Ann Dermatol.
2011 Dec;23(Suppl 3):S299-S302. 10.5021/ad.2011.23.S3.S299.
Correction of Pincer Nail Deformity Using Dermal Grafting
- Affiliations
-
- 1Department of Dermatology, Wonkwang University School of Medicine, Iksan, Korea. derma@chol.com
- 2Institute of Wonkwang Medical Science, Wonkwang University School of Medicine, Iksan, Korea.
- 3Division of Beauty Design, Wonkwang University, Iksan, Korea.
- KMID: 2171856
- DOI: http://doi.org/10.5021/ad.2011.23.S3.S299
Abstract
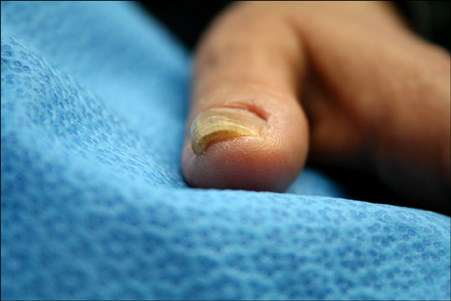
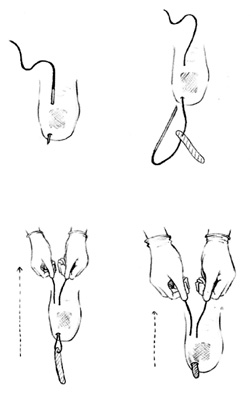
- Pincer nail deformity is characterized by excessive curvature and distortion of the nail in the transverse dimension, and particularly at the distal part of the nail plate. This deformity leads to pinching off and loss of soft tissue in the affected digit, causing severe pain. Many treatment methods have been proposed; however, an effective long-term method preserving the nail matrix has not yet been established. We present here a case of pincer nail in the left thumb in a 49-year-old woman who was treated successfully with dermal grafting under the nail bed. We describe the surgical method and the treatment results. To the best of our knowledge, this is the first report in the Korean medical literature on the use of dermal grafting for the treatment of pincer nail deformity.
Keyword
Figure
Cited by 1 articles
-
The Polyonychia and Distal Phalangeal Bone Underdevelopment on Right Second Toe
Dong Hyuk Eun, Jun Hong Park, Han Jin Jung, Yong Hyun Jang, Seok-Jong Lee, Do Won Kim, Weon Ju Lee
Ann Dermatol. 2018;30(1):105-106. doi: 10.5021/ad.2018.30.1.105.
Reference
-
1. Baran R, Dawber RPR, De Berker AR, Haneke E, Tosti A. Transverse overcurvature of the nail. Baran & Dawber's diseases of the nails and their management. 2001. 3rd ed. New York: Blackwell Science;54–55.2. Cornelius CE 3rd, Shelley WB. Pincer nail syndrome. Arch Surg. 1968. 96:321–322.
Article3. Zook EG, Chalekson CP, Brown RE, Neumeister MW. Correction of pincer-nail deformities with autograft or homograft dermis: modified surgical technique. J Hand Surg Am. 2005. 30:400–403.
Article4. Moon HS, Son SJ, Park K, Park HJ. A clinical study of efficacy of surgical management for pincer nails. Korean J Dermatol. 2009. 47:509–515.5. Effendy I, Ossowski B, Happle R. Pincer nail. Conservative correction by attachment of a plastic brace. Hautarzt. 1993. 44:800–802.6. Kim HJ, Ha DJ, Sim WY, Lee MH, Haw CR, Kim NI. The therapeutic effect of nail splinting in ingrown toenails. Korean J Dermatol. 2001. 39:855–860.7. Baran R, Haneke E, Richert B. Pincer nails: definition and surgical treatment. Dermatol Surg. 2001. 27:261–266.
Article8. Kim KD, Ha DJ, Sim WY. A case of pincer nail treated with nail plate separation. Korean J Dermatol. 2001. 39:1425–1427.9. Hatoko M, Iioka H, Tanaka A, Kuwahara M, Yurugi S, Niitsuma K. Hard-palate mucosal graft in the management of severe pincer-nail deformity. Plast Reconstr Surg. 2003. 112:835–839.
Article10. Mimouni D, Ben-Amitai D. Hereditary pincer nail. Cutis. 2002. 69:51–53.11. Suzuki K, Yagi I, Kondo M. Surgical treatment of pincer nail syndrome. Plast Reconstr Surg. 1979. 63:570–573.
Article12. Yun SK, You MY, Lee JS. Surgical treatment of pincer nail associated with osteophyte. Korean J Dermatol. 2000. 38:1215–1217.13. Brown RE, Zook EG, Williams J. Correction of pincer-nail deformity using dermal grafting. Plast Reconstr Surg. 2000. 105:1658–1661.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Pincer Nail Deformity Treated with Widening of the Nail Bed
- Significance of Surgery to Correct Anatomical Alterations in Pincer Nails
- The Effectiveness of Surgical Correction of Pincer Nails Using Nail Bed Flap and Bilateral Partial Matrixectomy, with or without Osteophyte Removal
- A Case of Heredetary Pincer Nail Treated with Nail Grinding Method
- Nail Plate and Bed Reconstruction for Pincer Nail Deformity