J Korean Surg Soc.
2013 Jun;84(6):338-345. 10.4174/jkss.2013.84.6.338.
Optimal timing of surgery after neoadjuvant chemoradiation therapy in locally advanced rectal cancer
- Affiliations
-
- 1Department of Surgery, Yonsei University College of Medicine, Seoul, Korea. namkyuk@yuhs.ac
- 2Department of Surgery, Hansol Hospital, Seoul, Korea.
- KMID: 1505183
- DOI: http://doi.org/10.4174/jkss.2013.84.6.338
Abstract
- PURPOSE
The optimal time between neoadjuvant chemoradiotherapy (CRT) and surgery for rectal cancer has been debated. This study evaluated the influence of this interval on oncological outcomes.
METHODS
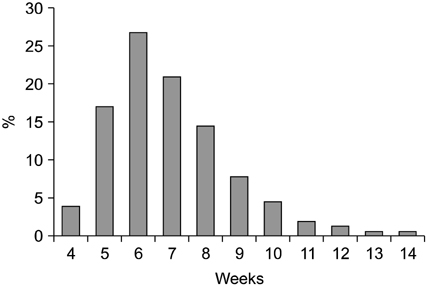
We compared postoperative complications, pathological downstaging, disease recurrence, and survival in patients with locally advanced rectal cancer who underwent surgical resection <8 weeks (group A, n = 105) to those who had surgery > or =8 weeks (group B, n = 48) after neoadjuvant CRT.
RESULTS
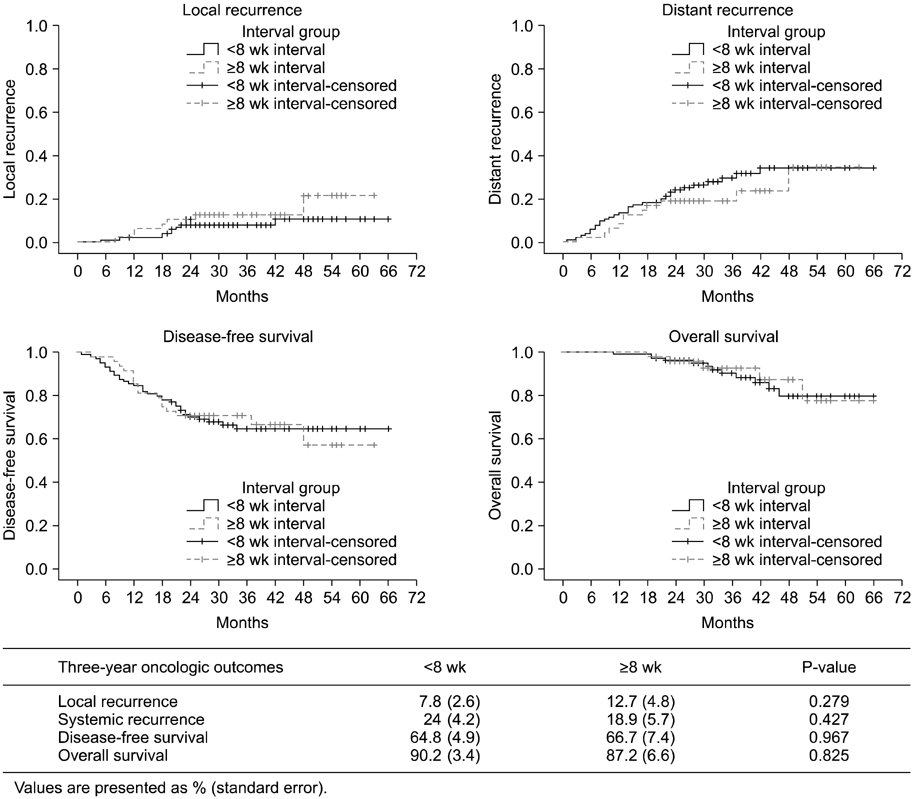
Of 153 patients, 117 (76.5%) were male and 36 (23.5%) were female. Mean age was 57.8 years (range, 28 to 79 years). There was no difference in the rate of sphincter preserving surgery between the two groups (group A, 82.7% vs. group B, 77.6%; P = 0.509). The longer interval group had decreased postoperative complications, although statistical significance was not reached (group A, 28.8% vs. group B, 14.3%; P = 0.068). A total of 111 (group A, 75 [71.4%] and group B, 36 [75%]) patients were downstaged and 26 (group A, 17 [16.2%] and group B, 9 [18%]) achieved pathological complete response (pCR). There was no significant difference in the pCR rate (P = 0.817). The longer interval group experienced significant improvement in the nodal (N) downstaging rate (group A, 46.7% vs. group B, 66.7%; P = 0.024). The local recurrence (P = 0.279), distant recurrence (P = 0.427), disease-free survival (P = 0.967), and overall survival (P = 0.825) rates were not significantly different.
