Percutaneous Radiofrequency Ablation with Multiple Electrodes for Medium-Sized Hepatocellular Carcinomas
- Affiliations
-
- 1Seoul National University Hospital, Seoul 110-744, Korea.
- 2Department of Radiology, and Institute of Radiation Medicine, Seoul National University College of Medicine, and Seoul National University Hospital, Seoul 110-744, Korea. jmsh@snu.ac.kr
- 3Department of Internal Medicine and Liver Research Institute, Seoul National University College of Medicine, Seoul 110-744, Korea.
- 4Department of Radiology, College of Medicine, Chungnam National University, Daejeon 320-721, Korea.
- KMID: 1058791
- DOI: http://doi.org/10.3348/kjr.2012.13.1.34
Abstract
OBJECTIVE
To prospectively evaluate the safety and short-term therapeutic efficacy of switching monopolar radiofrequency ablation (RFA) with multiple electrodes to treat medium-sized (3.1-5.0 cm), hepatocellular carcinomas (HCC).
MATERIALS AND METHODS
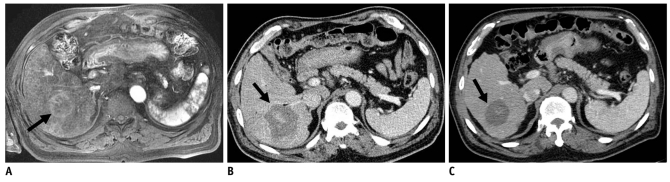
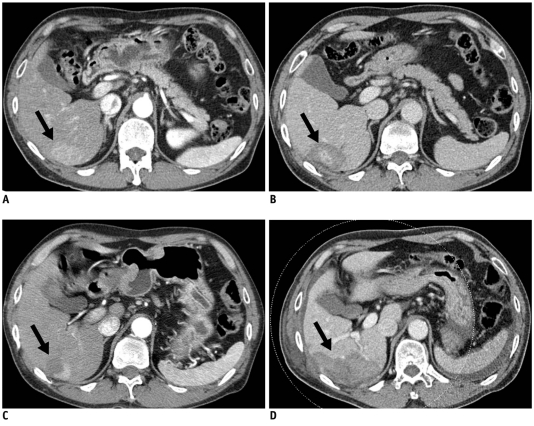
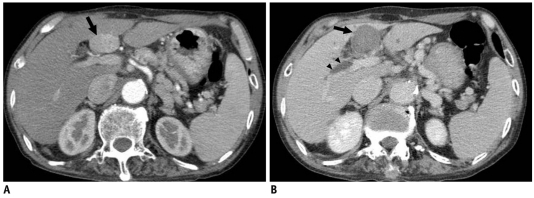
In this prospective study, 30 patients with single medium-sized HCCs (mean, 3.5 cm; range, 3.1-4.4 cm) were enrolled. The patients were treated under ultrasonographic guidance by percutaneous switching monopolar RFA with a multichannel RF generator and two or three internally cooled electrodes. Contrast-enhanced CT scans were obtained immediately after RFA, and the diameters and volume of the ablation zones were then measured. Follow-up CT scans were performed at the first month after ablation and every three months thereafter. Technical effectiveness, local progression and remote recurrence of HCCs were determined.
RESULTS
There were no major immediate or periprocedural complications. However, there was one bile duct stricture during the follow-up period. Technical effectiveness was achieved in 29 of 30 patients (97%). The total ablation time of the procedures was 25.4 +/- 8.9 minutes. The mean ablation volume was 73.8 +/- 56.4 cm3 and the minimum diameter was 4.1 +/- 7.3 cm. During the follow-up period (mean, 12.5 months), local tumor progression occurred in three of 29 patients (10%) with technical effectiveness, while new HCCs were detected in six of 29 patients (21%).
CONCLUSION
Switching monopolar RFA with multiple electrodes in order to achieve a sufficient ablation volume is safe and efficient. This method also showed relatively successful therapeutic effectiveness on short-term follow up for the treatment of medium-sized HCCs.
