Anesth Pain Med.
2020 Jul;15(3):371-377. 10.17085/apm.20028.
Performance of the MP570T pulse oximeter in volunteers participating in the controlled desaturation study: a comparison of seven probes
- Affiliations
-
- 1Department of Anesthesiology and Pain Medicine, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
- 2Department of Anesthesiology and Pain Medicine, Dankook University College of Medicine, Cheonan, Korea
- 3Department of Clinical Pharmacology and Therapeutics, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
- KMID: 2504901
- DOI: http://doi.org/10.17085/apm.20028
Abstract
- Background
The performance of the pulse oximeter was evaluated based on the ISO 80601-2-61:2011 (E) guidelines. This study aimed to determine whether the various finger probes of the MP570T pulse oximeter (MEK-ICS Co., Ltd., Korea) would provide clinically reliable peripheral oxygen saturation (SpO2) readings over a range of 70100% arterial oxygen saturation (SaO2) during non-motion conditions.
Methods
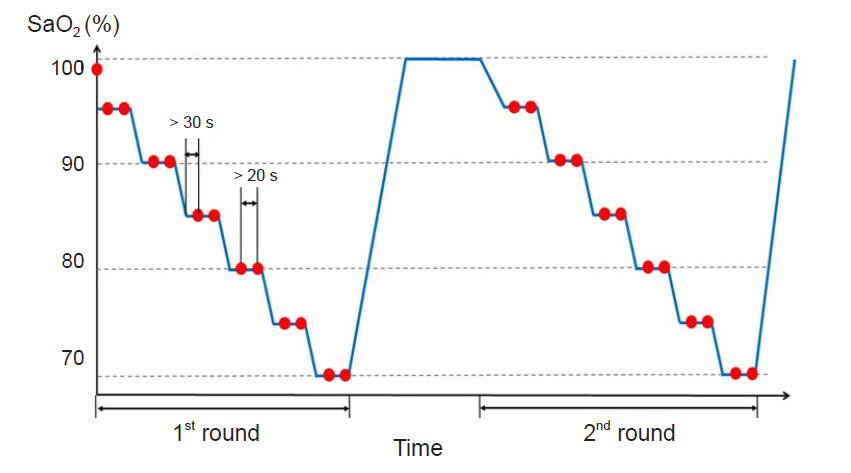
Each volunteer (n = 12) was connected to a breathing circuit for the administration of a hypoxic gas mixture. For frequent blood sampling, an arterial cannula was placed in a radial artery. The following seven pulse oximeter probes were simultaneously attached to each volunteer’s fingers: (1) WA-100 reusable finger probe (MEDNIS Co., Ltd., Korea), (2) MDNA disposable finger probe (MEDNIS Co., Ltd.), (3) IS-1011 disposable finger probe (Insung Medical Co., Ltd., Korea), (4) CJ340NA disposable finger probe (CHUN JI IN Medical Co., Ltd., Korea), (5) NellcorTM OxiMax DS-100A reusable finger probe (Medtronic, USA), (6) NellcorTM OxiMax MAX-N disposable finger probe (Medtronic), and (7) OXI-PRO DA disposable finger probe (Bio-Protech Inc., Korea).
Results
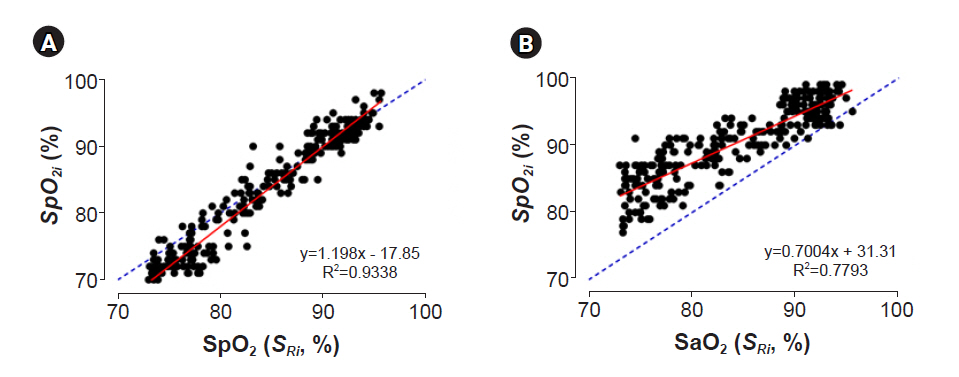
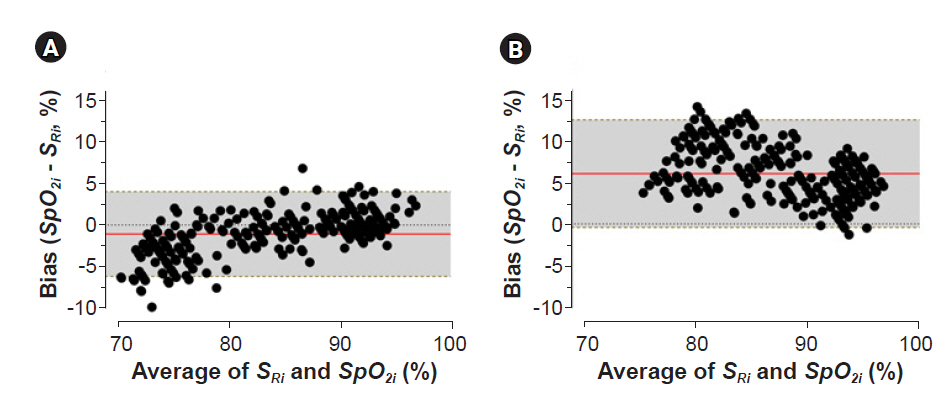
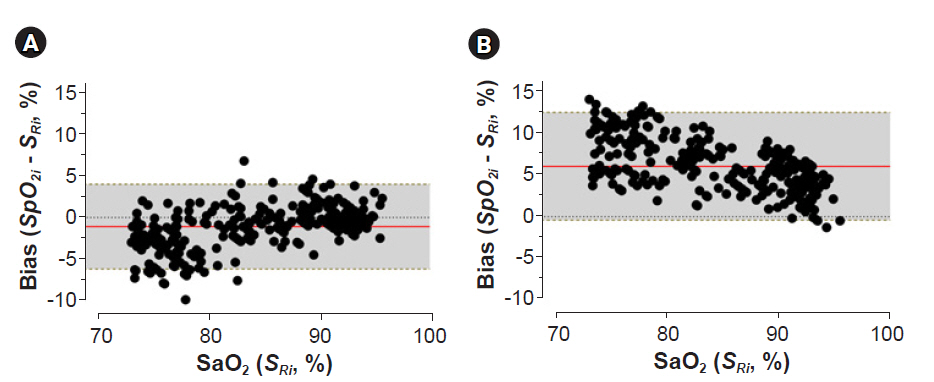
A total of 275 SpO2-SaO2 pairs were included in the analysis. The accuracy of the root mean square (Arms) of each probe was 2.83%, 3.98%, 3.75%, 6.84%, 3.43%, 5.17%, and 3.84%, respectively.
