Korean J Phys Anthropol.
2016 Dec;29(4):145-154. 10.11637/kjpa.2016.29.4.145.
Morphometric Analysis of Distances between Sacral Hiatus and Conus Medullaris Using Magnetic Resonance Image in Korean Adult
- Affiliations
-
- 1Department of Anatomy, College of Medicine, Pusan National University, Korea. sikyoon@pusan.ac.kr
- 2Busan Wooridul Spine Hospital, Korea.
- KMID: 2364637
- DOI: http://doi.org/10.11637/kjpa.2016.29.4.145
Abstract
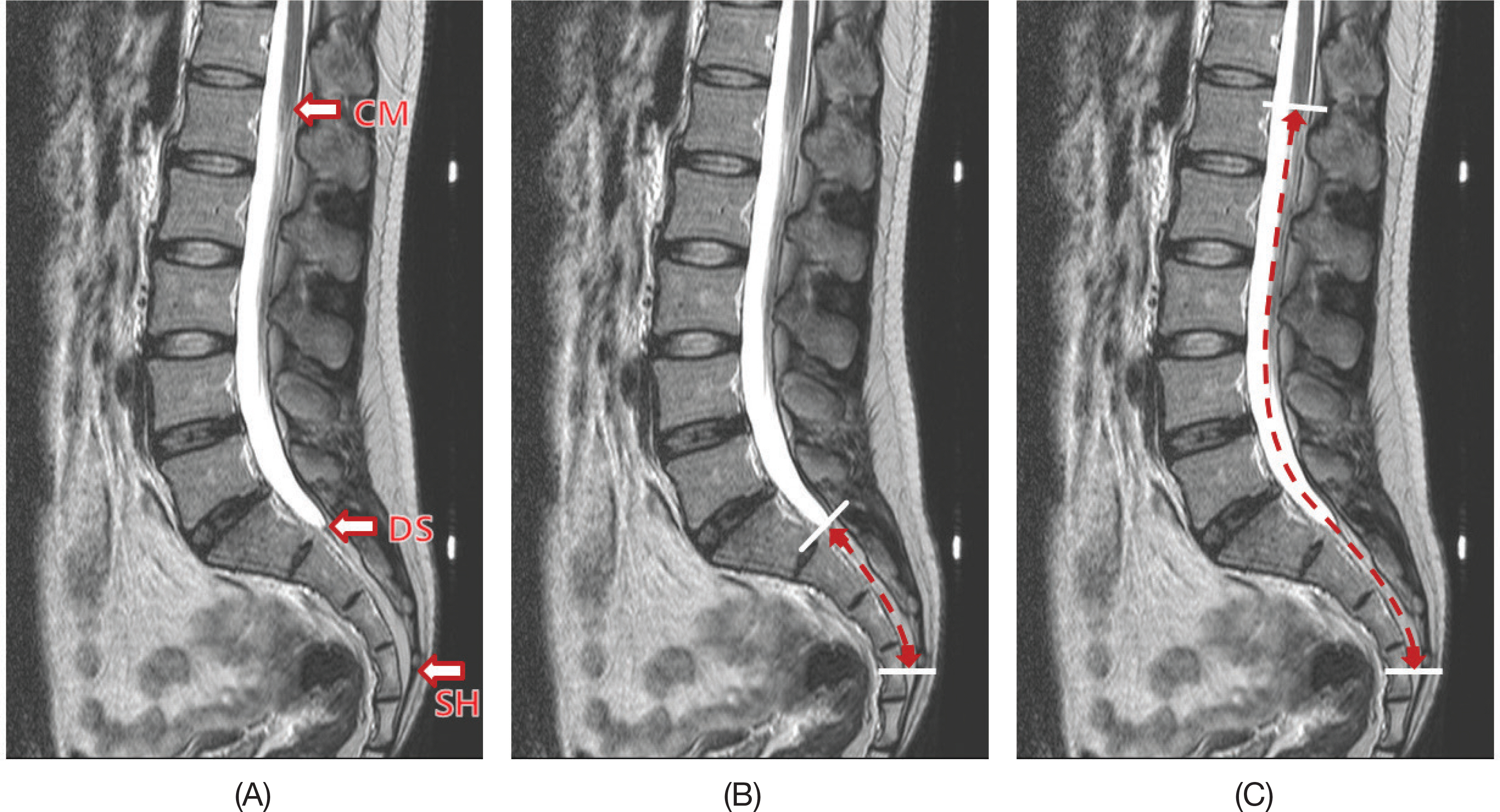
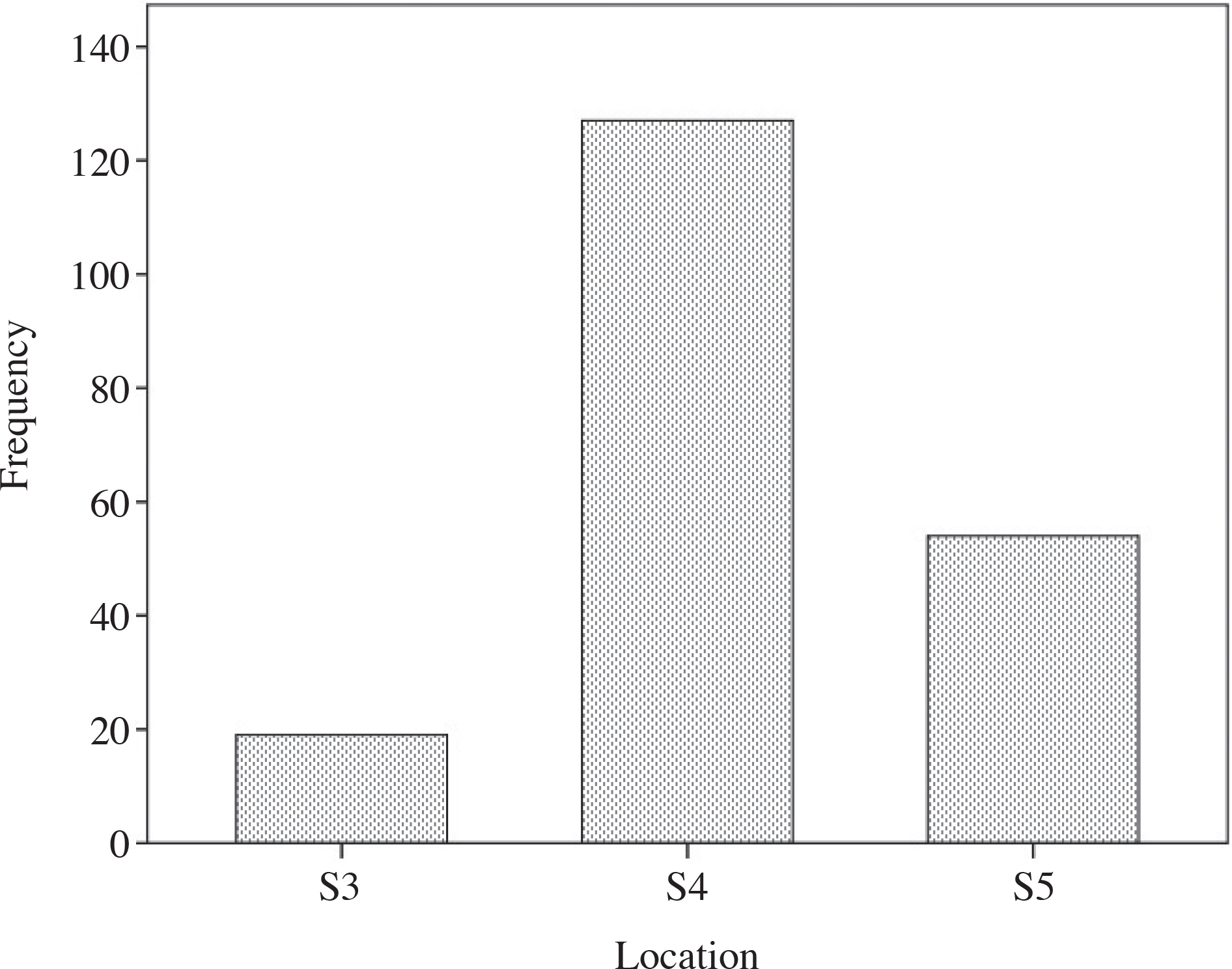
- The purpose of this study was to provide basic biometric data on Korean adults through magnetic resonance imaging (MRI)-based measurements of the distances between the apex of sacral hiatus (SH) and the termination of dural sac (DS), and between SH and conus medullaris (CM) because they are critical to the performance of epidural neuroplasty. A total of 200 patients (88 males and 112 females) with back pain, who had no spine fracture, significant spinal deformity, and spondyloisthesis were selected for this study. The subjects were of mean age 54.3 (20~84) years and mean height 161.3 cm (135~187). T2-weighted MRI images were used for correlation analysis to evaluate the relationships between the distances, and variables such as sex and height. In all patients, the mean distance between SH and DS was 62.8±9.4 mm and the mean distance between SH and CM was 232.2±21.8 mm. The minimum distance and the maximum distance between SH and DS were 34.8 mm and 93.9 mm respectively, and the minimum distance and the maximum distance between SH and CM were 155.0 mm and 284.0 mm respectively. In female patients, both the distances between the SH and DS, and between SH and CM were shorter when compared to those of the male patients (p<0.05). Both the distances between SH and DS and between SH and CM showed a significant correlation with height (p<0.01). The results of this study will provide a useful biometric data on the distances between SH and DS and between SH and CM in Korean in ensuring clinical safety and in the development of more effective catheterization techniques for epidural neuroplasty in Korean.
