J Clin Neurol.
2019 Jan;15(1):84-89. 10.3988/jcn.2019.15.1.84.
Antiepileptic Drug Withdrawal after Surgery in Children with Focal Cortical Dysplasia: Seizure Recurrence and Its Predictors
- Affiliations
-
- 1Department of Pediatrics, Seoul National University Bundang Hospital, Seongnam, Korea.
- 2Department of Pediatrics, Pediatric Clinical Neuroscience Center, Seoul National University Children's Hospital, Seoul National University College of Medicine, Seoul, Korea. pednr@snu.ac.kr
- 3Department of Pediatrics, Seoul National University Boramae Medical Center, Seoul, Korea.
- 4Division of Pediatric Neurosurgery, Pediatric Clinical Neuroscience Center, Seoul National University Children's Hospital, Seoul National University College of Medicine, Seoul, Korea.
- 5Department of Anatomy and Cell Biology, Seoul National University College of Medicine, Seoul, Korea.
- KMID: 2451149
- DOI: http://doi.org/10.3988/jcn.2019.15.1.84
Abstract
- BACKGROUND AND PURPOSE
This study investigated the seizure recurrence rate and potential predictors of seizure recurrence following antiepileptic drug (AED) withdrawal after resective epilepsy surgery in children with focal cortical dysplasia (FCD).
METHODS
We retrospectively analyzed the records of 70 children and adolescents with FCD types I, II, and IIIa who underwent resective epilepsy surgery between 2004 and 2015 and were followed for at least 2 years after surgery.
RESULTS
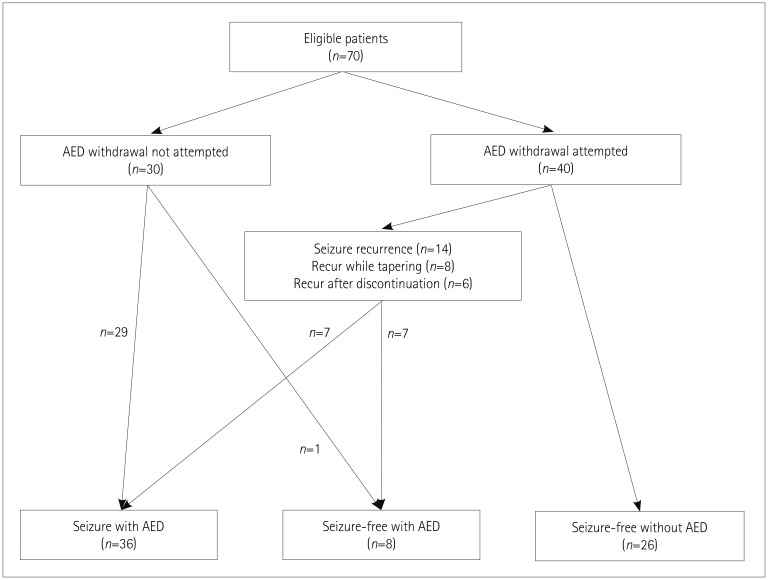
We attempted AED withdrawal in 40 patients. The median time of starting the AED reduction was 10.8 months after surgery. Of these 40 patients, 14 patients (35%) experienced seizure recurrence during AED reduction or after AED withdrawal. Half of the 14 patients who experienced recurrence regained seizure freedom after AED reintroduction and optimization. Compared with their preoperative status, the AED dose or number was decreased in 57.1% of patients, and remained unchanged in 14.3% after surgery. A multivariate analysis found that incomplete resection (p=0.004) and epileptic discharges on the postoperative EEG (p=0.025) were important predictors of seizure recurrence after AED withdrawal. Over the mean follow-up duration of 4.5 years after surgery, 34 patients (48.6% of the entire cohort) were seizure-free with and without AEDs.
CONCLUSIONS
Children with incomplete resection and epileptic discharges on postoperative EEG are at a high risk of seizure recurrence after drug withdrawal. Complete resection of FCD may lead to a favorable surgical outcome and successful AED withdrawal after surgery.
Keyword
MeSH Terms
Figure
Reference
-
1. Skirrow C, Cross JH, Cormack F, Harkness W, Vargha-Khadem F, Baldeweg T. Long-term intellectual outcome after temporal lobe surgery in childhood. Neurology. 2011; 76:1330–1337. PMID: 21482948.
Article2. van Schooneveld MM, van Erp N, Boshuisen K, Meekes J, Braun KP. Withdrawal of antiepileptic drugs improves psychomotor speed after childhood epilepsy surgery. Epilepsy Res. 2013; 107:200–203. PMID: 24050975.
Article3. Boshuisen K, van Schooneveld MM, Uiterwaal CS, Cross JH, Harrison S, Polster T, et al. Intelligence quotient improves after antiepileptic drug withdrawal following pediatric epilepsy surgery. Ann Neurol. 2015; 78:104–114. PMID: 25899932.
