J Korean Med Sci.
2022 Dec;37(50):e358. 10.3346/jkms.2022.37.e358.
Improving the Prognosis of Patients With Acute Ischemic Stroke Treated in the Late Time Window After the Introduction of Advanced Imaging Software: Benefits From Thrombectomy in the Extended Time Window
- Affiliations
-
- 1Department of Neurology, National Health Insurance Service Ilsan Hospital, Goyang, Korea
- 2Department of Neurology, Yonsei University College of Medicine, Seoul, Korea
- 3Department of Radiology, National Health Insurance Service Ilsan Hospital, Goyang, Korea
- 4Department of Neurology, Graduate School of Medicine, Kangwon National University, Chuncheon, Korea
- KMID: 2537056
- DOI: http://doi.org/10.3346/jkms.2022.37.e358
Abstract
- Background
Mechanical thrombectomy (MT) of ischemic stroke was recommended as a clinical guideline in 2015, and the indication for time was expanded in 2018 based on two clinical studies. We aimed to compare and analyze the prognosis of patients treated under the extended time indication before and after the introduction of advanced software.
Methods
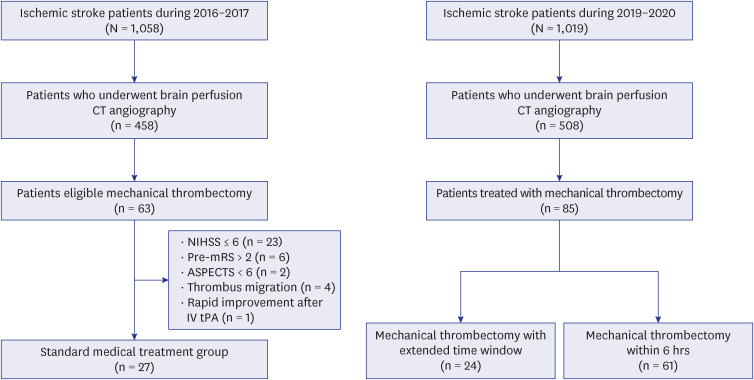
We obtained data from medical records between 2016 to 2020. From 2016 to 2017, patients who did not receive MT who visited the hospital within 24 hours from the last normal time (LNT) were classified as standard medical treatment (SMT) group. Among patients who underwent MT between 2019 and 2020, patients who visited the hospital between 6-24 hours from the LNT were classified into the extended MT (EMT) group. Good outcome was defined as 3-months modified rankin scale (mRS) ≤ 2, and a poor outcome as mRS ≥ 4.
Results
From 2016 to 2017, 1,058 patients were hospitalized for ischemic stroke, of which 60 (5.7%) received MT, and 27 patients were classified into the SMT group. Among 1,019 patients between 2019 and 2020, 85 (8.3%) received MT, and 24 patients were in the EMT group. Among the SMT group, only 3 had a good prognosis, and 24 (88.9%) had a poor prognosis. However, in the EMT group, 10 (41.7%) had a good prognosis, and 9 (37.5%) had a poor prognosis. The SMT group had a 49.1 times higher risk of poor prognosis compared to the EMT group (P = 0.008).
Conclusion
The number of patients with ischemic stroke who receive MT has increased by using advanced imaging software. It was confirmed that patients treated based on the extended time indication also had a good prognosis.
Figure
Reference
-
1. Ko SB, Park HK, Kim BM, Heo JH, Rha JH, Kwon SU, et al. 2019 update of the Korean clinical practice guidelines of stroke for endovascular recanalization therapy in patients with acute ischemic stroke. J Stroke. 2019; 21(2):231–240. PMID: 30991800.2. National Institute of Neurological Disorders and Stroke rt-PA Stroke Study Group. Tissue plasminogen activator for acute ischemic stroke. N Engl J Med. 1995; 333(24):1581–1587. PMID: 7477192.3. Powers WJ, Derdeyn CP, Biller J, Coffey CS, Hoh BL, Jauch EC, et al. 2015 American Heart Association/American Stroke Association focused update of the 2013 guidelines for the early management of patients with acute ischemic stroke regarding endovascular treatment: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2015; 46(10):3020–3035. PMID: 26123479.4. Jeong HS. An update of recent guideline for the endovascular recanalization therapy in acute ischemic stroke. J Korean Neurol Assoc. 2018; 36(3):145–151.5. Albers GW, Marks MP, Kemp S, Christensen S, Tsai JP, Ortega-Gutierrez S, et al. Thrombectomy for stroke at 6 to 16 hours with selection by perfusion imaging. N Engl J Med. 2018; 378(8):708–718. PMID: 29364767.6. Nogueira RG, Jadhav AP, Haussen DC, Bonafe A, Budzik RF, Bhuva P, et al. Thrombectomy 6 to 24 hours after stroke with a mismatch between deficit and infarct. N Engl J Med. 2018; 378(1):11–21. PMID: 29129157.7. Powers WJ, Rabinstein AA, Ackerson T, Adeoye OM, Bambakidis NC, Becker K, et al. 2018 Guidelines for the early management of patients with acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2018; 49(3):e46–110. PMID: 29367334.8. Seo KD, Suh SH. Endovascular treatment in acute ischemic stroke: a nationwide survey in Korea. Neurointervention. 