Pediatr Gastroenterol Hepatol Nutr.
2018 Jul;21(3):189-195. 10.5223/pghn.2018.21.3.189.
Amino Acid-Based Formula in Premature Infants with Feeding Intolerance: Comparison of Fecal Calprotectin Level
- Affiliations
-
- 1Department of Pediatrics, Keimyung University School of Medicine, Daegu, Korea. jhpark.neo@gmail.com
- 2Department of Laboratory Medicine, Keimyung University School of Medicine, Daegu, Korea.
- KMID: 2415597
- DOI: http://doi.org/10.5223/pghn.2018.21.3.189
Abstract
- PURPOSE
We investigated fecal calprotectin (FC) levels in preterm infants with and without feeding intolerance (FI), and compared the FC levels according to the type of feeding.
METHODS
The medical records of 67 premature infants were reviewed retrospectively. The fully enteral-fed infants were classified into two groups; the FI group (29 infants) and the control group (31 infants). Seven infants with necrotizing enterocolitis, sepsis, and perinatal asphyxia were excluded. If breast milk (BM) or preterm formula (PF) could not be tolerated by infants with FI, amino acid-based formula (AAF) was tried temporarily. Once FI improved, AAF was discontinued, and BM or PF was resumed. We investigated the FC levels according to the type of feeding.
RESULTS
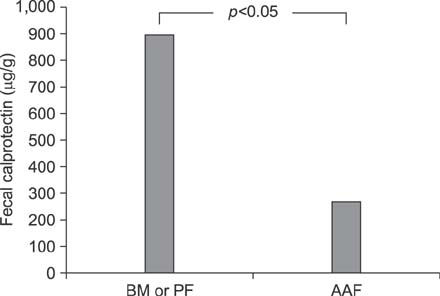
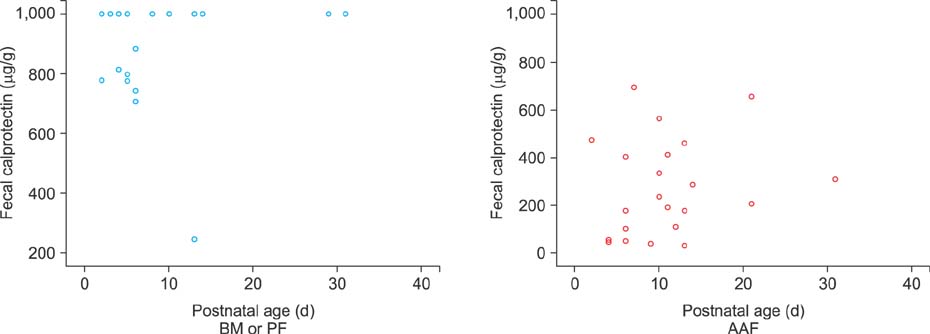
Significant differences were found in gestational age, birth weight, age when full enteral feeding was achieved, and hospital stay between the FI and control group (p < 0.05). The FC levels in the FI group were significantly higher than those in the control group (p < 0.05). The FC levels in the AAF-fed infants with FI were significantly lower than those in the BM- or PF-fed infants (p < 0.05). The growth velocities (g/d) and z scores were not significantly different between the FI and control group (p>0.05).
CONCLUSION
The FC levels in AAF-fed infants with FI showed significantly lower than those in the BM- or PF-fed infants with FI. The mitigation of gut inflammation through the decrease of FC levels in AAF-fed infants with FI could be presumed.
Keyword
MeSH Terms
Figure
Reference
-
1. Moore TA, Wilson ME. Feeding intolerance: a concept analysis. Adv Neonatal Care. 2011; 11:149–154.2. Berseth CL, Nordyke CK, Valdes MG, Furlow BL, Go VL. Responses of gastrointestinal peptides and motor activity to milk and water feedings in preterm and term infants. Pediatr Res. 1992; 31:587–590.
Article3. Stoll BJ, Hansen N, Fanaroff AA, Wright LL, Carlo WA, Ehrenkranz RA, et al. Late-onset sepsis in very low birth weight neonates: the experience of the NICHD Neonatal Research Network. Pediatrics. 2002; 110:285–291.
Article4. Stoll BJ, Hansen NI, Adams-Chapman I, Fanaroff AA, Hintz SR, Vohr B, et al. Neurodevelopmental and growth impairment among extremely low-birth-weight infants with neonatal infection. JAMA. 2004; 292:2357–2365.
Article5. Hay WW Jr. Aggressive nutrition of the preterm infant. Curr Pediatr Rep. 2013; 1:DOI: 10.1007/s40124-013-0026-.
Article6. Mansi Y, Abdelaziz N, Ezzeldin Z, Ibrahim R. Randomized controlled trial of a high dose of oral erythromycin for the treatment of feeding intolerance in preterm infants. Neonatology. 2011; 100:290–294.
Article7. Indrio F, Riezzo G, Cavallo L, Di Mauro A, Francavilla R. Physiological basis of food intolerance in VLBW. J Matern Fetal Neonatal Med. 2011; 24:Suppl 1. 64–66.
Article8. Lebenthal E, Lee PC, Heitlinger LA. Impact of development of the gastrointestinal tract on infant feeding. J Pediatr. 1983; 102:1–9.
Article9. Fanaro S. Feeding intolerance in the preterm infant. Early Hum Dev. 2013; 89:Suppl 2. S13–S20.
Article10. Hyman PE, Clarke DD, Everett SL, Sonne B, Stewart D, Harada T, et al. Gastric acid secretory function in preterm infants. J Pediatr. 1985; 106:467–471.
