Restor Dent Endod.
2024 Aug;49(3):e31. 10.5395/rde.2024.49.e31.
Assessment of mechanical allodynia in healthy teeth adjacent and contralateral to endodontically diseased teeth: a clinical study
- Affiliations
-
- 1Department of Conservative Dentistry and Endodontics, Bharati Vidyapeeth Dental College, Navi Mumbai, Maharashtra, India
- 2Department of Periodontics and Implantology, Bharati Vidyapeeth Dental College, Navi Mumbai, Maharashtra, India
- KMID: 2559744
- DOI: http://doi.org/10.5395/rde.2024.49.e31
Abstract
Objectives
The present study investigated the prevalence of mechanical allodynia (MA) in healthy teeth adjacent and contralateral to endodontically diseased teeth.
Materials and Methods
This cross-sectional study included 114 patients with symptomatic irreversible pulpitis and apical periodontitis in permanent mandibular first molars who possessed healthy teeth adjacent and contralateral to the endodontically diseased tooth. The mechanical sensitivity of the teeth was determined by percussion testing. The presence or absence of pain on percussion in the teeth adjacent and contralateral to the endodontically diseased tooth and the tooth distal to the contralateral symmetrical tooth was recorded according to coding criteria. The prevalence of MA was computed as a percentage, and binary logistic regression analysis was done. The Fisher exact test and Mann-Whitney U test were used for binary and ordinal data.
Results
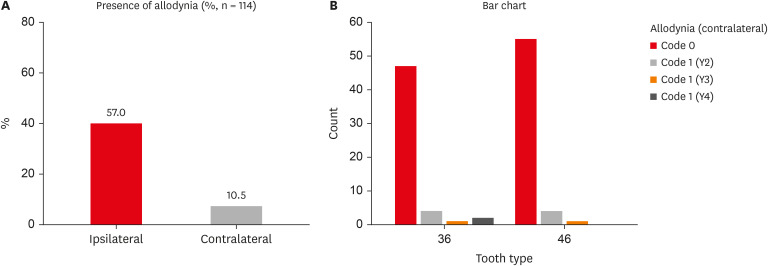
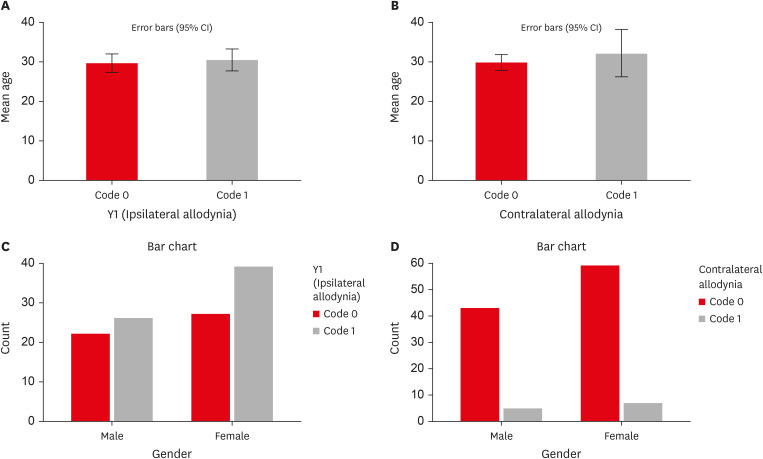
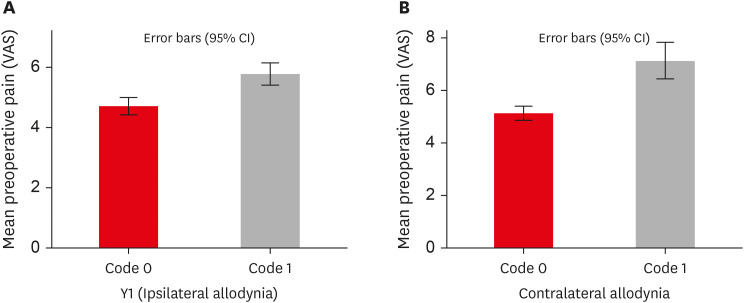
Age and sex did not influence the prevalence of MA. An increased prevalence of MA was found in patients with higher levels of spontaneous pain (p < 0.001). The prevalence of allodynia was 57% in teeth adjacent to endodontically diseased teeth and 10.5% in teeth contralateral to endodontically diseased teeth. In addition, on the ipsilateral side, there were more painful sensations distal to the diseased tooth than mesially.
