu J, Yao L, Ning J, et al. Fast-track surgery improves postoperative clinical recovery and cellular and humoral immunity after esophagectomy for esophageal cancer. BMC Cancer. 2016; 16:449.
Article87. Liu HT, Huang YC, Cheng SB, Huang YT, Lin PT. Effects of coenzyme Q10 supplementation on antioxidant capacity and inflammation in hepatocellular carcinoma patients after surgery: a randomized, placebo-controlled trial. Nutr J. 2016; 15:85.
Article88. Parolari A, Camera M, Alamanni F, Naliato M, Polvani GL, Agrifoglio M, et al. Systemic inflammation after on-pump and off-pump coronary bypass surgery: a one-month follow-up. Ann Thorac Surg. 2007; 84:823–828.
Article89. Papadima A, Boutsikou M, Lagoudianakis EE, Kataki A, Konstadoulakis M, Georgiou L, et al. Lymphocyte apoptosis after major abdominal surgery is not influenced by anesthetic technique: a comparative study of general anesthesia versus combined general and epidural analgesia. J Clin Anesth. 2009; 21:414–421.
Article90. Reisinger KW, Derikx JP, van Vugt JL, Von Meyenfeldt MF, Hulsewé KW, Olde Damink SW, et al. Sarcopenia is associated with an increased inflammatory response to surgery in colorectal cancer. Clin Nutr. 2016; 35:924–927.
Article91. Buttenschoen K, Schneider ME, Utz K, Kornmann M, Beger HG, Carli Buttenschoen D. Effect of major abdominal surgery on endotoxin release and expression of Toll-like receptors 2/4. Langenbecks Arch Surg. 2009; 394:293–302.
Article92. Brix-Christensen V, Tønnesen E, Sørensen IJ, Bilfinger TV, Sanchez RG, Stefano GB. Effects of anaesthesia based on high versus low doses of opioids on the cytokine and acute-phase protein responses in patients undergoing cardiac surgery. Acta Anaesthesiol Scand. 1998; 42:63–70.
Article93. Greco F, Hoda MR, Wagner S, Reichelt O, Inferrera A, Fischer K, et al. Adipocytokine: a new family of inflammatory and immunologic markers of invasiveness in major urologic surgery. Eur Urol. 2010; 58:781–787.
Article94. Iwasaki A, Shirakusa T, Maekawa T, Enatsu S, Maekawa S. Clinical evaluation of systemic inflammatory response syndrome (SIRS) in advanced lung cancer (T3 and T4) with surgical resection. Eur J Cardiothorac Surg. 2005; 27:14–18.
Article95. Bruce DM, Smith M, Walker CB, Heys SD, Binnie NR, Gough DB, et al. Minimal access surgery for cholelithiasis induces an attenuated acute phase response. Am J Surg. 1999; 178:232–234.
Article96. Mokart D, Merlin M, Sannini A, Brun JP, Delpero JR, Houvenaeghel G, et al. Procalcitonin, interleukin 6 and systemic inflammatory response syndrome (SIRS): early markers of postoperative sepsis after major surgery. Br J Anaesth. 2005; 94:767–773.
Article97. Karth GD, Buberl A, Nikfardjam M, Meyer B, Wollenek G, Grimm M, et al. Role of amiodarone on the systemic inflammatory response induced by cardiac surgery: proinflammatory actions. Can J Anaesth. 2007; 54:262–268.
Article98. Ni XC, Yi Y, Fu YP, He HW, Cai XY, Wang JX, et al. Prognostic value of the modified Glasgow prognostic score in patients undergoing radical surgery for hepatocellular carcinoma. Medicine (Baltimore). 2015; 94:e1486.
Article99. Ji F, Liang Y, Fu SJ, Guo ZY, Shu M, Shen SL, et al. A novel and accurate predictor of survival for patients with hepatocellular carcinoma after surgical resection: the neutrophil to lymphocyte ratio (NLR) combined with the aspartate aminotransferase/platelet count ratio index (APRI). BMC Cancer. 2016; 16:137.
Article100. Dias Rodrigues V, Barroso de Pinho N, Abdelhay E, Viola JP, Correia MI, Brum Martucci R. Nutrition and immune-modulatory intervention in surgical patients with gastric cancer. Nutr Clin Pract. 2017; 32:122–129.