Article11. Hyman PE, Feldman EJ, Ament ME, Byrne WJ, Euler AR. Effect of enteral feeding on the maintenance of gastric acid secretory function. Gastroenterology. 1983; 84:341–345.
Article12. Mihatsch WA, Franz AR, Högel J, Pohlandt F. Hydrolyzed protein accelerates feeding advancement in very low birth weight infants. Pediatrics. 2002; 110:1199–1203.
Article13. Raimondi F, Spera AM, Sellitto M, Landolfo F, Capasso L. Amino acid-based formula as a rescue strategy in feeding very-low-birth-weight infants with intrauterine growth restriction. J Pediatr Gastroenterol Nutr. 2012; 54:608–612.
Article14. Fagerhol MK, Dale I, Andersson T. A radioimmunoassay for a granulocyte protein as a marker in studies on the turnover of such cells. Bull Eur Physiopathol Respir. 1980; 16:Suppl. 273–282.
Article15. Lamb CA, Mansfield JC. Measurement of faecal calprotectin and lactoferrin in inflammatory bowel disease. Frontline Gastroenterol. 2011; 2:13–18.
Article16. Moussa R, Khashana A, Kamel N, Elsharqawy SE. Fecal calprotectin levels in preterm infants with and without feeding intolerance. J Pediatr (Rio J). 2016; 92:486–492.
Article17. Pergialiotis V, Konstantopoulos P, Karampetsou N, Koutaki D, Gkioka E, Perrea DN, et al. Calprotectin levels in necrotizing enterocolitis: a systematic review of the literature. Inflamm Res. 2016; 65:847–852.
Article18. Kapel N, Campeotto F, Kalach N, Baldassare M, Butel MJ, Dupont C. Faecal calprotectin in term and preterm neonates. J Pediatr Gastroenterol Nutr. 2010; 51:542–547.
Article19. Lim JS, Lim SW, Ahn JH, Song BS, Shim KS, Hwang IT. New Korean reference for birth weight by gestational age and sex: data from the Korean Statistical Information Service (2008–2012). Ann Pediatr Endocrinol Metab. 2014; 19:146–153.
Article20. Li F, Ma J, Geng S, Wang J, Ren F, Sheng X. Comparison of the different kinds of feeding on the level of fecal calprotectin. Early Hum Dev. 2014; 90:471–475.
Article21. Zoppelli L, Güttel C, Bittrich HJ, Andrée C, Wirth S, Jenke A. Fecal calprotectin concentrations in premature infants have a lower limit and show postnatal and gestational age dependence. Neonatology. 2012; 102:68–74.
Article22. Rougé C, Butel MJ, Piloquet H, Ferraris L, Legrand A, Vodovar M, et al. Fecal calprotectin excretion in preterm infants during the neonatal period. PLoS One. 2010; 5:e11083.
Article23. Savino F, Castagno E, Calabrese R, Viola S, Oggero R, Miniero R. High faecal calprotectin levels in healthy, exclusively breast-fed infants. Neonatology. 2010; 97:299–304.
Article24. Campeotto F, Kalach N, Lapillonne A, Butel MJ, Dupont C, Kapel N. Time course of faecal calprotectin in preterm newborns during the first month of life. Acta Paediatr. 2007; 96:1531–1533.
Article25. Yang Q, Smith PB, Goldberg RN, Cotten CM. Dynamic change of fecal calprotectin in very low birth weight infants during the first month of life. Neonatology. 2008; 94:267–271.
Article26. Sangild PT. Gut responses to enteral nutrition in preterm infants and animals. Exp Biol Med (Maywood). 2006; 231:1695–1711.
Article27. Kim YJ. Enteral nutrition and its clinical application. Korean J Pediatr Gastroenterol Nutr. 2009; 12:Suppl 1. S27–S36.
Article28. Wu G, Jaeger LA, Bazer FW, Rhoads JM. Arginine deficiency in preterm infants: biochemical mechanisms and nutritional implications. J Nutr Biochem. 2004; 15:442–451.
Article29. Buddington RK, Elnif J, Puchal-Gardiner AA, Sangild PT. Intestinal apical amino acid absorption during development of the pig. Am J Physiol Regul Integr Comp Physiol. 2001; 280:R241–R247.
Article30. Bjornvad CR, Schmidt M, Petersen YM, Jensen SK, Offenberg H, Elnif J, et al. Preterm birth makes the immature intestine sensitive to feeding-induced intestinal atrophy. Am J Physiol Regul Integr Comp Physiol. 2005; 289:R1212–R1222.
Article31. Rigo J, Salle BL, Picaud JC, Putet G, Senterre J. Nutritional evaluation of protein hydrolysate formulas. Eur J Clin Nutr. 1995; 49:Suppl 1. S26–S38.32. Szajewska H, Albrecht P, Stoitiska B, Prochowska A, Gawecka A, Laskowska-Klita T. Extensive and partial protein hydrolysate preterm formulas: the effect on growth rate, protein metabolism indices, and plasma amino acid concentrations. J Pediatr Gastroenterol Nutr. 2001; 32:303–309.
Article33. Zuppa AA, Visintini F, Cota F, Maggio L, Romagnoli C, Tortorolo G. Hydrolysed milk in preterm infants: an open problem. Acta Paediatr Suppl. 2005; 94:84–86.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Fecal calprotectin concentration in neonatal necrotizing enterocolitis
- Effects of Massage Therapy on Feeding Intolerance and Physical Growth in Premature Infants
- Feeding Introlerance Due to Allergic Enterocolitis in Very Low Birth Weight Infants
- Prevalence and Predictors of Exclusive Breastfeeding in Late Preterm Infants at 12 Weeks
- Evaluation of Acid Steatocrit in Korean Infants