MeSH Terms
-
Adult
Aged
Carcinoma, Hepatocellular/radiography/*surgery
Catheter Ablation/instrumentation/*methods
Contrast Media/diagnostic use
Disease Progression
Electrodes
Female
Humans
Iohexol/analogs & derivatives/diagnostic use
Kaplan-Meier Estimate
Liver Neoplasms/radiography/*surgery
Male
Middle Aged
Neoplasm Recurrence, Local
Prospective Studies
Tomography, X-Ray Computed/*methods
Ultrasonography, Interventional
Figure
Cited by 4 articles
-
Recent Advances in the Image-Guided Tumor Ablation of Liver Malignancies: Radiofrequency Ablation with Multiple Electrodes, Real-Time Multimodality Fusion Imaging, and New Energy Sources
Dong Ho Lee, Jeong Min Lee
Korean J Radiol. 2018;19(4):545-559. doi: 10.3348/kjr.2018.19.4.545.Evaluation of the
In Vivo Efficiency and Safety of Hepatic Radiofrequency Ablation Using a 15-G Octopus® in Pig Liver
Eun Sun Lee, Jeong Min Lee, Kyung Won Kim, In Joon Lee, Joon Koo Han, Byung Ihn Choi
Korean J Radiol. 2013;14(2):194-201. doi: 10.3348/kjr.2013.14.2.194.Percutaneous Dual-Switching Monopolar Radiofrequency Ablation Using a Separable Clustered Electrode: A Preliminary Study
Tae Won Choi, Jeong Min Lee, Dong Ho Lee, Jeong-Hoon Lee, Su Jong Yu, Yoon Jun Kim, Jung-Hwan Yoon, Joon Koo Han
Korean J Radiol. 2017;18(5):799-808. doi: 10.3348/kjr.2017.18.5.799.No-Touch Radiofrequency Ablation of VX2 Hepatic Tumors
In Vivo in Rabbits: A Proof of Concept Study
Tae-Hyung Kim, Hyoung In Choi, Bo Ram Kim, Ji Hee Kang, Ju Gang Nam, Sae Jin Park, Seunghyun Lee, Jeong Hee Yoon, Dong Ho Lee, Ijin Joo, Jeong Min Lee
Korean J Radiol. 2018;19(6):1099-1109. doi: 10.3348/kjr.2018.19.6.1099.
Reference
-
1. Garrean S, Hering J, Saied A, Helton WS, Espat NJ. Radiofrequency ablation of primary and metastatic liver tumors: a critical review of the literature. Am J Surg. 2008; 195:508–520. PMID: 18361927.
Article2. Curley SA. Radiofrequency ablation of malignant liver tumors. Oncologist. 2001; 6:14–23. PMID: 11161225.
Article3. Lau WY, Lai EC. The current role of radiofrequency ablation in the management of hepatocellular carcinoma: a systematic review. Ann Surg. 2009; 249:20–25. PMID: 19106671.4. Chen MS, Li JQ, Liang HH, Lin XJ, Guo RP, Zheng Y, et al. [Comparison of effects of percutaneous radiofrequency ablation and surgical resection on small hepatocellular carcinoma]. Zhonghua Yi Xue Za Zhi. 2005; 85:80–83. PMID: 15774210.5. Hong SN, Lee SY, Choi MS, Lee JH, Koh KC, Paik SW, et al. Comparing the outcomes of radiofrequency ablation and surgery in patients with a single small hepatocellular carcinoma and well-preserved hepatic function. J Clin Gastroenterol. 2005; 39:247–252. PMID: 15718869.
Article6. Lu MD, Kuang M, Liang LJ, Xie XY, Peng BG, Liu GJ, et al. [Surgical resection versus percutaneous thermal ablation for early-stage hepatocellular carcinoma: a randomized clinical trial]. Zhonghua Yi Xue Za Zhi. 2006; 86:801–805. PMID: 16681964.7. Lupo L, Panzera P, Giannelli G, Memeo M, Gentile A, Memeo V. Single hepatocellular carcinoma ranging from 3 to 5 cm: radiofrequency ablation or resection? HPB (Oxford). 2007; 9:429–434. PMID: 18345289.8. Montorsi M, Santambrogio R, Bianchi P, Donadon M, Moroni E, Spinelli A, et al. Survival and recurrences after hepatic resection or radiofrequency for hepatocellular carcinoma in cirrhotic patients: a multivariate analysis. J Gastrointest Surg. 2005; 9:62–67. discussion 67-68. PMID: 15623446.