Conclusions
Despite being disease-free, teeth adjacent and contralateral to endodontically diseased teeth exhibited pain on percussion. There was a direct association between the severity of the patient’s pain and the presence of MA.
Keyword
Figure
Reference
-
1. Kayaoglu G, Ekici M, Altunkaynak B. Mechanical allodynia in healthy teeth adjacent and contrala-teral to endodontically diseased teeth: a clinical study. J Endod. 2020; 46:611–618. PMID: 32145907.2. Jang YE, Kim Y, Kim BS. Influence of preoperative mechanical allodynia on predicting postoperative pain after root canal treatment: a prospective clinical study. J Endod. 2021; 47:770–778.e1. PMID: 33516824.3. Gutmann JL, Baumgartner JC, Gluskin AH, Hartwell GR, Walton RE. Identify and define all diagnostic terms for periapical/periradicular health and disease states. J Endod. 2009; 35:1658–1674. PMID: 19932340.4. Owatz CB, Khan AA, Schindler WG, Schwartz SA, Keiser K, Hargreaves KM. The incidence of mechanical allodynia in patients with irreversible pulpitis. J Endod. 2007; 33:552–556. PMID: 17437870.5. Khan AA, McCreary B, Owatz CB, Schindler WG, Schwartz SA, Keiser K, et al. The development of a diagnostic instrument for the measurement of mechanical allodynia. J Endod. 2007; 33:663–666. PMID: 17509402.6. Khan AA, Owatz CB, Schindler WG, Schwartz SA, Keiser K, Hargreaves KM. Measurement of mechanical allodynia and local anesthetic efficacy in patients with irreversible pulpitis and acute periradicular periodontitis. J Endod. 2007; 33:796–799. PMID: 17804314.7. Woolf CJ. Central sensitization: implications for the diagnosis and treatment of pain. Pain. 2011; 152(Supplement):S2–SS15. PMID: 20961685.8. Latremoliere A, Woolf CJ. Central sensitization: a generator of pain hypersensitivity by central neural plasticity. J Pain. 2009; 10:895–926. PMID: 19712899.9. Sessle BJ. Acute and chronic craniofacial pain: brainstem mechanisms of nociceptive transmission and neuroplasticity, and their clinical correlates. Crit Rev Oral Biol Med. 2000; 11:57–91. PMID: 10682901.10. Chiang CY, Park SJ, Kwan CL, Hu JW, Sessle BJ. NMDA receptor mechanisms contribute to neuroplasticity induced in caudalis nociceptive neurons by tooth pulp stimulation. J Neurophysiol. 1998; 80:2621–2631. PMID: 9819268.11. Worsley MA, Allen CE, Billinton A, King AE, Boissonade FM. Chronic tooth pulp inflammation induces persistent expression of phosphorylated ERK (pERK) and phosphorylated p38 (pp38) in trigeminal subnucleus caudalis. Neuroscience. 2014; 269:318–330. PMID: 24709040.12. Alelyani AA, Azar PS, Khan AA, Chrepa V, Diogenes A. Quantitative assessment of mechanical allodynia and central sensitization in endodontic patients. J Endod. 2020; 46:1841–1848. PMID: 32941893.13. Hashemipour MA, Borna R. Incidence and characteristics of acute referred orofacial pain caused by a posterior single tooth pulpitis in an Iranian population. Pain Pract. 2014; 14:151–157. PMID: 23425258.14. Cuschieri S. The STROBE guidelines. Saudi J Anaesth. 2019; 13(Supplement 1):S31–S34. PMID: 30930717.15. Orstavik D, Kerekes K, Eriksen HM. The periapical index: a scoring system for radiographic assessment of apical periodontitis. Endod Dent Traumatol. 1986; 2:20–34. PMID: 3457698.16. Zanini M, Decerle N, Hennequin M, Cousson PY. Revisiting Orstavik’s PAI score to produce a reliable and reproducible assessment of the outcomes of endodontic treatments in routine practice. Eur J Dent Educ. 2021; 25:291–298. PMID: 32966674.17. Matsuura S, Shimizu K, Shinoda M, Ohara K, Ogiso B, Honda K, et al. Mechanisms underlying ectopic persistent tooth-pulp pain following pulpal inflammation. PLoS One. 2013; 8:e52840. PMID: 23341909.18. Lee C, Ramsey A, De Brito-Gariepy H, Michot B, Podborits E, Melnyk J, et al. Molecular, cellular and behavioral changes associated with pathological pain signaling occur after dental pulp injury. Mol Pain. 2017; 13:1744806917715173. PMID: 28580829.19. Torebjörk HE, Lundberg LE, LaMotte RH. Central changes in processing of mechanoreceptive input in capsaicin-induced secondary hyperalgesia in humans. J Physiol. 