CONCLUSION
It is worth delaying surgical resection for 8 weeks or more after completion of CRT as it is safe and is associated with higher nodal downstaging rates.
MeSH Terms
Figure
Reference
-
1. de Campos-Lobato LF, Geisler DP, da Luz Moreira A, Stocchi L, Dietz D, Kalady MF. Neoadjuvant therapy for rectal cancer: the impact of longer interval between chemoradiation and surgery. J Gastrointest Surg. 2011. 15:444–450.2. Lim SB, Choi HS, Jeong SY, Kim DY, Jung KH, Hong YS, et al. Optimal surgery time after preoperative chemoradiotherapy for locally advanced rectal cancers. Ann Surg. 2008. 248:243–251.3. Pahlman L. Optimal timing of surgery after preoperative chemoradiotherapy for rectal cancer. Nat Clin Pract Oncol. 2009. 6:128–129.4. Habr-Gama A, Perez RO, Proscurshim I, Nunes Dos Santos RM, Kiss D, Gama-Rodrigues J, et al. Interval between surgery and neoadjuvant chemoradiation therapy for distal rectal cancer: does delayed surgery have an impact on outcome? Int J Radiat Oncol Biol Phys. 2008. 71:1181–1188.5. Colorectal Cancer Collaborative Group. Adjuvant radiotherapy for rectal cancer: a systematic overview of 8,507 patients from 22 randomised trials. Lancet. 2001. 358:1291–1304.6. Swedish Rectal Cancer Trial. Improved survival with preoperative radiotherapy in resectable rectal cancer. N Engl J Med. 1997. 336:980–987.7. van Gijn W, Marijnen CA, Nagtegaal ID, Kranenbarg EM, Putter H, Wiggers T, et al. Preoperative radiotherapy combined with total mesorectal excision for resectable rectal cancer: 12-year follow-up of the multicentre, randomised controlled TME trial. Lancet Oncol. 2011. 12:575–582.8. Sebag-Montefiore D, Stephens RJ, Steele R, Monson J, Grieve R, Khanna S, et al. Preoperative radiotherapy versus selective postoperative chemoradiotherapy in patients with rectal cancer (MRC CR07 and NCIC-CTG C016): a multicentre, randomised trial. Lancet. 2009. 373:811–820.9. Sauer R, Becker H, Hohenberger W, Rodel C, Wittekind C, Fietkau R, et al. Preoperative versus postoperative chemoradiotherapy for rectal cancer. N Engl J Med. 2004. 351:1731–1740.10. Folkesson J, Birgisson H, Pahlman L, Cedermark B, Glimelius B, Gunnarsson U. Swedish Rectal Cancer Trial: long lasting benefits from radiotherapy on survival and local recurrence rate. J Clin Oncol. 2005. 23:5644–5650.11. Francois Y, Nemoz CJ, Baulieux J, Vignal J, Grandjean JP, Partensky C, et al. Influence of the interval between preoperative radiation therapy and surgery on downstaging and on the rate of sphincter-sparing surgery for rectal cancer: the Lyon R90-01 randomized trial. J Clin Oncol. 1999. 17:2396.12. Tran CL, Udani S, Holt A, Arnell T, Kumar R, Stamos MJ. Evaluation of safety of increased time interval between chemoradiation and resection for rectal cancer. Am J Surg. 2006. 192:873–877.13. Garcia-Aguilar J, Smith DD, Avila K, Bergsland EK, Chu P, Krieg RM, et al. Optimal timing of surgery after chemoradiation for advanced rectal cancer: preliminary results of a multicenter, nonrandomized phase II prospective trial. Ann Surg. 2011. 254:97–102.14. Heald RJ. A new approach to rectal cancer. Br J Hosp Med. 1979. 22:277–281.15. Tulchinsky H, Shmueli E, Figer A, Klausner JM, Rabau M. An interval >7 weeks between neoadjuvant therapy and surgery improves pathologic complete response and disease-free survival in patients with locally advanced rectal cancer. Ann Surg Oncol. 2008. 15:2661–2667.16. Stein DE, Mahmoud NN, Anne PR, Rose DG, Isenberg GA, Goldstein SD, et al. Longer time interval between completion of neoadjuvant chemoradiation and surgical resection does not improve downstaging of rectal carcinoma. Dis Colon Rectum. 2003. 