Cancer Res Treat.
2018 Jul;50(3):843-851. 10.4143/crt.2017.232.
Sarcopenia Predicts Prognosis in Patients with Newly Diagnosed Hepatocellular Carcinoma, Independent of Tumor Stage and Liver Function
- Affiliations
-
- 1Department of Hepatology, CHA Bundang Medical Center, CHA University, Seongnam, Korea. yeonjung.ha@gmail.com
- 2Department of Radiology, CHA Bundang Medical Center, CHA University, Seongnam, Korea.
- 3Department of Applied Statistics, Gachon University, Seongnam, Korea.
- KMID: 2417873
- DOI: http://doi.org/10.4143/crt.2017.232
Abstract
- PURPOSE
The purpose of this study was to demonstrate the prognostic significance of changes in body composition in patients with newly diagnosed hepatocellular carcinoma (HCC).
MATERIALS AND METHODS
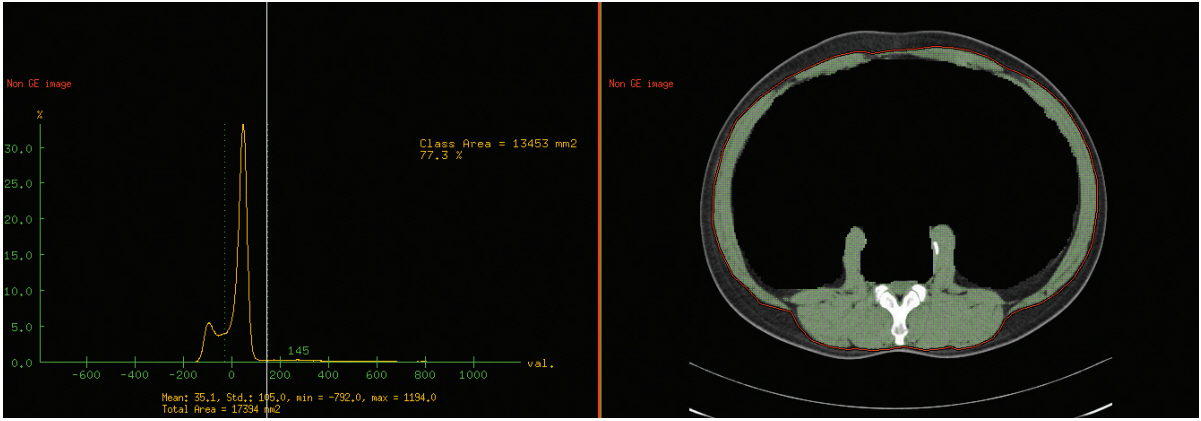
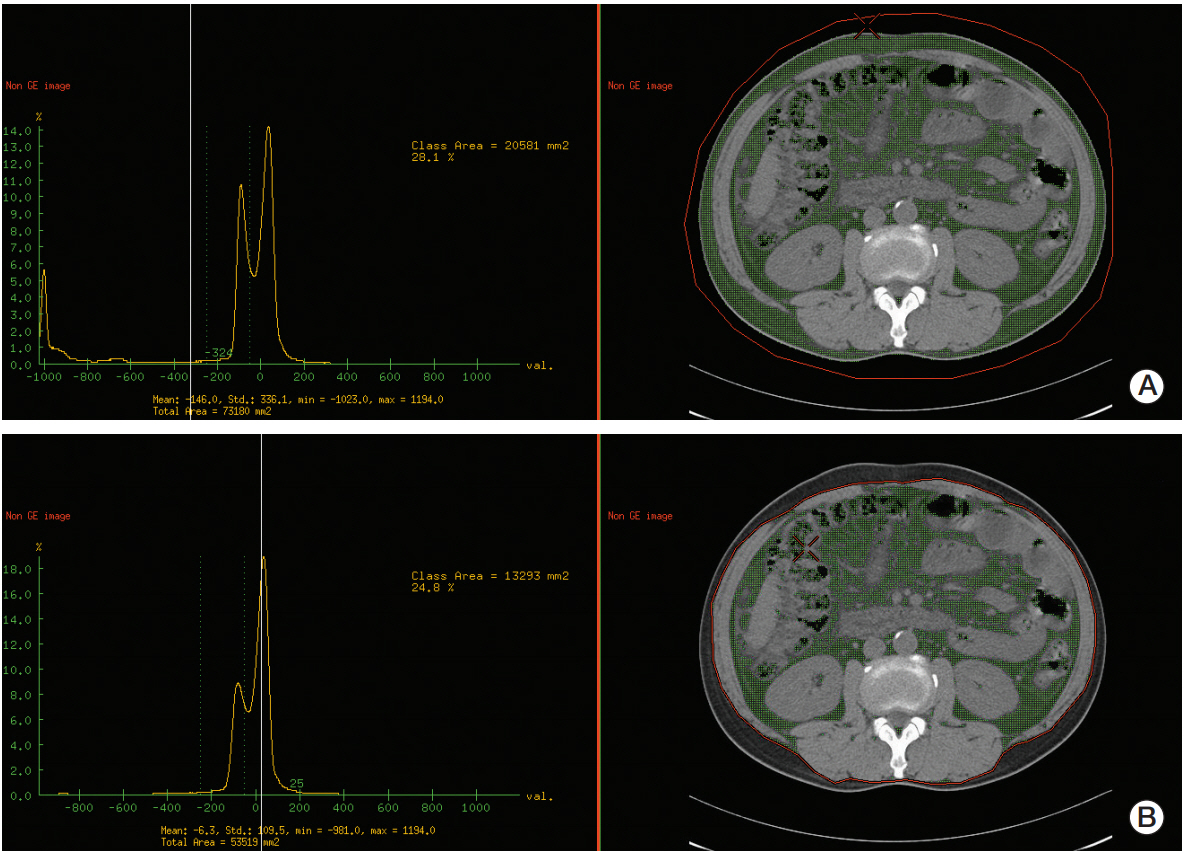
Patients (n=178) newly diagnosed with HCC participated in the study between 2007 and 2012. Areas of skeletal muscle and abdominal fat were directly measured using a three-dimensional workstation. Cox proportional-hazards modes were used to estimate the effect of baseline variables on overall survival. The inverse probability of treatmentweighting (IPTW) method was used to minimize confounding bias.
RESULTS