Article101. Sun KY, Xu JB, Chen SL, Yuan YJ, Wu H, Peng JJ, et al. Novel immunological and nutritional-based prognostic index for gastric cancer. World J Gastroenterol. 2015; 21:5961–5971.
Article102. Xie X, Luo KJ, Hu Y, Wang JY, Chen J. Prognostic value of preoperative platelet-lymphocyte and neutrophil-lymphocyte ratio in patients undergoing surgery for esophageal squamous cell cancer. Dis Esophagus. 2016; 29:79–85.
Article103. Liao R, Jiang N, Tang ZW, Li W, Huang P, Luo SQ, et al. Systemic and intratumoral balances between monocytes/macrophages and lymphocytes predict prognosis in hepatocellular carcinoma patients after surgery. Oncotarget. 2016; 7:30951–30961.
Article104. Hyun MH, Lee CH, Kwon YJ, Cho SI, Jang YJ, Kim DH, et al. Robot versus laparoscopic gastrectomy for cancer by an experienced surgeon: comparisons of surgery, complications, and surgical stress. Ann Surg Oncol. 2013; 20:1258–1265.
Article105. Hsu JT, Wang CC, Le PH, Chen TH, Kuo CJ, Lin CJ, et al. Lymphocyte-to-monocyte ratios predict gastric cancer surgical outcomes. J Surg Res. 2016; 202:284–290.
Article106. Pang S, Zhou Z, Yu X, Wei S, Chen Q, Nie S, et al. The predictive value of integrated inflammation scores in the survival of patients with resected hepatocellular carcinoma: a retrospective cohort study. Int J Surg. 2017; 42:170–177.
Article107. Jain S, Gautam V, Naseem S. Acute-phase proteins: As diagnostic tool. J Pharm Bioallied Sci. 2011; 3:118–127.
Article108. Warschkow R, Tarantino I, Ukegjini K, Beutner U, Müller SA, Schmied BM, et al. Diagnostic study and meta-analysis of C-reactive protein as a predictor of postoperative inflammatory complications after gastroesophageal cancer surgery. Langenbecks Arch Surg. 2012; 397:727–736.
Article109. Warschkow R, Ukegjini K, Tarantino I, Steffen T, Müller SA, Schmied BM, et al. Diagnostic study and meta-analysis of C-reactive protein as a predictor of postoperative inflammatory complications after pancreatic surgery. J Hepatobiliary Pancreat Sci. 2012; 19:492–500.
Article110. Kim S, McClave SA, Martindale RG, Miller KR, Hurt RT. Hypoalbuminemia and Clinical Outcomes: What is the Mechanism behind the Relationship? Am Surg. 2017; 83:1220–1227.
Article111. Iwaku A, Kinoshita A, Onoda H, Fushiya N, Nishino H, Matsushima M, et al. The Glasgow prognostic score accurately predicts survival in patients with biliary tract cancer not indicated for surgical resection. Med Oncol. 2014; 31:787.
Article112. Dupré A, Malik HZ. Inflammation and cancer: what a surgical oncologist should know. Eur J Surg Oncol. 2018; 44:566–570.113. Roxburgh CS, Salmond JM, Horgan PG, Oien KA, McMillan DC. The relationship between the local and systemic inflammatory responses and survival in patients undergoing curative surgery for colon and rectal cancers. J Gastrointest Surg. 2009; 13:2011–2018.
Article114. Guner A, Kim HI. ASO Author Reflections: Parameters for Predicting Surgical Outcomes for Gastric Cancer Patients: Simple Is Better Than Complex. Ann Surg Oncol. 2018; 25:699–700.
Article115. Lee JY, Kim HI, Kim YN, Hong JH, Alshomimi S, An JY, et al. Clinical significance of the prognostic nutritional index for predicting short- and long-term surgical outcomes after gastrectomy: a retrospective analysis of 7781 gastric cancer patients. Medicine (Baltimore). 2016; 95:e3539.116. Kohira S, Oka N, Inoue N, Itatani K, Hanayama N, Kitamura T, et al. Effect of the neutrophil elastase inhibitor sivelestat on perioperative inflammatory response after pediatric heart surgery with cardiopulmonary bypass: a prospective randomized study. Artif Organs. 2013; 37:1027–1033.