1992; 448:765–780. PMID: 1593489.20. Shenker NG, Haigh RC, Mapp PI, Harris N, Blake DR. Contralateral hyperalgesia and allodynia following intradermal capsaicin injection in man. Rheumatology (Oxford). 2008; 47:1417–1421. PMID: 18632788.21. Simonic-Kocijan S, Zhao X, Liu W, Wu Y, Uhac I, Wang K. TRPV1 channel-mediated bilateral allodynia induced by unilateral masseter muscle inflammation in rats. Mol Pain. 2013; 9:68. PMID: 24377488.22. Tariba Knežević P, Vukman R, Antonić R, Kovač Z, Uhač I, Simonić-Kocijan S. The role of P2X3 receptors in bilateral masseter muscle allodynia in rats. Croat Med J. 2016; 57:530–539. PMID: 28051277.23. Koltzenburg M, Wall PD, McMahon SB. Does the right side know what the left is doing? Trends Neurosci. 1999; 22:122–127. PMID: 10199637.24. Schreiber KL, Beitz AJ, Wilcox GL. Activation of spinal microglia in a murine model of peripheral inflammation-induced, long-lasting contralateral allodynia. Neurosci Lett. 2008; 440:63–67. PMID: 18541374.25. Sandkühler J. Models and mechanisms of hyperalgesia and allodynia. Physiol Rev. 2009; 89:707–758. PMID: 19342617.26. Serra CM, Manns AE. Bite force measurements with hard and soft bite surfaces. J Oral Rehabil. 2013; 40:563–568. PMID: 23692029.27. Ferrario VF, Sforza C, Serrao G, Dellavia C, Tartaglia GM. Single tooth bite forces in healthy young adults. J Oral Rehabil. 2004; 31:18–22. PMID: 15125591.28. Unruh AM. Gender variations in clinical pain experience. Pain. 1996; 65:123–167. PMID: 8826503.29. Fillingim RB, Maixner W. Gender differences in the responses to noxious stimuli. Pain Forum. 1995; 4:209–221.30. Nagendrababu V, Gutmann JL. Factors associated with postobturation pain following single-visit nonsurgical root canal treatment: a systematic review. Quintessence Int. 2017; 48:193–208. PMID: 27669726.31. Machado R, Comparin D, Ignácio SA, da Silva Neto UX. Postoperative pain after endodontic treatment of necrotic teeth with large intentional foraminal enlargement. Restor Dent Endod. 2021; 46:e31. PMID: 34513637.32. Kishnani S, Saha SG, Bhardwaj A, Dubey S, Saha M, Kala S, et al. Unmasking the effect of analgesics on endodontic diagnosis using a novel bite force sensor device: a prospective, randomized clinical trial. J Clin Diagn Res. 2016; 10:ZC38–ZC42.33. Eliav E, Gracely RH. Sensory changes in the territory of the lingual and inferior alveolar nerves following lower third molar extraction. Pain. 1998; 77:191–199. PMID: 9766837.34. Matsuda M, Huh Y, Ji RR. Roles of inflammation, neurogenic inflammation, and neuroinflammation in pain. J Anesth. 2019; 33:131–139. PMID: 30448975.35. Erdogan O, Malek M, Gibbs JL. Associations between pain severity, clinical findings, and endodontic disease: a cross-sectional study. J Endod. 2021; 47:1376–1382. PMID: 34256059.36. Read JK, McClanahan SB, Khan AA, Lunos S, Bowles WR. Effect of ibuprofen on masking endodontic diagnosis. J Endod. 2014; 40:1058–1062. PMID: 25069908.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- THE PROGNOSIS OF THE TEETH IN THE MANDIBULAR FRACTURE LINES
- Characteristics of a deep crack occurred on intact molars without restoration
- Fibre reinforcement in a structurally compromised endodontically treated molar: a case report
- Expression of osteoclastogenesis related factors in dental implant patients
- Evaluation of canine teeth crown reduction technique in macaques