Cutoff values for sarcopenia, obtained from receiver-operating characteristic curves, were defined as skeletal muscle index at the third lumbar vertebra of ≤ 45.8 cm/m2 for males and ≤ 43.0 cm/m2 for females. Sarcopenia patients were older, more likely to be female, and had lower body mass index. Univariable analysis showed that the presence of sarcopenia and visceral to subcutaneous fat area ratio (VSR) were significantly associatedwith prognosis. The multivariable analyses revealed that VSR was predictive of overall survival. However, in the multivariable Cox model adjusted by IPTW, sarcopenia, not VSR, were associated with overall survival.
CONCLUSION
The presence of sarcopenia at HCC diagnosis is independently associated with survival.
MeSH Terms
Figure
Reference
-
References
1. Bosy-Westphal A, Muller MJ. Identification of skeletal muscle mass depletion across age and BMI groups in health and disease: there is need for a unified definition. Int J Obes (Lond). 2015; 39:379–86.2. Hanai T, Shiraki M, Nishimura K, Ohnishi S, Imai K, Suetsugu A, et al. Sarcopenia impairs prognosis of patients with liver cirrhosis. Nutrition. 2015; 31:193–9.
Article3. Koo HS, Kim MJ, Kim KM, Kim YS. Decreased muscle mass is not an independent risk factor for metabolic syndrome in Korean population aged 70 or older. Clin Endocrinol (Oxf). 2015; 82:509–16.
Article4. Pereira RA, Cordeiro AC, Avesani CM, Carrero JJ, Lindholm B, Amparo FC, et al. Sarcopenia in chronic kidney disease on conservative therapy: prevalence and association with mortality. Nephrol Dial Transplant. 2015; 30:1718–25.
