J Korean Med Sci.
2014 Jan;29(1):98-105. 10.3346/jkms.2014.29.1.98.
A Randomized Controlled Trial of Comparison on Time and Rate of Cecal and Termianl Ileal Intubation according to Adult-Colonoscope Length: Intermediate versus Long
- Affiliations
-
- 1Health Promotion Center, Ajou University School of Medicine, Suwon, Korea. drhwa@hanmail.net
- 2Department of Gastroenterology, Ajou University School of Medicine, Suwon, Korea.
- 3Health Promotion Center, Wonkwang University College of Medicine, Gunpo, Korea.
- KMID: 1796921
- DOI: http://doi.org/10.3346/jkms.2014.29.1.98
Abstract
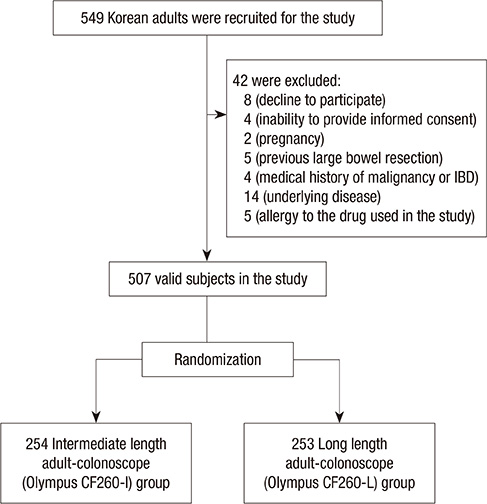
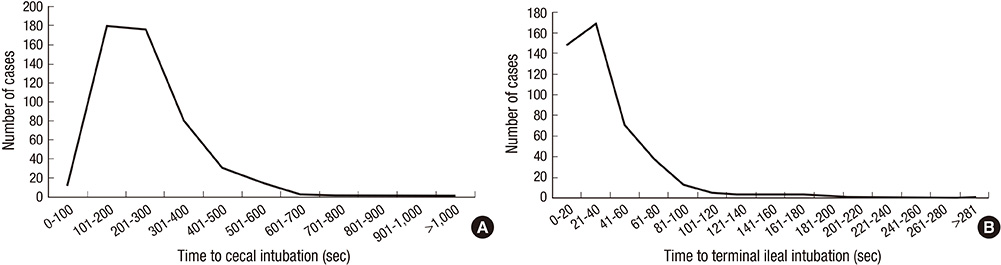
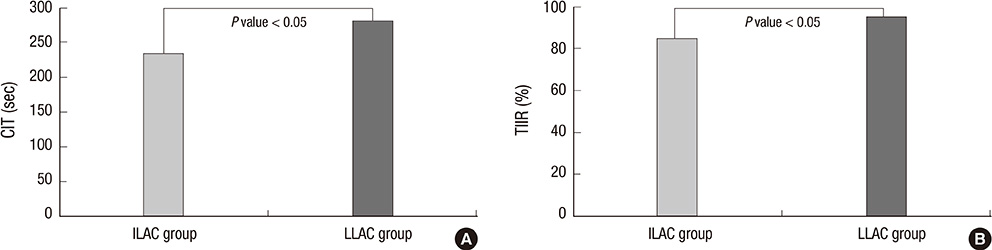
- For a complete colonoscopic examination, a high intubation rate and a short intubation time have been demanded to colonoscopists, if possible. The aim of the present study was to compare these examination parameters, intubation time and rate, according to the length of colonoscope. A total of 507 healthy Korean subjects were randomly assigned into two groups: intermediate length adult-colonoscope (n=254) and long length adult-colonoscope (n=253). There were significant differences in cecal intubation time and in terminal ileal intubation rate according to the length of the colonoscope. Time-to-cecal intubation was shorter for the intermediate-scope group than for the long-scope group (234.2 +/- 115.0 sec vs 280.7 +/- 135.0 sec, P < 0.001). However, the success rate of terminal ileal intubation was higher in the long-scope group than in the intermediate-scope group (95.3% vs 84.3%, P < 0.001). There were no significant differences in other colonoscopic parameters between the two groups. The intermediate length adult-colonoscope decreased the time to reach the cecum, whereas the long-scope showed a success rate of terminal ileal intubation. These findings suggest that it is reasonable to prepare and use these two types of colonoscope appropriate to the needs of the patient and examination, instead of employing only one type of colonoscope.