Article117. Ng CS, Lee TW, Wan S, Wan IY, Sihoe AD, Arifi AA, et al. Thoracotomy is associated with significantly more profound suppression in lymphocytes and natural killer cells than video-assisted thoracic surgery following major lung resections for cancer. J Invest Surg. 2005; 18:81–88.118. Volk T, Schenk M, Voigt K, Tohtz S, Putzier M, Kox WJ. Postoperative epidural anesthesia preserves lymphocyte, but not monocyte, immune function after major spine surgery. Anesth Analg. 2004; 98:1086–1092.
Article119. Ammendola M, Sacco R, Zuccalà V, Luposella M, Patruno R, Gadaleta P, et al. Mast cells density positive to tryptase correlate with microvascular density in both primary gastric cancer tissue and loco-regional lymph node metastases from patients that have undergone radical surgery. Int J Mol Sci. 2016; 17:1905.
Article120. Decker D, Tolba R, Springer W, Lauschke H, Hirner A, von Ruecker A. Abdominal surgical interventions: local and systemic consequences for the immune system--a prospective study on elective gastrointestinal surgery. J Surg Res. 2005; 126:12–18.121. Leal-Noval SR, Muñoz-Gómez M, Arellano V, Adsuar A, Jiménez-Sánchez M, Corcia Y, et al. Influence of red blood cell transfusion on CD4+ T-helper cells immune response in patients undergoing cardiac surgery. J Surg Res. 2010; 164:43–49.122. Matsuda A, Furukawa K, Takasaki H, Suzuki H, Kan H, Tsuruta H, et al. Preoperative oral immune-enhancing nutritional supplementation corrects Th1/Th2 imbalance in patients undergoing elective surgery for colorectal cancer. Dis Colon Rectum. 2006; 49:507–516.
Article123. Kirman I, Belizon A, Balik E, Feingold D, Arnell T, Horst P, et al. Perioperative sargramostim (recombinant human GM-CSF) induces an increase in the level of soluble VEGFR1 in colon cancer patients undergoing minimally invasive surgery. Eur J Surg Oncol. 2007; 33:1169–1176.
Article124. Crucitti A, Corbi M, Tomaiuolo PM, Fanali C, Mazzari A, Lucchetti D, et al. Laparoscopic surgery for colorectal cancer is not associated with an increase in the circulating levels of several inflammation-related factors. Cancer Biol Ther. 2015; 16:671–677.
Article125. Spittler A, Sautner T, Gornikiewicz A, Manhart N, Oehler R, Bergmann M, et al. Postoperative glycyl-glutamine infusion reduces immunosuppression: partial prevention of the surgery induced decrease in HLA-DR expression on monocytes. Clin Nutr. 2001; 20:37–42.
Article126. Welters ID, Feurer MK, Preiss V, Müller M, Scholz S, Kwapisz M, et al. Continuous S-(+)-ketamine administration during elective coronary artery bypass graft surgery attenuates pro-inflammatory cytokine response during and after cardiopulmonary bypass. Br J Anaesth. 2011; 106:172–179.127. Ikuta S, Miki C, Hatada T, Inoue Y, Araki T, Tanaka K, et al. Allogenic blood transfusion is an independent risk factor for infective complications after less invasive gastrointestinal surgery. Am J Surg. 2003; 185:188–193.
Article128. Leijte GP, Custers H, Gerretsen J, Heijne A, Roth J, Vogl T, et al. Increased plasma levels of danger-associated molecular patterns are associated with immune suppression and postoperative infections in patients undergoing cytoreductive surgery and hyperthermic intraperitoneal chemotherapy. Front Immunol. 2018; 9:663.
Article129. Schilling T, Kozian A, Senturk M, Huth C, Reinhold A, Hedenstierna G, et al. Effects of volatile and intravenous anesthesia on the alveolar and systemic inflammatory response in thoracic surgical patients. Anesthesiology. 2011; 115:65–74.
Article130. Zak-Nejmark T, Jankowska R, Passowicz-Muszynska E, Malolepszy J, Marciniak M, Jonkisz A, et al. Skin reactivity to histamine and expression of histamine receptors mRNA in lymphocytes of healthy subjects and non-small-cell lung cancer patients before and after surgery. Lung Cancer. 2004; 45:31–38.
Article131. Leaver HA, Craig SR, Yap PL, Walker WS. Lymphocyte responses following open and minimally invasive thoracic surgery. Eur J Clin Invest. 2000; 30:230–238.