Article5. Bryant RV, Ooi S, Schultz CG, Goess C, Grafton R, Hughes J, et al. Low muscle mass and sarcopenia: common and predictive of osteopenia in inflammatory bowel disease. Aliment Pharmacol Ther. 2015; 41:895–906.
Article6. Moon JH, Moon JH, Kim KM, Choi SH, Lim S, Park KS, et al. Sarcopenia as a predictor of future cognitive impairment in older adults. J Nutr Health Aging. 2016; 20:496–502.
Article7. Kumar A, Moynagh MR, Multinu F, Cliby WA, McGree ME, Weaver AL, et al. Muscle composition measured by CT scan is a measurable predictor of overall survival in advanced ovarian cancer. Gynecol Oncol. 2016; 142:311–6.
Article8. Shachar SS, Williams GR, Muss HB, Nishijima TF. Prognostic value of sarcopenia in adults with solid tumours: a metaanalysis and systematic review. Eur J Cancer. 2016; 57:58–67.
Article9. Park I, Choi SJ, Kim YS, Ahn HK, Hong J, Sym SJ, et al. Prognostic factors for risk stratification of patients with recurrent or metastatic pancreatic adenocarcinoma who were treated with gemcitabine-based chemotherapy. Cancer Res Treat. 2016; 48:1264–73.
Article10. Psutka SP, Boorjian SA, Moynagh MR, Schmit GD, Costello BA, Thompson RH, et al. Decreased skeletal muscle mass is associated with an increased risk of mortality after radical nephrectomy for localized renal cell cancer. J Urol. 2016; 195:270–6.
Article11. Tamandl D, Paireder M, Asari R, Baltzer PA, Schoppmann SF, Ba-Ssalamah A. Markers of sarcopenia quantified by computed tomography predict adverse long-term outcome in patients with resected oesophageal or gastro-oesophageal junction cancer. Eur Radiol. 2016; 26:1359–67.
Article12. Go SI, Park MJ, Song HN, Kim HG, Kang MH, Lee HR, et al. Prognostic impact of sarcopenia in patients with diffuse large B-cell lymphoma treated with rituximab plus cyclophosphamide, doxorubicin, vincristine, and prednisone. J Cachexia Sarcopenia Muscle. 2016; 7:567–76.
Article13. Dodson RM, Firoozmand A, Hyder O, Tacher V, Cosgrove DP, Bhagat N, et al. Impact of sarcopenia on outcomes following intra-arterial therapy of hepatic malignancies. J Gastrointest Surg. 2013; 17:2123–32.
Article14. Imai K, Takai K, Hanai T, Ideta T, Miyazaki T, Kochi T, et al. Skeletal muscle depletion predicts the prognosis of patients with hepatocellular carcinoma treated with sorafenib. Int J Mol Sci. 2015; 16:9612–24.
Article15. Voron T, Tselikas L, Pietrasz D, Pigneur F, Laurent A, Compagnon P, et al. Sarcopenia impacts on short- and long-term results of hepatectomy for hepatocellular carcinoma. Ann Surg. 2015; 261:1173–83.
Article16. Fujiwara N, Nakagawa H, Kudo Y, Tateishi R, Taguri M, Watadani T, et al. Sarcopenia, intramuscular fat deposition, and visceral adiposity independently predict the outcomes of hepatocellular carcinoma. J Hepatol. 2015; 63:131–40.
Article17. Blauwhoff-Buskermolen S, Versteeg KS, de van der Schueren MA, den Braver NR, Berkhof J, Langius JA, et al. Loss of muscle mass during chemotherapy is predictive for poor survival of patients with metastatic colorectal cancer. J Clin Oncol. 2016; 34:1339–44.18. Malietzis G, Currie AC, Johns N, Fearon KC, Darzi A, Kennedy RH, et al. Skeletal muscle changes after elective colorectal cancer resection: a longitudinal study. Ann Surg Oncol. 2016; 23:2539–47.