46:448–453.17. Das P, Skibber JM, Rodriguez-Bigas MA, Feig BW, Chang GJ, Hoff PM, et al. Clinical and pathologic predictors of locoregional recurrence, distant metastasis, and overall survival in patients treated with chemoradiation and mesorectal excision for rectal cancer. Am J Clin Oncol. 2006. 29:219–224.18. Marijnen CA, Kapiteijn E, van de Velde CJ, Martijn H, Steup WH, Wiggers T, et al. Acute side effects and complications after short-term preoperative radiotherapy combined with total mesorectal excision in primary rectal cancer: report of a multicenter randomized trial. J Clin Oncol. 2002. 20:817–825.19. Wong RK, Tandan V, De Silva S, Figueredo A. Pre-operative radiotherapy and curative surgery for the management of localized rectal carcinoma. Cochrane Database Syst Rev. 2007. (2):CD002102.20. Veenhof AA, Kropman RH, Engel AF, Craanen ME, Meijer S, Meijer OW, et al. Preoperative radiation therapy for locally advanced rectal cancer: a comparison between two different time intervals to surgery. Int J Colorectal Dis. 2007. 22:507–513.21. Marijnen CA, van de Velde CJ, Putter H, van den Brink M, Maas CP, Martijn H, et al. Impact of short-term preoperative radiotherapy on health-related quality of life and sexual functioning in primary rectal cancer: report of a multicenter randomized trial. J Clin Oncol. 2005. 23:1847–1858.22. Hartley A, Giridharan S, Gray L, Billingham L, Ismail T, Geh JI. Retrospective study of acute toxicity following short-course preoperative radiotherapy. Br J Surg. 2002. 89:889–895.23. Moore HG, Gittleman AE, Minsky BD, Wong D, Paty PB, Weiser M, et al. Rate of pathologic complete response with increased interval between preoperative combined modality therapy and rectal cancer resection. Dis Colon Rectum. 2004. 47:279–286.24. Withers HR, Haustermans K. Where next with preoperative radiation therapy for rectal cancer? Int J Radiat Oncol Biol Phys. 2004. 58:597–602.25. Kerr SF, Norton S, Glynne-Jones R. Delaying surgery after neoadjuvant chemoradiotherapy for rectal cancer may reduce postoperative morbidity without compromising prognosis. Br J Surg. 2008. 95:1534–1540.26. Guillem JG, Chessin DB, Cohen AM, Shia J, Mazumdar M, Enker W, et al. Long-term oncologic outcome following preoperative combined modality therapy and total mesorectal excision of locally advanced rectal cancer. Ann Surg. 2005. 241:829–836.27. Onaitis MW, Noone RB, Hartwig M, Hurwitz H, Morse M, Jowell P, et al. Neoadjuvant chemoradiation for rectal cancer: analysis of clinical outcomes from a 13-year institutional experience. Ann Surg. 2001. 233:778–785.28. Shivnani AT, Small W Jr, Stryker SJ, Kiel KD, Lim S, Halverson AL, et al. Pre-operative chemoradiation for rectal cancer: results of multimodality management and analysis of prognostic factors. Am J Surg. 2007. 193:389–393.29. Kim NK, Baik SH, Seong JS, Kim H, Roh JK, Lee KY, et al. Oncologic outcomes after neoadjuvant chemoradiation followed by curative resection with tumor-specific mesorectal excision for fixed locally advanced rectal cancer: Impact of postirradiated pathologic downstaging on local recurrence and survival. Ann Surg. 2006. 244:1024–1030.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Current approaches in intensification of long-course chemoradiotherapy in locally advanced rectal cancer: a review
- Unveiling the profound advantages of total neoadjuvant therapy in rectal cancer: a trailblazing exploration
- Recent Advances in the Diagnosis and Treatment for Rectal Cancer
- The Outcome of Preoperative Chemoradiation to Locally Advanced Rectal Cancer
- How to Achieve a Higher Pathologic Complete Response in Patients With Locally Advanced Rectal Cancer Who Receive Preoperative Chemoradiation Therapy