Korean J healthc assoc Infect Control Prev.
2019 Dec;24(2):52-59. 10.14192/kjicp.2019.24.2.52.
Prevalence and Risk Factors of Latent Tuberculosis Infection among Healthcare Workers
- Affiliations
-
- 1Department of Infectious Diseases, Ajou University School of Medicine, Suwon, Korea. yhwa1805@ajou.ac.kr
- 2Infection Control Unit, Ajou University Medical Center, Suwon, Korea.
- KMID: 2467904
- DOI: http://doi.org/10.14192/kjicp.2019.24.2.52
Abstract
- BACKGROUND
Due to occupational exposure, healthcare workers (HCW) face an increased risk of tuberculosis (TB) infection. This study was conducted to assess the prevalence and risk factors of latent tuberculosis infection (LTBI), and to estimate the cumulative risk of active TB among HCWs.
METHODS
We conducted a cross-sectional study among HCWs in Ajou university medical center. A standard questionnaire was used for data collection, and LTBI was detected using the Interferon gamma-release assay (IGRA). The biographical information was collected from the electronic database. A computerized algorithm was used to evaluate the predicted cumulative risk of active TB in HCWs with LTBI.
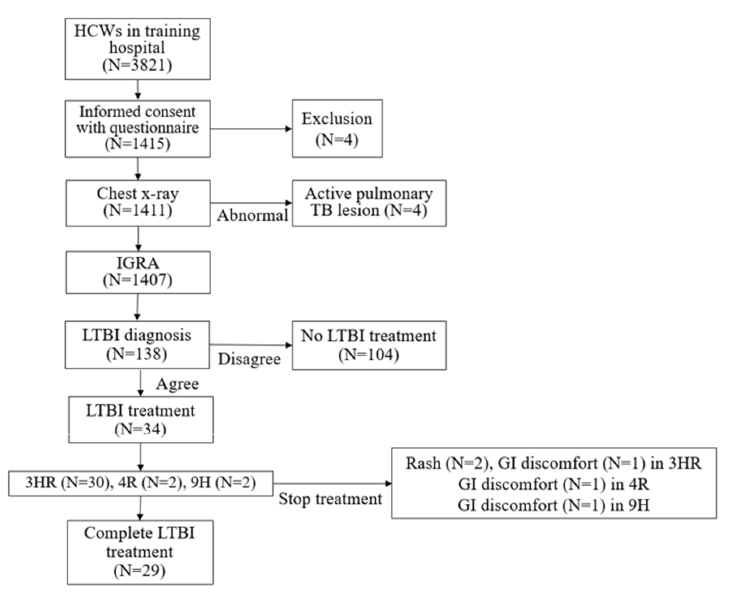
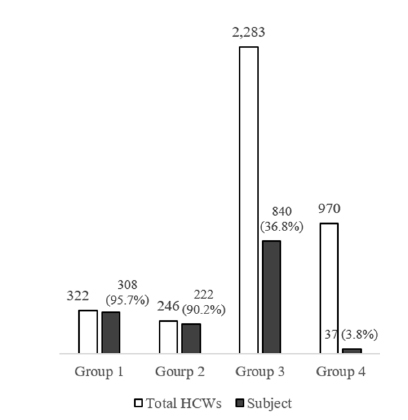
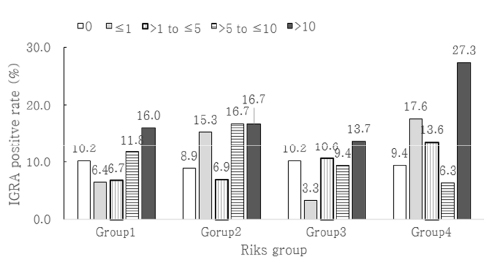
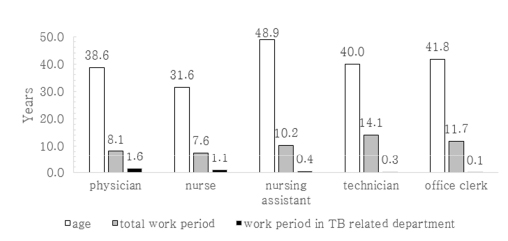
RESULTS
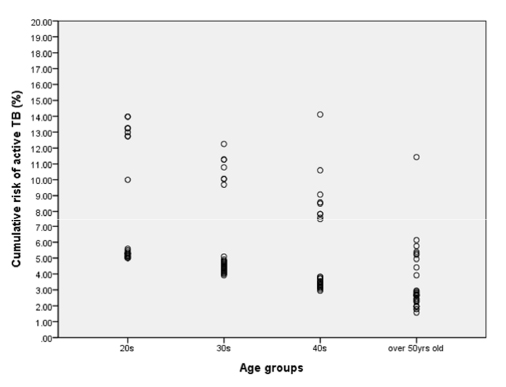
Of a total of 1,407 HCWs, a positive IGRA result was detected in 138 HCWs. The prevalence of LTBI in HCWs was found to be 9.8% [95% confidence interval (CI) 8.2-11.4]. It was observed that the prevalence of LTBI increased with age (P value < 0.001). However, it was also observed that duration of the working periods in a TB-related department was not associated with LTBI (P value=0.369). According to the multivariate analysis, an increased risk of LTBI was observed among participants aged ≥ 50 years [odds ratio (OR) 7.522, 95% CI 3.56-15.89] and nursing assistants (OR 2.912, 95% CI 1.283-6.608). The median cumulative risk of active TB with LTBI was estimated to be 4.31% [interquartile range (IQR) 3.43-5.29], and 4.41% (IQR 3.14-5.29) in HCWs with and without work experience in TB-related department, respectively. No significant difference was observed between two groups (P value=0.715).
