J Gastric Cancer.
2011 Dec;11(4):219-224.
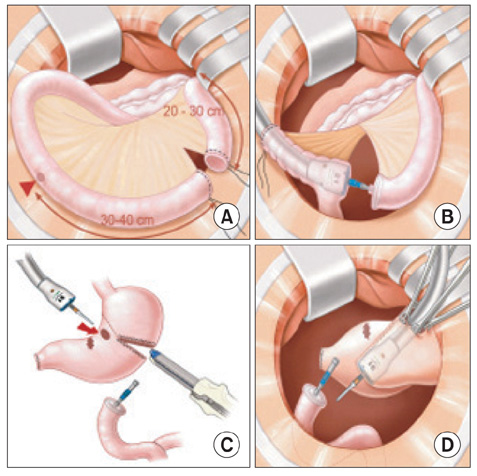
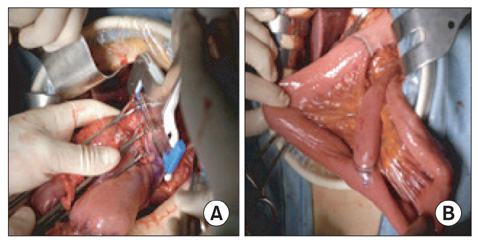
Efficacy of Roux-en-Y Reconstruction Using Two Circular Staplers after Subtotal Gastrectomy: Results from a Pilot Study Comparing with Billroth-I Reconstruction
- Affiliations
-
- 1Department of Surgery, Ajou University School of Medicine, Suwon, Korea. hhcmc75@naver.com
Abstract
- PURPOSE
The Roux en Y method has rarely been performed due to longer operation time and high risk of complication, despite several merits including prevention of bile reflux. We conducted a retrospective review of the result of Roux en Y reconstruction using two circular staplers after subtotal gastrectomy.
MATERIALS AND METHODS
From December 2008 to May 2009, a total of 26 patients underwent Roux en Y reconstruction using two circular staplers after subtotal gastrectomy, and seventy-two patients underwent Billroth-I reconstruction. Roux en Y anastomosis was performed using two circular staplers without hand sewing anastomosis. We compared clinicopathologic features and surgical outcomes between the two groups. All patients underwent gastrofiberscopy between six and twelve months after surgery to compare the bile reflux.
RESULTS
No significant differences in clinicopathologic findings were observed between the two groups, except for the rate of minimal invasive surgery (P=0.004) and cancer stage (P=0.002). No differences in the rate of morbidity (P=0.353) and admission duration (P=0.391) were observed between the two groups. Gastrofiberscopic findings showed a significant reduction of bile reflux in the remnant stomach in the Roux en Y group (P=0.019).
CONCLUSIONS
When compared with Billroth-I reconstruction, Roux en Y reconstruction using the double stapler technique was found to reduce bile reflux in the remnant stomach without increasing postoperative morbidity. Based on these results, we planned to begin a randomized controlled clinical trial for comparison of Roux en Y reconstruction using this method with Billroth-I anastomosis.
MeSH Terms
Figure
Reference
-
1. Kim JP. Current status of surgical treatment of gastric cancer. J Surg Oncol. 2002. 79:79–80.
Article2. Roukos DH. Current advances and changes in treatment strategy may improve survival and quality of life in patients with potentially curable gastric cancer. Ann Surg Oncol. 1999. 6:46–56.
Article3. Fukuhara K, Osugi H, Takada N, Takemura M, Higashino M, Kinoshita H. Reconstructive procedure after distal gastrectomy for gastric cancer that best prevents duodenogastroesophageal reflux. World J Surg. 2002. 26:1452–1457.
Article4. Lehnert T, Buhl K. Techniques of reconstruction after total gastrectomy for cancer. Br J Surg. 2004. 91:528–539.
Article5. Yang HK, Lee HJ, Ahn HS, Yoo MW, Lee IK, Lee KU. Safety of modified double-stapling end-to-end gastroduodenostomy in distal subtotal gastrectomy. J Surg Oncol. 2007. 96:624–629.