Keyword
MeSH Terms
Figure
Reference
-
References
1. Racz G, Heavner J, Trescot A. Percutaneous lysis of epidural adhesions: evidence for safety and efficacy. Pain Pract. 2008; 8:277–86.2. Hsu E, Atanelov L, Plunkett A, Chai N, Chen Y, Cohen S. Epidural lysis of adhesions for failed back surgery and spinal stenosis: factors associated with treatment outcome. Anesth Analg. 2014; 118:215–24.3. Erdine S, Talu GK. Precautions during epidural neuroplasty. Pain Pract. 2002; 2:308–14.
Article4. Ho KY, Manghnani P. Acute monoplegia after lysis of epidural adhesions: A case Report. Pain Pract. 2008; 8:404–7.
Article5. Bogduk N. The sacrum. Clinical anatomy of the lumbar spine and sacrum. 4th ed.Philadelphia: Elsevier Churchill Livingstone;2005. p. 59–61.6. Senoglu N, Senoglu M, Oksuz H, Gumusalan Y, Yuksel KZ, Zencirci B, et al. Landmarks of the sacral hiatus for caudal epidural block: an anatomical study. Br J Anaesth. 2005; 95:692–5.
Article7. Sekiguchi M, Yabuki S, Satoh K, Kikuchi S. An anatomic study of the sacral hiatus: a basis for successful caudal epidural block. Clin J Pain. 2004; 20:51–4.
Article8. Demiryürek D, Aydingöz Ü, Akşit M, Yener N, Geyik P. MR imaging determination of the normal level of conus medullaris. Clin Imaging. 2002; 26:375–7.
Article9. Louis R. Topographic relationship of the vertebral column, spinal-cord, and nerve roots. Anat Clin. 1978; 1:3–12.10. Kwon SW, Kim TS, Kim HS, Rhyu IJ. The Tip Level of the Conus Medullaris by Magnetic Resonance Imaging and Cadaver Studies in Korean Adults. Korean J Phys Anthropol. 2016; 29:47–51.
Article11. Macdonald A, Chatrath P, Spector T, Ellis H. Level of termination of the spinal cord and the dural sac: a magnetic resonance study. Clin Anat. 1999; 12:149–52.
Article12. Becker SH, Arenson RL. Cost benefits of picture archiving and communication system. J Am Med Assoc. 1994; 1:361–71.13. Deyo RA, Loeser JD, Bigos SJ. Herniated lumbar intervertebral disk. Ann Intern Med. 1990; 112:598–603.
Article14. Shin SW. Low back pain: Review of anatomy and pathophysiology. J Korean Med Assoc. 2006; 49:656–64.
Article15. Suk SI. Lumbar disc disease. Spinal surgery. Revised edition. Seoul: Newest Medical Journal;2004. p. 218–20.16. Modic MT, Pavlicek W, Weinstein MA, Boumphrey F, Ngo F, Hardy R, et al. Magnetic rresonance imaging of intervertebral disk disease: Clinical and pulse sequence considerations. Radiology. 1984; 152:103–11.17. Barson AJ. The vertebral level of termination of spinal cord during normal and abnormal development. J Anat. 1970; 106:489–97.18. Kim DC. Anatomical studies on the vertebral column and spinal cord of korean subjects: Part Ⅱ. Study on the adult. Seoul J Med. 1961; 2:149–63.19. Joo SP, Kim SH, Lee JK, Kim TS, Jung S, Kang SS, et al. The variation of position of the conus medullaris in korean adults: A magnetic resonance imaging study. J Korean Neurosurg Soc. 2001; 30:451–5.20. Park SJ, Choi WS, Kim EJ, Oh JH, Yoon Y. Normal variation of lumbosacral thecal sac on MR. J Korean Radiol Soc. 1996; 34:565–69.
Article21. Ko HY, Kim K, Kim HJ. Normal variations of the spinal cord termination. J Korean Acad Rehabil Med. 1998; 22:1040–43.22. Ko HY, Park JH, Kim HJ, Kim K. Variations of end level of the dural sac. J Korean Acad Rehabil Med. 1999; 23:805–8.23. Nasr AY. Vertebral level and measurements of conus medullaris and dural sac termination with special reference to the apex of the sacral hiatus: anatomical and MRI radiologic study. Folia Morphol. 2016; 75:287–99. doi:. DOI: 10.5603/FM.a2016.0004.24. Mustafa MS, Mahmoud OM, El Raouf HH, Atef HM. Morphometric study of sacral hiatus in adult human Egyptian sacra: Their significance in caudal epidural anesthesia. Saudi J Anaesth. 2012; 6:350–7.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- The Tip Level of the Conus Medullaris by Magnetic Resonance Imaging and Cadaver Studies in Korean Adults
- Multiple Hemangioendotheliomas of the Spinal Cord and Cauda Equina: Case Report
- Magnetic Resonance Imaging Observations of the Conus Medullaris in a Korean Population
- Intramedullary Spinal Cystic Teratoma of the Conus Mudullaris with Caudal Exophytic Growth: Case Report
- Conus Medullaris Hemangioblastoma