Article4. Helmstaedter C, Elger CE, Witt JA. The effect of quantitative and qualitative antiepileptic drug changes on cognitive recovery after epilepsy surgery. Seizure. 2016; 36:63–69. PMID: 26954934.
Article5. Lee SY, Lee JY, Kim DW, Lee SK, Chung CK. Factors related to successful antiepileptic drug withdrawal after anterior temporal lobectomy for medial temporal lobe epilepsy. Seizure. 2008; 17:11–18. PMID: 17604655.
Article6. Lachhwani DK, Loddenkemper T, Holland KD, Kotagal P, Mascha E, Bingaman W, et al. Discontinuation of medications after successful epilepsy surgery in children. Pediatr Neurol. 2008; 38:340–344. PMID: 18410850.
Article7. Park KI, Lee SK, Chu K, Jung KH, Bae EK, Kim JS, et al. Withdrawal of antiepileptic drugs after neocortical epilepsy surgery. Ann Neurol. 2010; 67:230–238. PMID: 20225284.
Article8. Menon R, Rathore C, Sarma SP, Radhakrishnan K. Feasibility of antiepileptic drug withdrawal following extratemporal resective epilepsy surgery. Neurology. 2012; 79:770–776. PMID: 22843256.
Article9. Berg AT, Vickrey BG, Langfitt JT, Sperling MR, Shinnar S, Bazil C, et al. Reduction of AEDs in postsurgical patients who attain remission. Epilepsia. 2006; 47:64–71.
Article10. Hoppe C, Poepel A, Sassen R, Elger CE. Discontinuation of anticonvulsant medication after epilepsy surgery in children. Epilepsia. 2006; 47:580–583. PMID: 16529625.
Article11. Boshuisen K, Braams O, Jennekens-Schinkel A, Braun KP, Jansen FE, van Rijen PC, et al. Medication policy after epilepsy surgery. Pediatr Neurol. 2009; 41:332–338. PMID: 19818934.
Article12. Boshuisen K, Arzimanoglou A, Cross JH, Uiterwaal CS, Polster T, van Nieuwenhuizen O, et al. Timing of antiepileptic drug withdrawal and long-term seizure outcome after paediatric epilepsy surgery (TimeToStop): a retrospective observational study. Lancet Neurol. 2012; 11:784–791. PMID: 22841352.
Article13. Rathore C, Panda S, Sarma PS, Radhakrishnan K. How safe is it to withdraw antiepileptic drugs following successful surgery for mesial temporal lobe epilepsy? Epilepsia. 2011; 52:627–635. PMID: 21219315.
Article14. Lamberink HJ, Otte WM, Geleijns K, Braun KP. Antiepileptic drug withdrawal in medically and surgically treated patients: a meta-analysis of seizure recurrence and systematic review of its predictors. Epileptic Disord. 2015; 17:211–228. PMID: 26292909.
Article15. Blümcke I, Thom M, Aronica E, Armstrong DD, Vinters HV, Palmini A, et al. The clinicopathologic spectrum of focal cortical dysplasias: a consensus classification proposed by an ad hoc Task Force of the ILAE Diagnostic Methods Commission. Epilepsia. 2011; 52:158–174. PMID: 21219302.16. Schmidt D, Baumgartner C, Löscher W. Seizure recurrence after planned discontinuation of antiepileptic drugs in seizure-free patients after epilepsy surgery: a review of current clinical experience. Epilepsia. 2004; 45:179–186. PMID: 14738426.
Article17. Schiller Y, Cascino GD, So EL, Marsh WR. Discontinuation of antiepileptic drugs after successful epilepsy surgery. Neurology. 2000; 54:346–349. PMID: 10668694.
Article18. Hader WJ, Mackay M, Otsubo H, Chitoku S, Weiss S, Becker L, et al. Cortical dysplastic lesions in children with intractable epilepsy: role of complete resection. J Neurosurg. 2004; 100(2 Suppl Pediatrics):110–117. PMID: 14758938.
Article19. Cossu M, Lo Russo G, Francione S, Mai R, Nobili L, Sartori I, et al. Epilepsy surgery in children: results and predictors of outcome on seizures. Epilepsia. 2008; 49:65–72. PMID: 17645538.
Article20. Krsek P, Maton B, Jayakar P, Dean P, Korman B, Rey G, et al. Incomplete resection of focal cortical dysplasia is the main predictor of poor postsurgical outcome. Neurology. 2009; 72:217–223. PMID: 19005171.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Discontinuing Antiepileptic Drugs after Pediatric Epilepsy Surgery for Focal Cortical Dysplasia
- Changes in frequency of seizure after acute antiepileptic drugs withdrawal
- The Surgical and Cognitive Outcomes of Focal Cortical Dysplasia
- Prognostic Factors for Recurrence of Seizure After Antiepileptic Drug Withdrawal
- Effects of Arbiturary Acute Anticonvulsnat Withdrawal in Epileptic Children