Risk Factors for Recurrent High-Risk Polyps after the Removal of High-Risk Polyps at Initial Colonoscopy
- Affiliations
-
- 1Department of Internal Medicine, Institute of Gastroenterology, Yonsei University College of Medicine, Seoul, Korea. taeilkim@yuhs.ac
- KMID: 2345883
- DOI: http://doi.org/10.3349/ymj.2015.56.6.1559
Abstract
- PURPOSE
Colonoscopic polypectomy and surveillance are important to prevent colorectal cancer and identify additional relative risk factors for adequate surveillance. In this study, we evaluated risk factors related to recurrent high-risk polyps during the surveillance of patients with high-risk polyps.
MATERIALS AND METHODS
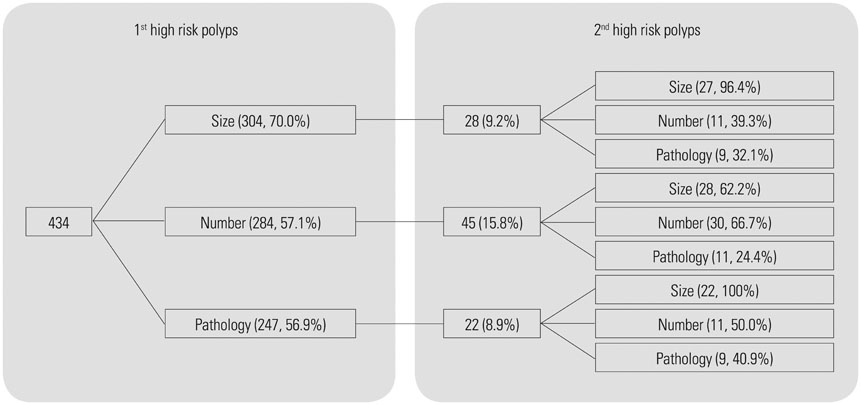
We included 434 patients who had high-risk polyps (adenoma > or =10 mm, > or =3 adenomas, villous histology, or high-grade dysplasia) on the baseline colonoscopy and underwent at least one surveillance colonoscopy from 2005 to 2011 at Severance Hospital. Data regarding patient characteristics, bowel preparation and polyp size, location, number, and pathological diagnosis were retrospectively collected from medical records. Patients with recurrent high-risk polyps were compared with patients with low-risk or no polyps during surveillance.
RESULTS
Patients were predominantly male (77.4%), with a mean age of 61.0+/-8.6 years and mean follow-up of 1.5+/-0.8 years. High-risk polyps recurred during surveillance colonoscopy in 51 (11.8%) patients. Results of multivariate analysis showed that male gender, poor bowel preparation, and a larger number of adenomas were independent risk factors for recurrent high-risk polyps (p=0.047, 0.01, and <0.001, respectively). Compared with high-risk polyps found during initial colonoscopy, high-risk polyps on surveillance colonoscopy had higher proportions of small adenomas, low-risk pathology, and fewer adenomas overall, but there was no difference in location.
CONCLUSION
Male patients and those with poor bowel preparation for colonoscopy or higher numbers of adenomas were more likely to experience recurrent high-risk polyps.