Article132. Qadan M, Battista C, Gardner SA, Anderson G, Akca O, Polk HC Jr. Oxygen and surgical site infection: a study of underlying immunologic mechanisms. Anesthesiology. 2010; 113:369–377.133. Kim HI, Kim H, Cho HW, Kim SY, Song KJ, Hyung WJ, et al. The ratio of intra-tumoral regulatory T cells (Foxp3+)/helper T cells (CD4+) is a prognostic factor and associated with recurrence pattern in gastric cardia cancer. J Surg Oncol. 2011; 104:728–733.
Article134. Lee JY, Son T, Cheong JH, Hyung WJ, Noh SH, Kim CB, et al. Association between chemotherapy-response assays and subsets of tumor-infiltrating lymphocytes in gastric cancer: a pilot study. J Gastric Cancer. 2015; 15:223–230.
Article135. Lee S, Choi S, Kim SY, Yun MJ, Kim HI. Potential utility of FDG PET-CT as a non-invasive tool for monitoring local immune responses. J Gastric Cancer. 2017; 17:384–393.
Article136. Zhuang Y, Peng LS, Zhao YL, Shi Y, Mao XH, Chen W, et al. CD8+ T cells that produce interleukin-17 regulate myeloid-derived suppressor cells and are associated with survival time of patients with gastric cancer. Gastroenterology. 2012; 143:951–962.e8.137. Gérard A, Beemiller P, Friedman RS, Jacobelli J, Krummel MF. Evolving immune circuits are generated by flexible, motile, and sequential immunological synapses. Immunol Rev. 2013; 251:80–96.
Article138. Xie J, Tato CM, Davis MM. How the immune system talks to itself: the varied role of synapses. Immunol Rev. 2013; 251:65–79.
Article139. Annunziato F, Romagnani C, Romagnani S. The 3 major types of innate and adaptive cell-mediated effector immunity. J Allergy Clin Immunol. 2015; 135:626–635.
Article140. Romagnani S. T-cell subsets (Th1 versus Th2). Ann Allergy Asthma Immunol. 2000; 85:9–18.
Article141. Moraga I, Spangler J, Mendoza JL, Garcia KC. Multifarious determinants of cytokine receptor signaling specificity. Adv Immunol. 2014; 121:1–39.
Article142. Miller MC, Mayo KH. Chemokines from a structural perspective. Int J Mol Sci. 2017; 18:18.
Article143. Lin E, Calvano SE, Lowry SF. Inflammatory cytokines and cell response in surgery. Surgery. 2000; 127:117–126.
Article144. Cavaillon JM, Singer M. Inflammation: From Molecular and Cellular Mechanisms to the Clinic. Weinheim: Wiley-VCH;2017.145. Datta J, Berk E, Xu S, Fitzpatrick E, Rosemblit C, Lowenfeld L, et al. Anti-HER2 CD4+ T-helper type 1 response is a novel immune correlate to pathologic response following neoadjuvant therapy in HER2-positive breast cancer. Breast Cancer Res. 2015; 17:71.
Article146. Kvarnström A, Swartling T, Kurlberg G, Bengtson JP, Bengtsson A. Pro-inflammatory cytokine release in rectal surgery: comparison between laparoscopic and open surgical techniques. Arch Immunol Ther Exp (Warsz). 2013; 61:407–411.
Article147. Wu FP, Sietses C, von Blomberg BM, van Leeuwen PA, Meijer S, Cuesta MA. Systemic and peritoneal inflammatory response after laparoscopic or conventional colon resection in cancer patients: a prospective, randomized trial. Dis Colon Rectum. 2003; 46:147–155.148. Leung KL, Lai PB, Ho RL, Meng WC, Yiu RY, Lee JF, et al. Systemic cytokine response after laparoscopic-assisted resection of rectosigmoid carcinoma: a prospective randomized trial. Ann Surg. 2000; 231:506–511.149. Ahlers O, Nachtigall I, Lenze J, Goldmann A, Schulte E, Höhne C, et al. Intraoperative thoracic epidural anaesthesia attenuates stress-induced immunosuppression in patients undergoing major abdominal surgery. Br J Anaesth. 2008; 101:781–787.150. Sun HZ, Song YL, Wang XY. Effects of different anesthetic methods on cellular immune and neuroendocrine functions in patients with hepatocellular carcinoma before and after surgery. J Clin Lab Anal. 2016; 30:1175–1182.