Article9. Kosari K, Gomes M, Hunter D, Hess DJ, Greeno E, Sielaff TD. Local, intrahepatic, and systemic recurrence patterns after radiofrequency ablation of hepatic malignancies. J Gastrointest Surg. 2002; 6:255–263. PMID: 11992812.
Article10. Kuvshinoff BW, Ota DM. Radiofrequency ablation of liver tumors: influence of technique and tumor size. Surgery. 2002; 132:605–611. discussion 611-602. PMID: 12407343.
Article11. Livraghi T, Goldberg SN, Lazzaroni S, Meloni F, Ierace T, Solbiati L, et al. Hepatocellular carcinoma: radio-frequency ablation of medium and large lesions. Radiology. 2000; 214:761–768. PMID: 10715043.
Article12. Bowles BJ, Machi J, Limm WM, Severino R, Oishi AJ, Furumoto NL, et al. Safety and efficacy of radiofrequency thermal ablation in advanced liver tumors. Arch Surg. 2001; 136:864–869. PMID: 11485520.
Article13. Ni Y, Mulier S, Miao Y, Michel L, Marchal G. A review of the general aspects of radiofrequency ablation. Abdom Imaging. 2005; 30:381–400. PMID: 15776302.
Article14. Buscarini E, Savoia A, Brambilla G, Menozzi F, Reduzzi L, Strobel D, et al. Radiofrequency thermal ablation of liver tumors. Eur Radiol. 2005; 15:884–894. PMID: 15754165.
Article15. Lorentzen T. A cooled needle electrode for radiofrequency tissue ablation: thermodynamic aspects of improved performance compared with conventional needle design. Acad Radiol. 1996; 3:556–563. PMID: 8796717.
Article16. Goldberg SN, Solbiati L, Hahn PF, Cosman E, Conrad JE, Fogle R, et al. Large-volume tissue ablation with radio frequency by using a clustered, internally cooled electrode technique: laboratory and clinical experience in liver metastases. Radiology. 1998; 209:371–379. PMID: 9807561.
Article17. Kim SW, Rhim H, Park M, Kim H, Kim YS, Choi D, et al. Percutaneous radiofrequency ablation of hepatocellular carcinomas adjacent to the gallbladder with internally cooled electrodes: assessment of safety and therapeutic efficacy. Korean J Radiol. 2009; 10:366–376. PMID: 19568465.
Article18. Goldberg SN, Gazelle GS, Solbiati L, Rittman WJ, Mueller PR. Radiofrequency tissue ablation: increased lesion diameter with a perfusion electrode. Acad Radiol. 1996; 3:636–644. PMID: 8796727.19. Buscarini L, Rossi S. Technology for Radiofrequency Thermal Ablation of Liver Tumors. Semin Laparosc Surg. 1997; 4:96–101. PMID: 10401146.
Article20. Rossi S, Buscarini E, Garbagnati F, Di Stasi M, Quaretti P, Rago M, et al. Percutaneous treatment of small hepatic tumors by an expandable RF needle electrode. AJR Am J Roentgenol. 1998; 170:1015–1022. PMID: 9530052.
Article21. Chen MH, Yang W, Yan K, Zou MW, Solbiati L, Liu JB, et al. Large liver tumors: protocol for radiofrequency ablation and its clinical application in 110 patients--mathematic model, overlapping mode, and electrode placement process. Radiology. 2004; 232:260–271. PMID: 15166323.
Article22. de Baere T, Rehim MA, Teriitheau C, Deschamps F, Lapeyre M, Dromain C, et al. Usefulness of guiding needles for radiofrequency ablative treatment of liver tumors. Cardiovasc Intervent Radiol. 2006; 29:650–654. PMID: 16729235.
Article23. Dodd GD 3rd, Frank MS, Aribandi M, Chopra S, Chintapalli KN. Radiofrequency thermal ablation: computer analysis of the size of the thermal injury created by overlapping ablations. AJR Am J Roentgenol. 2001; 177:777–782. PMID: 11566672.24. Dupuy DE, Goldberg SN. Image-guided radiofrequency tumor ablation: challenges and opportunities--part II. J Vasc Interv Radiol. 2001; 12:1135–1148. PMID: 11585879.
