Korean J Perinatol.
2014 Jun;25(2):91-94. 10.14734/kjp.2014.25.2.91.
Discrepancy between Non-stress Test Result and Umbilical Artery Doppler Study in a Pregnancy Complicated by Diabetes; A Case Report
- Affiliations
-
- 1Department of Obstetrics and Gynecology, Inje University College of Medicine, Ilsan-Paik Hospital, Gyeonggi, Korea. jwjwpark@gmail.com
- KMID: 2280959
- DOI: http://doi.org/10.14734/kjp.2014.25.2.91
Abstract
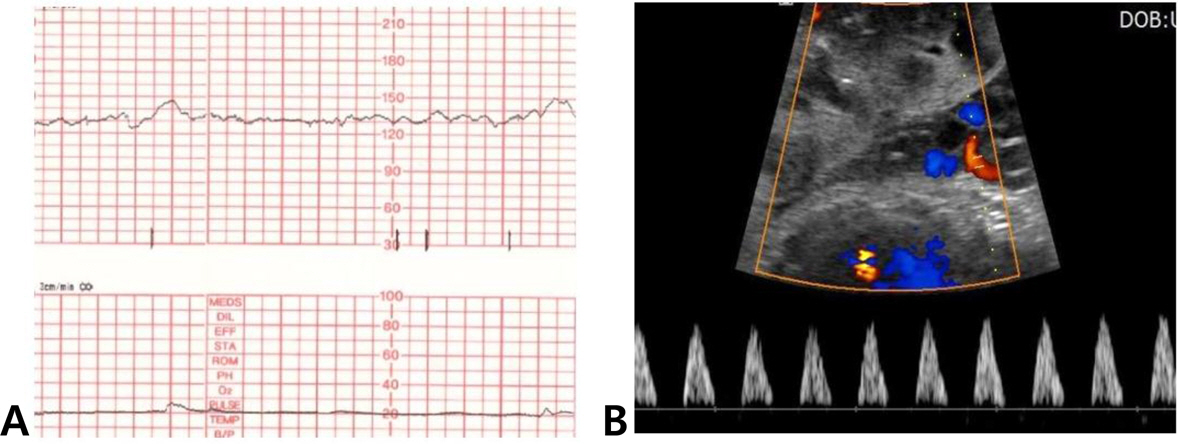
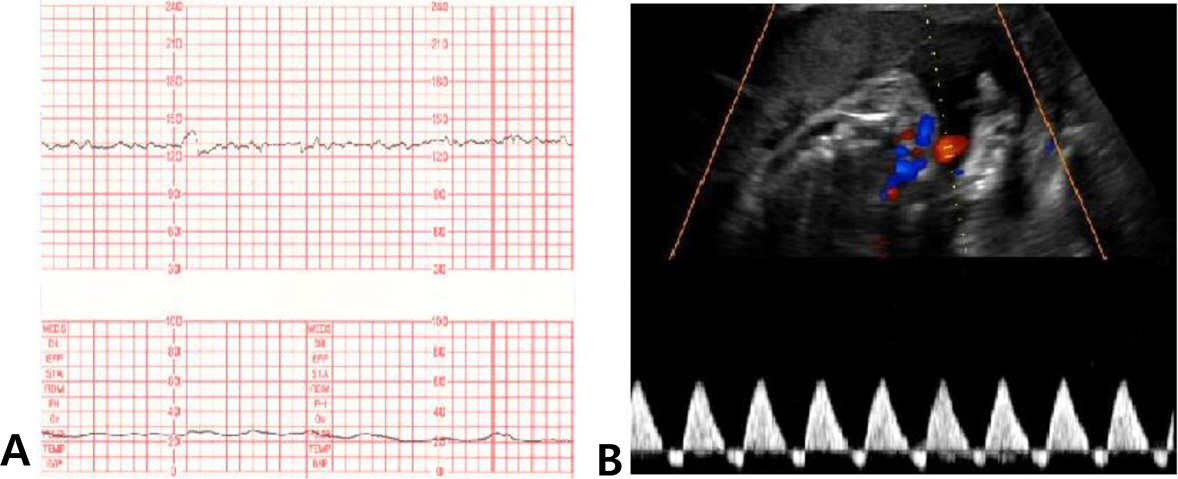
- Pregestational diabetes is a well-known risk factor for perinatal mortality, and regarded as an important cause of stillbirth. Unfortunately, more than half of stillbirths remain unexplained. Nevertheless, there is no consensus regarding the optimal timing and content of antepartum testing in pregnancies complicated by diabetes. A 32-year-old primigravida presented with diabetes diagnosed during pregnancy. Antenatal fetal surveillance tests including nonstress test, biophysical profile, and Doppler waveforms of umbilical arteries were performed twice weekly, beginning at 32 weeks gestation. At 37(+4) weeks' gestation, a discrepancy in the surveillance test results arose when reversed end-diastolic flow in the umbilical arteries was seen, despite a reactive nonstress test. A male baby was delivered by cesarean section. The umbilical arterial pH at delivery was 7.171. Antenatal fetal surveillance in pregnancies complicated by diabetes should include evaluation of Doppler waveforms in the umbilical vessels, regardless of the presence or absence of maternal vasculopathy.