Keyword
MeSH Terms
Figure
Cited by 6 articles
-
Long-Term Outcome and Surveillance Colonoscopy after Successful Endoscopic Treatment of Large Sessile Colorectal Polyps
Bun Kim, A Ra Choi, Soo Jung Park, Jae Hee Cheon, Tae Il Kim, Won Ho Kim, Sung Pil Hong
Yonsei Med J. 2016;57(5):1106-1114. doi: 10.3349/ymj.2016.57.5.1106.Commentary on “Comparative Study of Narrow-Band Imaging and i-scan for Predicting the Histology of Intermediate-to-Large Colorectal Polyps: A Prospective, Randomized Pilot Study”
Yunho Jung, Masayuki Kato
Clin Endosc. 2021;54(6):781-782. doi: 10.5946/ce.2021.206.Korean guidelines for postpolypectomy colonoscopic surveillance: 2022 revised edition
Su Young Kim, Min Seob Kwak, Soon Man Yoon, Yunho Jung, Jong Wook Kim, Sun-Jin Boo, Eun Hye Oh, Seong Ran Jeon, Seung-Joo Nam, Seon-Young Park, Soo-Kyung Park, Jaeyoung Chun, Dong Hoon Baek, Mi-Young Choi, Suyeon Park, Jeong-Sik Byeon, Hyung Kil Kim, Joo Young Cho, Moon Sung Lee, Oh Young Lee
Clin Endosc. 2022;55(6):703-725. doi: 10.5946/ce.2022.136.Three-year colonoscopy surveillance after polypectomy in Korea: a Korean Association for the Study of Intestinal Diseases (KASID) multicenter prospective study
Won Seok Choi, Dong Soo Han, Chang Soo Eun, Dong Il Park, Jeong-Sik Byeon, Dong-Hoon Yang, Sung-Ae Jung, Sang Kil Lee, Sung Pil Hong, Cheol Hee Park, Suck-Ho Lee, Jeong-Seon Ji, Sung Jae Shin, Bora Keum, Hyun Soo Kim, Jung Hye Choi, Sin-Ho Jung
Intest Res. 2018;16(1):126-133. doi: 10.5217/ir.2018.16.1.126.Korean Guidelines for Postpolypectomy Colonoscopic Surveillance: 2022 revised edition
Su Young Kim, Min Seob Kwak, Soon Man Yoon, Yunho Jung, Jong Wook Kim, Sun-Jin Boo, Eun Hye Oh, Seong Ran Jeon, Seung-Joo Nam, Seon-Young Park, Soo-Kyung Park, Jaeyoung Chun, Dong Hoon Baek, Mi-Young Choi, Suyeon Park, Jeong-Sik Byeon, Hyung Kil Kim, Joo Young Cho, Moon Sung Lee, Oh Young Lee
Intest Res. 2023;21(1):20-42. doi: 10.5217/ir.2022.00096.Clinical characteristics and risk factors related to polyposis recurrence and advanced neoplasm development among patients with non-hereditary colorectal polyposis
Jihun Jang, Jihye Park, Soo Jung Park, Jae Jun Park, Jae Hee Cheon, Tae Il Kim
Intest Res. 2023;21(4):510-517. doi: 10.5217/ir.2022.00139.
Reference
-
1. Winawer SJ, Zauber AG, Ho MN, O'Brien MJ, Gottlieb LS, Sternberg SS, et al. Prevention of colorectal cancer by colonoscopic polypectomy. The National Polyp Study Workgroup. N Engl J Med. 1993; 329:1977–1981.
Article2. Baxter NN, Goldwasser MA, Paszat LF, Saskin R, Urbach DR, Rabeneck L. Association of colonoscopy and death from colorectal cancer. Ann Intern Med. 2009; 150:1–8.
Article3. Bertario L, Russo A, Sala P, Pizzetti P, Ballardini G, Andreola S, et al. Predictors of metachronous colorectal neoplasms in sporadic adenoma patients. Int J Cancer. 2003; 105:82–87.
Article4. Lieberman DA, Rex DK, Winawer SJ, Giardiello FM, Johnson DA, Levin TR, et al. Guidelines for colonoscopy surveillance after screening and polypectomy: a consensus update by the US Multi-Society Task Force on Colorectal Cancer. Gastroenterology. 2012; 143:844–857.
Article5. Lieberman DA, Weiss DG, Harford WV, Ahnen DJ, Provenzale D, Sontag SJ, et al. Five-year colon surveillance after screening colonoscopy. Gastroenterology. 2007; 133:1077–1085.
Article6. Imperiale TF, Glowinski EA, Lin-Cooper C, Larkin GN, Rogge JD, Ransohoff DF. Five-year risk of colorectal neoplasia after negative screening colonoscopy. N Engl J Med. 2008; 359:1218–1224.
Article7. Leung WK, Lau JY, Suen BY, Wong GL, Chow DK, Lai LH, et al. Repeat-screening colonoscopy 5 years after normal baseline-screening colonoscopy in average-risk Chinese: a prospective study. Am J Gastroenterol. 2009; 104:2028–2034.
Article8. Brenner H, Haug U, Arndt V, Stegmaier C, Altenhofen L, Hoffmeister M. Low risk of colorectal cancer and advanced adenomas more than 10 years after negative colonoscopy. Gastroenterology. 2010; 138:870–876.