Article25. Curley SA, Izzo F, Ellis LM, Nicolas Vauthey J, Vallone P. Radiofrequency ablation of hepatocellular cancer in 110 patients with cirrhosis. Ann Surg. 2000; 232:381–391. PMID: 10973388.
Article26. Goldberg SN, Solbiati L, Halpern EF, Gazelle GS. Variables affecting proper system grounding for radiofrequency ablation in an animal model. J Vasc Interv Radiol. 2000; 11:1069–1075. PMID: 10997473.
Article27. Haemmerich D, Lee FT Jr, Schutt DJ, Sampson LA, Webster JG, Fine JP, et al. Large-volume radiofrequency ablation of ex vivo bovine liver with multiple cooled cluster electrodes. Radiology. 2005; 234:563–568. PMID: 15601891.
Article28. Lee FT Jr, Haemmerich D, Wright AS, Mahvi DM, Sampson LA, Webster JG. Multiple probe radiofrequency ablation: pilot study in an animal model. J Vasc Interv Radiol. 2003; 14:1437–1442. PMID: 14605110.
Article29. Lee JM, Rhim H, Han JK, Youn BJ, Kim SH, Choi BI. Dual-probe radiofrequency ablation: an in vitro experimental study in bovine liver. Invest Radiol. 2004; 39:89–96. PMID: 14734923.30. Laeseke PF, Sampson LA, Haemmerich D, Brace CL, Fine JP, Frey TM, et al. Multiple-electrode radiofrequency ablation creates confluent areas of necrosis: in vivo porcine liver results. Radiology. 2006; 241:116–124. PMID: 16928978.
Article31. Clasen S, Schmidt D, Boss A, Dietz K, Krober SM, Claussen CD, et al. Multipolar radiofrequency ablation with internally cooled electrodes: experimental study in ex vivo bovine liver with mathematic modeling. Radiology. 2006; 238:881–890. PMID: 16424244.
Article32. Lee JM, Han JK, Lee JY, Kim SH, Choi JY, Lee MW, et al. Hepatic radiofrequency ablation using multiple probes: ex vivo and in vivo comparative studies of monopolar versus multipolar modes. Korean J Radiol. 2006; 7:106–117. PMID: 16799271.
Article33. Haemmerich D, Lee FT Jr. Multiple applicator approaches for radiofrequency and microwave ablation. Int J Hyperthermia. 2005; 21:93–106. PMID: 15764353.
Article34. Haemmerich D, Tungjitkusolmun S, Staelin ST, Lee FT Jr, Mahvi DM, Webster JG. Finite-element analysis of hepatic multiple probe radio-frequency ablation. IEEE Trans Biomed Eng. 2002; 49:836–842. PMID: 12148822.
Article35. Laeseke PF, Sampson LA, Frey TM, Mukherjee R, Winter TC 3rd, Lee FT Jr, et al. Multiple-electrode radiofrequency ablation: comparison with a conventional cluster electrode in an in vivo porcine kidney model. J Vasc Interv Radiol. 2007; 18:1005–1010. PMID: 17675619.
Article36. Lee JM, Han JK, Kim HC, Choi YH, Kim SH, Choi JY, et al. Switching monopolar radiofrequency ablation technique using multiple, internally cooled electrodes and a multichannel generator: ex vivo and in vivo pilot study. Invest Radiol. 2007; 42:163–171. PMID: 17287646.37. Laeseke PF, Frey TM, Brace CL, Sampson LA, Winter TC 3rd, Ketzler JR, et al. Multiple-electrode radiofrequency ablation of hepatic malignancies: initial clinical experience. AJR Am J Roentgenol. 2007; 188:1485–1494. PMID: 17515366.
Article38. Weisbrod AJ, Atwell TD, Callstrom MR, Farrell MA, Mandrekar JN, Charboneau JW. Percutaneous radiofrequency ablation with a multiple-electrode switching-generator system. J Vasc Interv Radiol. 2007; 18:1528–1532. PMID: 18057287.
Article39. Bruix J, Sherman M. Management of hepatocellular carcinoma. Hepatology. 2005; 42:1208–1236. PMID: 16250051.