2018; 13(2):84–89. PMID: 30196678.9. Powers WJ, Rabinstein AA, Ackerson T, Adeoye OM, Bambakidis NC, Becker K, et al. Guidelines for the early management of patients with acute ischemic stroke: 2019 update to the 2018 guidelines for the early management of acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2019; 50(12):e344–e418. PMID: 31662037.10. Rangaraju S, Haussen D, Nogueira RG, Nahab F, Frankel M. Comparison of 3-month stroke disability and quality of life across modified rankin scale categories. Interv Neurol. 2017; 6(1-2):36–41. PMID: 28611832.11. Beckhauser MT, Castro-Afonso LH, Dias FA, Nakiri GS, Monsignore LM, Martins Filho RK, et al. Extended time window mechanical thrombectomy for acute stroke in Brazil. J Stroke Cerebrovasc Dis. 2020; 29(10):105134. PMID: 32912530.12. Virtanen P, Tomppo L, Martinez-Majander N, Kokkonen T, Sillanpää M, Lappalainen K, et al. Thrombectomy in acute ischemic stroke in the extended time window: real-life experience in a high-volume center. J Stroke Cerebrovasc Dis. 2022; 31(8):106603. PMID: 35749938.13. Hui W, Wu C, Zhao W, Sun H, Hao J, Liang H, et al. Efficacy and safety of recanalization therapy for acute ischemic stroke with large vessel occlusion: a systematic review. Stroke. 2020; 51(7):2026–2035. PMID: 32486966.14. Gunda B, Sipos I, Stang R, Böjti P, Dobronyi L, Takács T, et al. Comparing extended versus standard time window for thrombectomy: caseload, patient characteristics, treatment rates and outcomes-a prospective single-centre study. Neuroradiology. 2021; 63(4):603–607. PMID: 32935174.15. Kim JY, Kang K, Kang J, Koo J, Kim DH, Kim BJ, et al. Executive summary of stroke statistics in Korea 2018: a report from the Epidemiology Research Council of the Korean Stroke Society. J Stroke. 2019; 21(1):42–59. PMID: 30558400.16. MacKenzie IE, Moeini-Naghani I, Sigounas D. Trends in endovascular mechanical thrombectomy in treatment of acute ischemic stroke in the United States. World Neurosurg. 2020; 138:e839–e846. PMID: 32229302.17. Rinaldo L, Rabinstein AA, Cloft H, Knudsen JM, Castilla LR, Brinjikji W. Racial and ethnic disparities in the utilization of thrombectomy for acute stroke. Stroke. 2019; 50(9):2428–2432. PMID: 31366313.18. Richter D, Weber R, Eyding J, Bartig D, Misselwitz B, Grau A, et al. Acute ischemic stroke care in Germany - further progress from 2016 to 2019. Neurol Res Pract. 2021; 3(1):14. PMID: 33789773.19. Chia NH, Leyden JM, Newbury J, Jannes J, Kleinig TJ. Determining the number of ischemic strokes potentially eligible for endovascular thrombectomy: a population-based study. Stroke. 2016; 47(5):1377–1380. PMID: 26987869.20. Jadhav AP, Desai SM, Kenmuir CL, Rocha M, Starr MT, Molyneaux BJ, et al. Eligibility for endovascular trial enrollment in the 6- to 24-hour time window: analysis of a single comprehensive stroke center. Stroke. 2018; 49(4):1015–1017. PMID: 29581344.21. Health Insurance Review and Assessment Service (HIRA). Healthcare Bigdata Hub. Updated 2022. Accessed July 1, 2022. http://opendata.hira.or.kr/op/opc/olapDiagBhvInfo.do .22. Aroor SR, Asif KS, Potter-Vig J, Sharma A, Menon BK, Inoa V, et al. Mechanical thrombectomy access for all? Challenges in increasing endovascular treatment for acute ischemic stroke in the United States. J Stroke. 2022; 24(1):41–48. PMID: 35135058.23. Hassan AE. New Technology Add-On Payment (NTAP) for Viz LVO: a win for stroke care. J Neurointerv Surg. 2021; 13(5):406–408. PMID: 33234600.24. Kim B, You SH, Jung SC. A multicenter survey of acute stroke imaging protocols for endovascular thrombectomy. Neurointervention. 2021; 16(1):20–28. PMID: 33267533.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Reperfusion therapy in acute ischemic stroke
- An Update of Recent Guideline for the Endovascular Recanalization Therapy in Acute Ischemic Stroke
- Imaging in Acute Anterior Circulation Ischemic Stroke: Current and Future
- A Multicenter Survey of Acute Stroke Imaging Protocols for Endovascular Thrombectomy
- Magnetic Resonance Imaging of the Ischemic Penumbra: Diffusion-Perfusion Mismatch in Acute Stroke Patients