Article9. Miller HL, Mukherjee R, Tian J, Nagar AB. Colonoscopy surveillance after polypectomy may be extended beyond five years. J Clin Gastroenterol. 2010; 44:e162–e166.
Article10. Chung SJ, Kim YS, Yang SY, Song JH, Kim D, Park MJ, et al. Five-year risk for advanced colorectal neoplasia after initial colonoscopy according to the baseline risk stratification: a prospective study in 2452 asymptomatic Koreans. Gut. 2011; 60:1537–1543.
Article11. Martínez ME, Baron JA, Lieberman DA, Schatzkin A, Lanza E, Winawer SJ, et al. A pooled analysis of advanced colorectal neoplasia diagnoses after colonoscopic polypectomy. Gastroenterology. 2009; 136:832–841.
Article12. Martínez ME, Thompson P, Messer K, Ashbeck EL, Lieberman DA, Baron JA, et al. One-year risk for advanced colorectal neoplasia: US versus UK risk-stratification guidelines. Ann Intern Med. 2012; 157:856–864.
Article13. Martínez ME, Sampliner R, Marshall JR, Bhattacharyya AK, Reid ME, Alberts DS. Adenoma characteristics as risk factors for recurrence of advanced adenomas. Gastroenterology. 2001; 120:1077–1083.
Article14. Bonithon-Kopp C, Piard F, Fenger C, Cabeza E, O'Morain C, Kronborg O, et al. Colorectal adenoma characteristics as predictors of recurrence. Dis Colon Rectum. 2004; 47:323–333.
Article15. Kim WH, Cho YJ, Park JY, Min PK, Kang JK, Park IS. Factors affecting insertion time and patient discomfort during colonoscopy. Gastrointest Endosc. 2000; 52:600–605.
Article16. Hong SN, Yang DH, Kim YH, Hong SP, Shin SJ, Kim SE, et al. [Korean guidelines for post-polypectomy colonoscopic surveillance]. Korean J Gastroenterol. 2012; 59:99–117.
Article17. Harewood GC, Sharma VK, de Garmo P. Impact of colonoscopy preparation quality on detection of suspected colonic neoplasia. Gastrointest Endosc. 2003; 58:76–79.
Article18. Lebwohl B, Wang TC, Neugut AI. Socioeconomic and other predictors of colonoscopy preparation quality. Dig Dis Sci. 2010; 55:2014–2020.
Article19. Kazarian ES, Carreira FS, Toribara NW, Denberg TD. Colonoscopy completion in a large safety net health care system. Clin Gastroenterol Hepatol. 2008; 6:438–442.
Article20. Lebwohl B, Kastrinos F, Glick M, Rosenbaum AJ, Wang T, Neugut AI. The impact of suboptimal bowel preparation on adenoma miss rates and the factors associated with early repeat colonoscopy. Gastrointest Endosc. 2011; 73:1207–1214.
Article21. Chokshi RV, Hovis CE, Hollander T, Early DS, Wang JS. Prevalence of missed adenomas in patients with inadequate bowel preparation on screening colonoscopy. Gastrointest Endosc. 2012; 75:1197–1203.
Article22. Saini SD, Kim HM, Schoenfeld P. Incidence of advanced adenomas at surveillance colonoscopy in patients with a personal history of colon adenomas: a meta-analysis and systematic review. Gastrointest Endosc. 2006; 64:614–626.
Article23. Noshirwani KC, van Stolk RU, Rybicki LA, Beck GJ. Adenoma size and number are predictive of adenoma recurrence: implications for surveillance colonoscopy. Gastrointest Endosc. 2000; 51(4 Pt 1):433–437.
Article24. van Stolk RU, Beck GJ, Baron JA, Haile R, Summers R. Adenoma characteristics at first colonoscopy as predictors of adenoma recurrence and characteristics at follow-up. The Polyp Prevention Study Group. Gastroenterology. 1998; 115:13–18.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Factors Predictive of High-Risk Adenomas at the Third Colonoscopy after Initial Adenoma Removal
- Importance of Early Follow-up Colonoscopy in Patients at High Risk for Colorectal Polyps
- Characteristics and Risk Factors of Synchronous and Metachronous Polyp in Colorectal Cancer
- Synchronous Lesions in Colorectal Cancer
- Recent Updates on Management and Follow-up of Gallbladder Polyps