Article40. Nakazawa T, Kokubu S, Shibuya A, Ono K, Watanabe M, Hidaka H, et al. Radiofrequency ablation of hepatocellular carcinoma: correlation between local tumor progression after ablation and ablative margin. AJR Am J Roentgenol. 2007; 188:480–488. PMID: 17242258.
Article41. Goldberg SN, Grassi CJ, Cardella JF, Charboneau JW, Dodd GD 3rd, Dupuy DE, et al. Image-guided tumor ablation: standardization of terminology and reporting criteria. Radiology. 2005; 235:728–739. PMID: 15845798.
Article42. Lee JM, Han JK, Kim HC, Kim SH, Kim KW, Joo SM, et al. Multiple-electrode radiofrequency ablation of in vivo porcine liver: comparative studies of consecutive monopolar, switching monopolar versus multipolar modes. Invest Radiol. 2007; 42:676–683. PMID: 17984764.43. Cabassa P, Donato F, Simeone F, Grazioli L, Romanini L. Radiofrequency ablation of hepatocellular carcinoma: long-term experience with expandable needle electrodes. AJR Am J Roentgenol. 2006; 186:S316–S321. PMID: 16632694.
Article44. Khan MR, Poon RT, Ng KK, Chan AC, Yuen J, Tung H, et al. Comparison of percutaneous and surgical approaches for radiofrequency ablation of small and medium hepatocellular carcinoma. Arch Surg. 2007; 142:1136–1143. discussion 1143. PMID: 18086979.
Article45. Shibata T, Iimuro Y, Yamamoto Y, Maetani Y, Ametani F, Itoh K, et al. Small hepatocellular carcinoma: comparison of radio-frequency ablation and percutaneous microwave coagulation therapy. Radiology. 2002; 223:331–337. PMID: 11997534.
Article46. Bilchik AJ, Wood TF, Allegra D, Tsioulias GJ, Chung M, Rose DM, et al. Cryosurgical ablation and radiofrequency ablation for unresectable hepatic malignant neoplasms: a proposed algorithm. Arch Surg. 2000; 135:657–662. discussion 662-654. PMID: 10843361.47. Brace CL, Sampson LA, Hinshaw JL, Sandhu N, Lee FT Jr. Radiofrequency ablation: simultaneous application of multiple electrodes via switching creates larger, more confluent ablations than sequential application in a large animal model. J Vasc Interv Radiol. 2009; 20:118–124. PMID: 19019701.
Article48. Lencioni R, Cioni D, Crocetti L, Franchini C, Pina CD, Lera J, et al. Early-stage hepatocellular carcinoma in patients with cirrhosis: long-term results of percutaneous image-guided radiofrequency ablation. Radiology. 2005; 234:961–967. PMID: 15665226.
Article49. Shibata T, Maetani Y, Isoda H, Hiraoka M. Radiofrequency ablation for small hepatocellular carcinoma: prospective comparison of internally cooled electrode and expandable electrode. Radiology. 2006; 238:346–353. PMID: 16373776.
Article50. Choi D, Lim HK, Rhim H, Kim YS, Lee WJ, Paik SW, et al. Percutaneous radiofrequency ablation for early-stage hepatocellular carcinoma as a first-line treatment: long-term results and prognostic factors in a large single-institution series. Eur Radiol. 2007; 17:684–692. PMID: 17093964.
Article51. Buscarini E, Buscarini L. Radiofrequency thermal ablation with expandable needle of focal liver malignancies: complication report. Eur Radiol. 2004; 14:31–37. PMID: 14564470.
Article52. Livraghi T, Solbiati L, Meloni MF, Gazelle GS, Halpern EF, Goldberg SN. Treatment of focal liver tumors with percutaneous radio-frequency ablation: complications encountered in a multicenter study. Radiology. 2003; 226:441–451. PMID: 12563138.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Recent Advances in the Image-Guided Tumor Ablation of Liver Malignancies: Radiofrequency Ablation with Multiple Electrodes, Real-Time Multimodality Fusion Imaging, and New Energy Sources
- Current status and future of radiofrequency ablation for hepatocellular carcinoma
- Recent technical advances in radiofrequency ablations for hepatocellular carcinoma
- Radiofrequency Thermal Ablation of Hepatocellular Carcinomas
- Completely Ablated Hepatocellular Carcinoma by Percutaneous Radiofrequency Thermal Ablation