MeSH Terms
Figure
Reference
-
1. Siegel R, Naishadham D, Jemal A. Cancer statistics, 2013. CA Cancer J Clin. 2013; 63:11–30.2. Sung JJ, Lau JY, Goh KL, Leung WK. Asia Pacific Working Group on Colorectal Cancer. Increasing incidence of colorectal cancer in Asia: implications for screening. Lancet Oncol. 2005; 6:871–876.3. Jung KW, Park S, Kong HJ, Won YJ, Boo YK, Shin HR, Park EC, Lee JS. Cancer statistics in Korea: incidence, mortality and survival in 2006-2007. J Korean Med Sci. 2010; 25:1113–1121.4. Kim YJ. What is a reasonable screening test for colorectal cancer. J Korean Soc Coloproctol. 2010; 26:375.5. Bertelson NL, Kalkbrenner KA, Merchea A, Dozois EJ, Landmann RG, De Petris G, Young-Fadok TM, Etzioni DA. Colectomy for endoscopically unresectable polyps: how often is it cancer? Dis Colon Rectum. 2012; 55:1111–1116.6. Baik SH, Lee KS, Jeong SY, Park YK, Kim HS, Lee DH, Oh HJ, Kim BC. Korean Academy of Medical Sciences. Development of a rating system for digestive system impairments: Korean Academy of Medical Sciences Guideline. J Korean Med Sci. 2009; 24:S271–S276.7. Choi YS, Lee JB, Lee EJ, Lee SH, Suh JP, Lee DH, Kim do S, Youk EG. Can endoscopic submucosal dissection technique be an alternative treatment option for a difficult giant (≥ 30 mm) pedunculated colorectal polyp? Dis Colon Rectum. 2013; 56:660–666.8. Zuber-Jerger I, Endlicher E, Gelbmann CM. Factors affecting cecal and ileal intubation time in colonoscopy. Med Klin (Munich). 2008; 103:477–481.9. Kim WH, Cho YJ, Park JY, Min PK, Kang JK, Park IS. Factors affecting insertion time and patient discomfort during colonoscopy. Gastrointest Endosc. 2000; 52:600–605.10. Hsu CM, Lin WP, Su MY, Chiu CT, Ho YP, Chen PC. Factors that influence cecal intubation rate during colonoscopy in deeply sedated patients. J Gastroenterol Hepatol. 2012; 27:76–80.11. Bernstein C, Thorn M, Monsees K, Spell R, O'Connor JB. A prospective study of factors that determine cecal intubation time at colonoscopy. Gastrointest Endosc. 2005; 61:72–75.12. Arcovedo R, Larsen C, Reyes HS. Patient factors associated with a faster insertion of the colonoscope. Surg Endosc. 2007; 21:885–888.13. Krishnan P, Sofi AA, Dempsey R, Alaradi O, Nawras A. Body mass index predicts cecal insertion time: the higher, the better. Dig Endosc. 2012; 24:439–442.14. Hsieh YH, Kuo CS, Tseng KC, Lin HJ. Factors that predict cecal insertion time during sedated colonoscopy: the role of waist circumference. J Gastroenterol Hepatol. 2008; 23:215–217.15. Rex DK. Effect of variable stiffness colonoscopes on cecal intubation times for routine colonoscopy by an experienced examiner in sedated patients. Endoscopy. 2001; 33:60–64.16. Sola-Vera J, Uceda F, Brotons A, Sáez J, Girona E, Pérez E, Picó MD, Grau C, Sillero C. Does the use of a variable stiffness colonoscope offer advantages during colonoscopy under deep sedation? results of a randomized trial. Eur J Gastroenterol Hepatol. 2011; 23:593–597.17. Barthel J, Hinojosa T, Shah N. Colonoscope length and procedure efficiency. J Clin Gastroenterol. 1995; 21:30–32.18. Dickey W, Garrett D. Colonoscope length and procedure efficiency. Am J Gastroenterol. 2002; 97:79–82.19. Hsieh YH, Zhou AL, Lin HJ. Long pediatric colonoscope versus intermediate length adult colonoscope for colonoscopy. J Gastroenterol Hepatol. 2008; 23:e7–e10.20. Shumaker DA, Zaman A, Katon RM. A randomized controlled trial in a training institution comparing a pediatric variable stiffness colonoscope, a pediatric colonoscope, and an adult colonoscope. Gastrointest Endosc. 