Article151. Yeh CN, Lee HL, Liu YY, Chiang KC, Hwang TL, Jan YY, et al. The role of parenteral glutamine supplement for surgical patient perioperatively: result of a single center, prospective and controlled study. Langenbecks Arch Surg. 2008; 393:849–855.
Article152. Chen DW, Wei Fei Z, Zhang YC, Ou JM, Xu J. Role of enteral immunonutrition in patients with gastric carcinoma undergoing major surgery. Asian J Surg. 2005; 28:121–124.
Article153. Watt SK, Hasselbalch HC, Skov V, Kjær L, Thomassen M, Kruse TA, et al. Whole blood gene expression profiling in patients undergoing colon cancer surgery identifies differential expression of genes involved in immune surveillance, inflammation and carcinogenesis. Surg Oncol. 2018; 27:208–215.
Article154. Allen CJ, Griswold AJ, Schulman CI, Sleeman D, Levi JU, Livingstone AS, et al. Global gene expression change induced by major thoracoabdominal surgery. Ann Surg. 2017; 266:981–987.
Article155. Cancer Genome Atlas Research Network. Comprehensive molecular characterization of gastric adenocarcinoma. Nature. 2014; 513:202–209.156. Newman AM, Liu CL, Green MR, Gentles AJ, Feng W, Xu Y, et al. Robust enumeration of cell subsets from tissue expression profiles. Nat Methods. 2015; 12:453–457.
Article157. Altman DG, McShane LM, Sauerbrei W, Taube SE. Reporting Recommendations for Tumor Marker Prognostic Studies (REMARK): explanation and elaboration. PLoS Med. 2012; 9:e1001216.
Article158. Cohen JF, Korevaar DA, Altman DG, Bruns DE, Gatsonis CA, Hooft L, et al. STARD 2015 guidelines for reporting diagnostic accuracy studies: explanation and elaboration. BMJ Open. 2016; 6:e012799.
Article159. Welsch T, Müller SA, Ulrich A, Kischlat A, Hinz U, Kienle P, et al. C-reactive protein as early predictor for infectious postoperative complications in rectal surgery. Int J Colorectal Dis. 2007; 22:1499–1507.
Article160. Lee K, Hwang H, Nam KT. Immune response and the tumor microenvironment: how they communicate to regulate gastric cancer. Gut Liver. 2014; 8:131–139.
Article161. Kim CH, Park SM, Kim JJ. The impact of preoperative low body mass index on postoperative complications and long-term survival outcomes in gastric cancer patients. J Gastric Cancer. 2018; 18:274–286.
Article162. Seo HS, Jung YJ, Kim JH, Park CH, Kim IH, Lee HH. Long-term nutritional outcomes of near-total gastrectomy in gastric cancer treatment: a comparison with total gastrectomy using propensity score matching analysis. J Gastric Cancer. 2018; 18:189–199.
Article163. Lee HJ, Hyung WJ, Yang HK, Han SU, Park YK, An JY, et al. Short-term outcomes of a multicenter randomized controlled trial comparing laparoscopic distal gastrectomy with D2 lymphadenectomy to open distal gastrectomy for locally advanced gastric cancer (KLASS-02-RCT). Ann Surg. 2019.
Article164. Kim HH, Han SU, Kim MC, Kim W, Lee HJ, Ryu SW, et al. Effect of laparoscopic distal gastrectomy vs open distal gastrectomy on long-term survival among patients with stage I gastric cancer: The KLASS-01 Randomized Clinical Trial. JAMA Oncol. 2019; 5:506–513.165. Desiderio J, Stewart CL, Sun V, Melstrom L, Warner S, Lee B, et al. Enhanced recovery after surgery for gastric cancer patients improves clinical outcomes at a US Cancer Center. J Gastric Cancer. 2018; 18:230–241.
Article166. Mortensen K, Nilsson M, Slim K, Schäfer M, Mariette C, Braga M, et al. Consensus guidelines for enhanced recovery after gastrectomy: Enhanced Recovery After Surgery (ERAS®) Society recommendations. Br J Surg. 2014; 101:1209–1229.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Biomarkers of Sepsis
- Assessment of Asymptomatically Increased CA 19-9
- The severity of clinical symptoms according to cancer diagnosis in fever patients visiting the emergency department: a retrospective analysis
- Communicating clinical research to reduce cancer risk through diet: Walnuts as a case example
- Do we need a better marker for successful ovarian cancer surgery?