Article6. Kojima K, Yamada H, Inokuchi M, Kawano T, Sugihara K. A comparison of Roux-en-Y and Billroth-I reconstruction after laparoscopy-assisted distal gastrectomy. Ann Surg. 2008. 247:962–967.
Article7. Shinoto K, Ochiai T, Suzuki T, Okazumi S, Ozaki M. Effectiveness of Roux-en-Y reconstruction after distal gastrectomy based on an assessment of biliary kinetics. Surg Today. 2003. 33:169–177.
Article8. Lorusso D, Linsalata M, Pezzolla F, Berloco P, Osella AR, Guerra V, et al. Duodenogastric reflux and gastric mucosal polyamines in the non-operated stomach and in the gastric remnant after Billroth II gastric resection. A role in gastric carcinogenesis? Anticancer Res. 2000. 20:2197–2201.9. Miwa K, Hasegawa H, Fujimura T, Matsumoto H, Miyata R, Kosaka T, et al. Duodenal reflux through the pylorus induces gastric adenocarcinoma in the rat. Carcinogenesis. 1992. 13:2313–2316.
Article10. Svensson JO. Duodenogastric reflux after gastric surgery. Scand J Gastroenterol. 1983. 18:729–734.
Article11. Kubo M, Sasako M, Gotoda T, Ono H, Fujishiro M, Saito D, et al. Endoscopic evaluation of the remnant stomach after gastrectomy: proposal for a new classification. Gastric Cancer. 2002. 5:83–89.
Article12. Berman S, Hashizume M, Yang Y, DuPree J, Matsumoto T. Intraoperative hemostasis and wound healing in intestinal anastomoses using the ILA stapling device. Am J Surg. 1988. 155:520–525.
Article13. Shoji Y, Nihei Z, Hirayama R, Mishima Y. Experiences with the linear cutter technique for performing Roux-en-Y anastomosis following total gastrectomy. Surg Today. 1995. 25:27–31.
Article14. Yo LS, Consten EC, Quarles van Ufford HM, Gooszen HG, Gagner M. Buttressing of the staple line in gastrointestinal anastomoses: overview of new technology designed to reduce perioperative complications. Dig Surg. 2006. 23:283–291.
Article15. Britton JP, Johnston D, Ward DC, Axon AT, Barker MC. Gastric emptying and clinical outcome after Roux-en-Y diversion. Br J Surg. 1987. 74:900–904.
Article16. Herrington JL Jr, Scott HW Jr, Sawyers JL. Experience with vagotomy--antrectomy and Roux-en-Y gastrojejunostomy in surgical treatment of duodenal, gastric, and stomal ulcers. Ann Surg. 1984. 199:590–597.
Article17. Hocking MP, Vogel SB, Falasca CA, Woodward ER. Delayed gastric emptying of liquids and solids following Roux-en-Y biliary diversion. Ann Surg. 1981. 194:494–501.
Article18. Gustavsson S, Ilstrup DM, Morrison P, Kelly KA. Roux-Y stasis syndrome after gastrectomy. Am J Surg. 1988. 155:490–494.
Article19. Fujiwara M, Kodera Y, Kasai Y, Kanyama Y, Hibi K, Ito K, et al. Laparoscopy-assisted distal gastrectomy with systemic lymph node dissection for early gastric carcinoma: a review of 43 cases. J Am Coll Surg. 2003. 196:75–81.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- A Novel Roux-en-Y Reconstruction Involving the Use of Two Circular Staplers after Distal Subtotal Gastrectomy for Gastric Cancer
- Totally Laparoscopic Roux-en-Y Gastrojejunostomy after Laparoscopic Distal Gastrectomy: Analysis of Initial 50 Consecutive Cases of Single Surgeon in Comparison with Totally Laparoscopic Billroth I Reconstruction
- A Clinical Study of the Uncut Roux-en-Y Gastrojejunostomy Using a Short Roux Limb after Subtotal Gastrectomy
- Laparoscopic Hiatal Hernia Repair and Roux-en-Y Conversion for Refractory Duodenogastroesophageal Reflux after Billroth I Distal Gastrectomy
- Various types of reconstruction after pancreaticoduodenectomy for the patients who underwent all types of gastrectomy: a single-center experience