Korean J Gastroenterol.
2018 Jan;71(1):18-23. 10.4166/kjg.2018.71.1.18.
The Prevalence of Nontuberculous Mycobacterial Lung Disease with orwithout Reflux Esophagitis
- Affiliations
-
- 1Department of Internal Medicine, Seoul National University Bundang Hospital, Seoul National University College of Medicine, Seongnam, Korea. dhljohn@snubh.org
- KMID: 2402801
- DOI: http://doi.org/10.4166/kjg.2018.71.1.18
Abstract
- BACKGROUND/AIMS
Gastrointestinal reflux disease (GERD) is defined as "˜a condition that develops when the reflux of stomach contents causes troublesome symptoms and/or complications'. It is associated with various lung diseases, including bronchial asthma, chronic bronchitis, and bronchiectasis. GERD may also affect nontuberculous mycobacterial (NTM) lung disease. We presumed that the normal mucosal barrier of the bronchial epithelium is broken due to the aspiration of gastric juice and consequent chronic bronchial inflammation. This study investigated the prevalence of GERD in accordance with the presence or absence of NTM lung disease and analyzed the difference.
METHODS
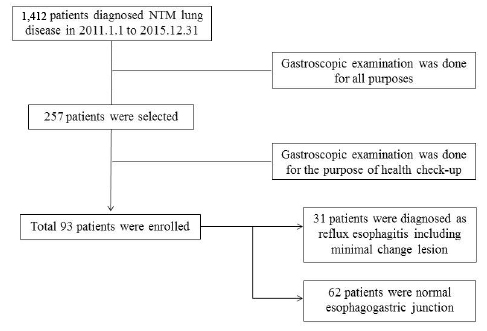
We screened patients with NTM lung disease in this hospital between January 2011 and December 2015. Among these patients, gastroscopic examinations as a health check-up were performed on 93 patients. We obtained the prevalence of Reflux esophagitis (RE) in patients with NTM and compared it with the prevalence of RE in the normal control subjects.
RESULTS
Among 93 patients with NTM, patients without RE was 66.7% (62/93). RE-minimal change was diagnosed in 29.0% (27/93), and RE LA-A was diagnosed in 4.3% (4/93). Comparing the prevalence of RE minimal change, 29.0% (27/93) had NTM and 11.9% (3043/25536) did not have NTM. This was statistically significant.
CONCLUSIONS
We showed a greater prevalence of RE minimal change in patients with NTM than those without NTM with statistical significance.
MeSH Terms
Figure
Reference
-
1. Morehead RS. Gastro-oesophageal reflux disease and non-asthma lung disease. Eur Respir Rev. 2009; 18:233–243.2. Mirsaeidi M, Hadid W, Ericsoussi B, Rodgers D, Sadikot RT. Non-tuberculous mycobacterial disease is common in patients with non-cystic fibrosis bronchiectasis. Int J Infect Dis. 2013; 17:e1000–e1004.
Article3. Koh WJ, Kwon OJ, Lee KS. Diagnosis and treatment of non-tuberculous mycobacterial pulmonary diseases: a Korean perspective. J Korean Med Sci. 2005; 20:913–925.
Article4. Koh WJ, Lee JH, Kwon YS, et al. Prevalence of gastroesophageal reflux disease in patients with nontuberculous mycobacterial lung disease. Chest. 2007; 131:1825–1830.
Article5. Thomson RM, Armstrong JG, Looke DF. Gastroesophageal reflux disease, acid suppression, and Mycobacterial avium complex pulmonary disease. Chest. 2007; 131:1166–1172.6. Griffith DE, Aksamit T, Brown-Elliott BA, et al. An official ATS/IDSA statement: diagnosis, treatment, and prevention of nontuberculous mycobacterial diseases. Am J Respir Crit Care Med. 2007; 175:367–416.
Article7. Kim BJ, Hong SK, Lee KH, et al. Differential identification of Mycobacterium tuberculosis complex and nontuberculous mycobacteria by duplex PCR assay using the RNA polymerase gene (rpoB). J Clin Microbiol. 2004; 42:1308–1312.8. Lee JH, Kim N, Chung IK, et al. Clinical significance of minimal change lesions of the esophagus in a healthy Korean population: a nationwide multi-center prospective study. J Gastroenterol Hepatol. 2008; 23(7 Pt 1):1153–1157.
Article9. Dent J. Endoscopic grading of reflux oesophagitis: the past, present and future. Best Pract Res Clin Gastroenterol. 2008; 22:585–599.
Article10. Lundell LR, Dent J, Bennett JR, et al. Endoscopic assessment of oesophagitis: clinical and functional correlates and further validation of the Los Angeles classification. Gut. 1999; 45:172–180.
Article11. Varghese G, Shepherd R, Watt P, Bruce JH. Fatal infection with Mycobacterium fortuitum associated with oesophageal achalasia. Thorax. 1988; 43:151–152.
Article12. Hadjiliadis D, Adlakha A, Prakash UB. Rapidly growing mycobacterial lung infection in association with esophageal disorders. Mayo Clin Proc. 1999; 74:45–51.13. Griffith DE, Girard WM, Wallace RJ Jr. Clinical features of pulmonary disease caused by rapidly growing mycobacteria. An analysis of 154 patients. Am Rev Respir Dis. 1993; 147:1271–1278.
Article14. Winthrop KL, McNelley E, Kendall B, et al. Pulmonary non-tuberculous mycobacterial disease prevalence and clinical features: an emerging public health disease. Am J Respir Crit Care Med. 2010; 182:977–982.15. Koh WJ, Kwon OJ, Kim EJ, Lee KS, Ki CS, Kim JW. NRAMP1 gene polymorphism and susceptibility to nontuberculous mycobacterial lung diseases. Chest. 2005; 128:94–101.
Article16. Linden SK, Sutton P, Karlsson NG, Korolik V, McGuckin MA. Mucins in the mucosal barrier to infection. Mucosal Immunol. 2008; 1:183–197.
Article17. Werther JL. The gastric mucosal barrier. Mt Sinai J Med. 2000; 67:41–53.18. Mercer RR, Russell ML, Crapo JD. Mucous lining layers in human and rat airways. Am Rev Respir Dis. 1992; 145:355.19. Strugala V, Allen A, Dettmar PW, Pearson JP. Colonic mucin: methods of measuring mucus thickness. Proc Nutr Soc. 2003; 62:237–243.
Article20. Jordan N, Newton J, Pearson J, Allen A. A novel method for the visualization of the in situ mucus layer in rat and man. Clin Sci (Lond). 1998; 95:97–106.
Article21. Atuma C, Strugala V, Allen A, Holm L. The adherent gastrointestinal mucus gel layer: thickness and physical state in vivo. Am J Physiol Gastrointest Liver Physiol. 2001; 280:G922–G929.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Respiratory Review of 2009: Nontuberculous Mycobacterium
- The Role of Helicobacter Pylori Infection in Reflux Esophagitis
- Diagnosis and Treatment of Gastroesophageal Reflux Disease
- The prevalence and associated factors of reflux esophagitis in routine check-up subjects
- Reflux esophagitis and its relationship to hiatal hernia