CONCLUSION
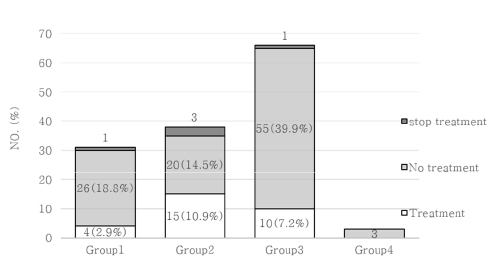
The prevalence of LTBI among HCWs may not be higher than that of individuals in other group facilities. It may be necessary to revise the treatment recommendations, which are classified based on the risk for LTBI associated with departments and locations of work.
MeSH Terms
Figure
Cited by 1 articles
-
TST (Tuberculin Skin Test)와 IGRA (Interferon-γ Release Assay)검사를 이용한 의료기관 종사자의 잠복결핵감염 유병률과 위험요인
Sin Jeong Kim, Eunjin Ha, Eun Suk Park, Jun Young Choi, Young Ae Kang
Korean J Healthc Assoc Infect Control Prev. 2020;25(1):46-53. doi: 10.14192/kjicp.2020.25.1.46.
Reference
-
1. WHO. Global tuberculosis report 2018. Geneva: World Health Organization;2018.2. Kim JH. Achievements in and challenges of tuberculosis control in South Korea. Emerg Infect Dis. 2015; 21:1913–1920.
Article3. Cho KS, Park WS, Jeong HR, Kim MJ, Park SJ, Park AY, et al. Prevalence of latent tuberculosis infection at congregated settings in the Republic of Korea, 2017. Division of TB & HIV Control, Center for Disease Prevention, KCDC;2017.4. Getahun H, Matteelli A, Abubakar I, Aziz MA, Baddeley A, Barreira D, et al. Management of latent Mycobacterium tuberculosis infection: WHO guidelines for low tuberculosis burden countries. Eur Respir J. 2015; 46:1563–1576.5. Jagger A, Reiter-Karam S, Hamada Y, Getahun H. National policies on the management of latent tuberculosis infection: review of 98 countries. Bull World Health Organ. 2018; 96:173–184F.
Article6. Park JS. The prevalence and risk factors of latent tuberculosis infection among health care workers working in a tertiary hospital in South Korea. Tuberc Respir Dis. 2018; 81:274–280.
Article7. Yeon JH, Seong H, Hur H, Park Y, Kim YA, Park YS, et al. Prevalence and risk factors of latent tuberculosis among Korean healthcare workers using whole-blood interferon-γ release assay. Sci Rep. 2018; 8:10113.
Article8. Yoon CG, Oh SY, Lee JB, Kim MH, Seo Y, Yang J, et al. Occupational risk of latent tuberculosis infection in health workers of 14 military hospitals. J Korean Med Sci. 2017; 32:1251–1257.
Article9. Lee KJ, Kang YA, Kim YM, Cho SN, Moon JW, Park MS, et al. Screening for latent tuberculosis infection in South Korean healthcare workers using a tuberculin skin test and whole blood interferon-gamma assay. Scand J Infect Dis. 2010; 42:672–678.10. Lee SH. Diagnosis and treatment of latent tuberculosis infection. Tuberc Respir Dis (Seoul). 2015; 78:56–63.
Article11. Menzies D, Gardiner G, Farhat M, Greenaway C, Pai M. Thinking in three dimensions: a web-based algorithm to aid the interpretation of tuberculin skin test results. Int J Tuberc Lung Dis. 2008; 12:498–505.12. Park SH, Lee SJ, Cho YJ, Jeong YY, Kim HC, Lee JD, et al. A prospective cohort study of latent tuberculosis in adult close contacts of active pulmonary tuberculosis patients in Korea. Korean J Intern Med. 2016; 31:517–524.
Article13. Njie GJ, Morris SB, Woodruff RY, Moro RN, Vernon AA, Borisov AS. Isoniazid-rifapentine for latent tuberculosis infection: a systematic review and meta-analysis. Am J Prev Med. 2018; 55:244–252.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Analysis of Prevalence and Risk Factors for Latent Tuberculosis Infection among Healthcare Workers
- Diagnosis and Treatment of Latent Tuberculosis Infection for Healthcare Workers
- Diagnosis and Treatment of Latent Tuberculosis Infection in Healthcare Workers
- The Prevalence and Risk Factors of Latent Tuberculosis Infection among Health Care Workers Working in a Tertiary Hospital in South Korea
- Prevalence and Risk Factors of Latent Tuberculosis Infection among Healthcare Workers Using Tuberculin Skin Test and Interferon-γ Release Assay at a Tertiary Hospital in South Korea