2002; 55:172–179.21. Marshall JB. Use of a pediatric colonoscope improves the success of total colonoscopy in selected adult patients. Gastrointest Endosc. 1996; 44:675–678.22. Saifuddin T, Trivedi M, King PD, Madsen R, Marshall JB. Usefulness of a pediatric colonoscope for colonoscopy in adults. Gastrointest Endosc. 2000; 51:314–317.23. De Silva AP, Kumarasena RS, Perera Keragala SD, Kalubowila U, Niriella M, Dassanayake AS, Pathmeswaran A, de Silva HJ. The prone 12 o'clock position reduces ileal intubation time during colonoscopy compared to the left lateral 6 o'clock (standard) position. BMC Gastroenterol. 2011; 11:89.24. Powell N, Hayee BH, Yeoh DP, Rowbotham DS, Saxena V, McNair A. Terminal ileal photography or biopsy to verify total colonoscopy: does the endoscope agree with the microscope? Gastrointest Endosc. 2007; 66:320–325.25. Rex DK, Petrini JL, Baron TH, Chak A, Cohen J, Deal SE, Hoffman B, Jacobson BC, Mergener K, Petersen BT, et al. Quality indicators for colonoscopy. Am J Gastroenterol. 2006; 101:873–885.26. Lee HL, Eun CS, Lee OY, Jeon YC, Han DS, Sohn JH, Yoon BC, Choi HS, Hahm JS, Lee MH, et al. Significance of colonoscope length in cecal insertion time. Gastrointest Endosc. 2009; 69:503–508.27. Lohsiriwat V, Sujarittanakarn S, Akaraviputh T, Lertakyamanee N, Lohsiriwat D, Kachinthorn U. What are the risk factors of colonoscopic perforation? BMC Gastroenterol. 2009; 9:71.28. Kim JH, Jeon EJ, Song JH, Lee SH, Jung JH, Cheung DY, Kim JI, Park SH, Kim JK. Colonoscopic perforation during a diagnostic colonoscopy. Korean J Gastrointest Endosc. 2011; 42:289–292.29. Shida T, Katsuura Y, Teramoto O, Kaiho M, Takano S, Yoshidome H, Miyazaki M. Transparent hood attached to the colonoscope: does it really work for all types of colonoscopes? Surg Endosc. 2008; 22:2654–2658.30. Cheon YK, Jung IS, Cho YD, Kim JO, Lee MS, Shim CS. A comparative study for usefulness of a variable-stiffness colonoscope to a conventional colonoscope. Korean J Gastrointest Endosc. 2002; 25:132–136.31. Westwood DA, Alexakis N, Connor SJ. Transparent cap-assisted colonoscopy versus standard adult colonoscopy: a systematic review and meta-analysis. Dis Colon Rectum. 2012; 55:218–225.32. Kennedy G, Larson D, Wolff B, Winter D, Petersen B, Larson M. Routine ileal intubation during screening colonoscopy: a useful maneuver? Surg Endosc. 2008; 22:2606–2608.33. Jeong SH, Lee KJ, Kim YB, Kwon HC, Sin SJ, Chung JY. Diagnostic value of terminal ileum intubation during colonoscopy. J Gastroenterol Hepatol. 2008; 23:51–55.34. Rey JF, Lambert R. ESGE Quality Assurance Committee. ESGE recommendations for quality control in gastrointestinal endoscopy: guidelines for image documentation in upper and lower GI endoscopy. Endoscopy. 2001; 33:901–903.35. Marshall JB, Brown DN. Photodocumentation of total colonoscopy: how successful are endoscopists? do reviewers agree? Gastrointest Endosc. 1996; 44:243–248.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- A Comparative Study for Usefulness of a Variable-Stiffness Colonoscope to a Conventional Colonoscope
- Efficacy of Hood-cap Assisted Colonoscopy; Comparison with Conventional Colonoscopy
- How Do I Overcome Difficulties in Insertion?
- Efficacy of Transparent Cap-attached Colonoscopy: Does It Improve the Quality of Colonoscopy?
- The Comparison of Suceess Rates of Lightwand Facilitated Tracheal Intubation in Different Head Positions (Neutral Position versus Sniffing Position)