Article19. Yoshizumi T, Nakamura T, Yamane M, Islam AH, Menju M, Yamasaki K, et al. Abdominal fat: standardized technique for measurement at CT. Radiology. 1999; 211:283–6.
Article20. Fong C, Ratkovic M, Imai K, Hazlett C, Yang X, Peng S. CBPS: R Package for Covariate Balancing Propensity Score. R package version 0.9 [Internet]. Comprehensive R Archive Network; 2017 [cited 2017 Aug 2]. Available from: http://CRAN.R-project.org/package=CBPS).21. Kurth T, Walker AM, Glynn RJ, Chan KA, Gaziano JM, Berger K, et al. Results of multivariable logistic regression, propensity matching, propensity adjustment, and propensity-based weighting under conditions of nonuniform effect. Am J Epidemiol. 2006; 163:262–70.
Article22. Clark W, Siegel EM, Chen YA, Zhao X, Parsons CM, Hernandez JM, et al. Quantitative measures of visceral adiposity and body mass index in predicting rectal cancer outcomes after neoadjuvant chemoradiation. J Am Coll Surg. 2013; 216:1070–81.
Article23. Grignol VP, Smith AD, Shlapak D, Zhang X, Del Campo SM, Carson WE. Increased visceral to subcutaneous fat ratio is associated with decreased overall survival in patients with metastatic melanoma receiving anti-angiogenic therapy. Surg Oncol. 2015; 24:353–8.
Article24. Iwase T, Sangai T, Nagashima T, Sakakibara M, Sakakibara J, Hayama S, et al. Impact of body fat distribution on neoadjuvant chemotherapy outcomes in advanced breast cancer patients. Cancer Med. 2016; 5:41–8.
Article25. Okamura A, Watanabe M, Mine S, Nishida K, Imamura Y, Kurogochi T, et al. Clinical impact of abdominal fat distribution on prognosis after esophagectomy for esophageal squamous cell carcinoma. Ann Surg Oncol. 2016; 23:1387–94.
Article26. Kaneko G, Miyajima A, Yuge K, Yazawa S, Mizuno R, Kikuchi E, et al. Visceral obesity is associated with better recurrencefree survival after curative surgery for Japanese patients with localized clear cell renal cell carcinoma. Jpn J Clin Oncol. 2015; 45:210–6.
Article27. Lee HW, Jeong BC, Seo SI, Jeon SS, Lee HM, Choi HY, et al. Prognostic significance of visceral obesity in patients with advanced renal cell carcinoma undergoing nephrectomy. Int J Urol. 2015; 22:455–61.
Article28. Dobs AS, Boccia RV, Croot CC, Gabrail NY, Dalton JT, Hancock ML, et al. Effects of enobosarm on muscle wasting and physical function in patients with cancer: a double-blind, randomised controlled phase 2 trial. Lancet Oncol. 2013; 14:335–45.
Article29. Crawford J, Prado CM, Johnston MA, Gralla RJ, Taylor RP, Hancock ML, et al. Study design and rationale for the phase 3 clinical development program of enobosarm, a selective androgen receptor modulator, for the prevention and treatment of muscle wasting in cancer patients (POWER Trials). Curr Oncol Rep. 2016; 18:37.
Article30. Sinclair M, Grossmann M, Hoermann R, Angus PW, Gow PJ. Testosterone therapy increases muscle mass in men with cirrhosis and low testosterone: a randomised controlled trial. J Hepatol. 2016; 65:906–13.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Subclassification of Hepatocellular Carcinoma with Barcelona Clinic Liver Cancer Intermediate Stage
- 2014 KLCSG-NCC Korea Practice Guideline for the Management of Hepatocellular Carcinoma
- Sarcopenia and blood myokine levels as prognostic biomarkers in patients with liver cirrhosis or hepatocellular carcinoma
- Two-Stage Hepatectomy for Bilateral Hepatocellular Carcinoma with Bile Duct Tumor Thrombi
- Differences in radiotherapy application according to regional disease characteristics of hepatocellular carcinoma