MeSH Terms
Figure
Reference
-
1.von Kries R., Kimmerle R., Schmidt JE., Hachmeister A., Bohm O., Wolf HG. Pregnancy outcomes in mothers with pregestational diabetes: a population-based study in North Rhine (Germany) from 1988 to 1993. Eur J Pediatr. 1997. 156:963–7.
Article2.Yang J., Cummings EA., O'Connell C., Jangaard K. Fetal and neonatal outcomes of diabetic pregnancies. Obstet Gynecol. 2006. 108:644–50.
Article3.Melamed N., Hod M. Perinatal mortality in pregestational diabetes. Int J Gynaecol Obstet. 2009. 104(Suppl 1):S20–4.
Article4.Mathiesen ER., Ringholm L., Damm P. Stillbirth in diabetic pregnancies. Best Pract Res Clin Obstet Gynaecol. 2011. 25:105–11.
Article5.ACOG Practice Bulletin. Clinical Management Guidelines for Obstetrician-Gynecologists. Number 60, March 2005. Pregestational diabetes mellitus. Obstet Gynecol. 2005. 105:675–85.6.Reece EA., Coustan DR. Diabetes mellitus in pregnancy: Principles and practice: Churchill Livingstone. 1988.7.Salvesen DR., Brudenell JM., Proudler AJ., Crook D., Nicolaides KH. Fetal pancreatic beta-cell function in pregnancies complicated by maternal diabetes mellitus: relationship to fetal acidemia and macrosomia. Am J Obstet Gynecol. 1993. 168:1363–9.8.Bradley R., Brudenell J., Nicolaides K. Fetal acidosis and hyperlacticaemia diagnosed by cordocentesis in pregnancies complicated by maternal diabetes mellitus. Diabet Med. 1991. 8:464–8.
Article9.Philipps A., Porte P., Stabinsky S., Rosenkrantz T., Raye J. Effects of chronic fetal hyperglycemia upon oxygen consumption in the ovine uterus and conceptus. J Clin Invest. 1984. 74:279–86.
Article10.Salvesen DR., Freeman J., Brudenell JM., Nicolaides KH. Prediction of fetal acidaemia in pregnancies complicated by maternal diabetes mellitus by biophysical profile scoring and fetal heart rate monitoring. BJOG. 1993. 100:227–33.
Article11.Richey SD., Sandstad JS., Leveno KJ. Observations concerning “unexplained” fetal demise in pregnancy complicated by diabetes mellitus. J Matern Fetal Neonatal Med. 1995. 4:169–72.
Article12.Daskalakis G., Marinopoulos S., Krielesi V., Papapanagiotou A., Papantoniou N., Mesogitis S, et al. Placental pathology in women with gestational diabetes. Acta Obstet Gynecol Scand. 2008. 87:403–7.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Pregnancy outcomes following uterince artery and umbilical artery doppler velicimetry
- Comparison of doppler umbilical artery flow velocimetry and neonates test in predicting pregnancy outcomes
- Pseudo-Single Umbilical Artery by Spontaneous Intrauterine Umbilical Artery Thrombosis
- The Application of Doppler Ultrasound in the Assessment of Fetal Weight
- The Relationship between Umbilical-Cerebral Doppler Ratio and Umbilical Artery Gas Analysis