Conclusions
The MP570T pulse oximeter with WA-100 reusable, MDNA disposable, IS-1011 disposable, NellcorTM OxiMax DS-100A reusable, and OXI-PRO DA disposable finger probes meets an acceptable standard of SpO2 accuracy under non-motion conditions.
Keyword
Figure
Reference
-
1. Jubran A. Pulse oximetry. Crit Care. 2015; 19:272.2. ISO 80601-2-61:2011 Medical electrical equipment- Part 2-61: particular requirements for basic safety and essential performance of pulse oximeter equipment. ISO [serial on the Internet]. 2011 Apr [cited 2019 Oct 17]. Available from https://www.iso.org/standard/51847.html.3. Pulse oximeters- premarket notification submissions [510(k)s]: guidance for industry and Food and Drug Administration staff. U.S. Department of Health and Human Services Food and Drug Administration [serial on the Internet]. 2013 Mar 4 [cited 2020 Mar 15]. Available from https://www.fda.gov/regulatory-information/search-fda-guidance-documents/pulse-oximeters-premarket-notification-submissions-510ks-guidance-industry-and-food-and-drug.4. Matthes K, Urman R, Ehrenfeld J. Anesthesiology: a comprehensive review for the written boards and recertification. New York: Oxford University Press;2013.5. Milner QJ, Mathews GR. An assessment of the accuracy of pulse oximeters. Anaesthesia. 2012; 67:396–401.6. Bickler PE, Feiner JR, Severinghaus JW. Effects of skin pigmentation on pulse oximeter accuracy at low saturation. Anesthesiology. 2005; 102:715–9.7. Feiner JR, Severinghaus JW, Bickler PE. Dark skin decreases the accuracy of pulse oximeters at low oxygen saturation: the effects of oximeter probe type and gender. Anesth Analg. 2007; 105(6 Suppl):S18–23.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Arterial Oxygen Desaturation during Non-sedated Diagnostic Gastrointestinal Endoscopy
- Skin Burn Associated with Pulse Oximeter : A case report
- Reliability of Pulse Oximetry in Severe Hypoxemic Children with Congenital Heart Disease
- Influence of Repeated Exposures to Hypobaric Chamber on Acute Hypoxia Tolerance
- The Accuracy of Pulse Oximeter in Predicting the Arterial Oxygen Saturation