J Korean Med Sci.
2022 Feb;37(5):e32. 10.3346/jkms.2022.37.e32.
Dermatomyositis Following BNT162b2 mRNA COVID-19 Vaccination
- Affiliations
-
- 1Department of Rheumatology, Faculty of Medicine, Al Azhar University, Assiut, Egypt
- 2Department of Rheumatology, Al-Sabah Hospital, Kuwait, Kuwait
- 3Department of Rheumatology, Jaber Al Ahmad Hospital, Kuwait, Kuwait
- 4Asad Al Hamad Dermatology Center, Kuwait, Kuwait
- 5Department of Radiodiagnosis, Al-Sabah Hospital, Kuwait, Kuwait
- 6Department of Endemic and Infectious Diseases, Faculty of Medicine, Suez Canal University, Ismailia, Egypt
- KMID: 2525484
- DOI: http://doi.org/10.3346/jkms.2022.37.e32
Abstract
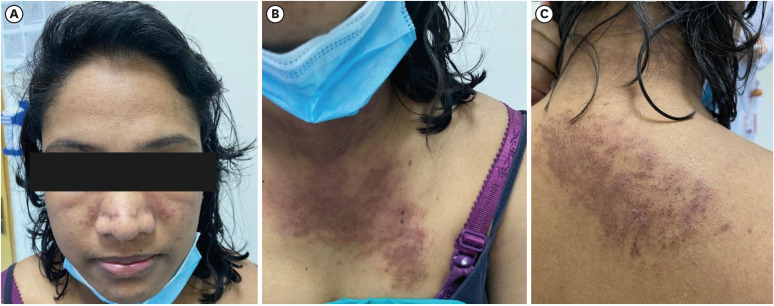
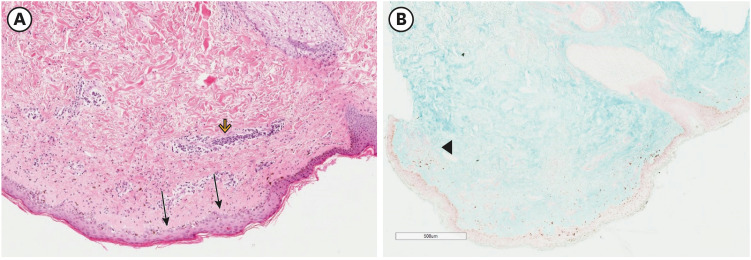
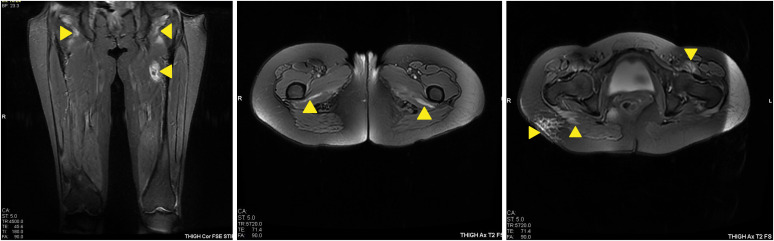
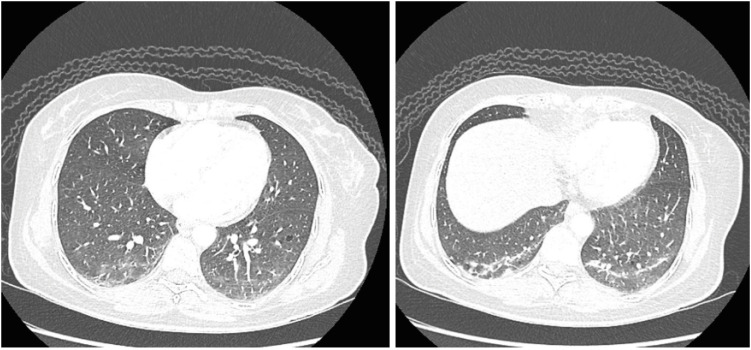
- Dermatomyositis (DM) is one of the uncommon multi-organ idiopathic inflammatory myopathies that has been reported following the hepatitis B, Influenza, tetanus toxoid, H1N1, and BCG vaccines. However, an association with the coronavirus disease 2019 (COVID-19) vaccine is yet to be reported. In this case, we present the case of a 43-year-old Asian Indian female who was diagnosed with DM 10 days after receiving the second dosage of BNT162b2 mRNA COVID-19 vaccination, in the absence of any additional triggering factors. The diagnosis was established based on physical examination, serological antibodies, magnetic resonance imaging of the muscles, skin biopsy, and electromyography. She received standard treatment for DM, including oral high doses of prednisolone, hydroxychloroquine, mycophenolate, and physiotherapy. The treatment successfully reversed skin changes and muscle weakness. This is the first reported case of classic DM complicated by interstitial lung disease following COVID-19 vaccination. More clinical and functional studies are needed to elucidate this association. Clinicians should be aware of this unexpected adverse event following COVID-19 vaccination and arrange for appropriate management.
Keyword
Figure
Reference
-
1. University of Oxford. Statistics and research. Coronavirus (COVID-19) vaccinations. Updated 2021. Accessed March 5 2021. https://ourworldindata.org/covid-vaccinations .2. Vlachoyiannopoulos PG, Magira E, Alexopoulos H, Jahaj E, Theophilopoulou K, Kotanidou A, et al. Autoantibodies related to systemic autoimmune rheumatic diseases in severely ill patients with COVID-19. Ann Rheum Dis. 2020; 79(12):1661–1663. PMID: 32581086.
Article3. Avina-Zubieta JA, Sayre EC, Bernatsky S, Lehman AJ, Shojania K, Esdaile J, et al. Adult prevalence of systemic autoimmune rheumatic diseases (SARDs) in British Columbia, Canada. Arthritis Rheum. 2011; 63(Suppl 10):1846.4. Bohan A, Peter JB. Polymyositis and dermatomyositis (first of two parts). N Engl J Med. 1975; 292(7):344–347. PMID: 1090839.5. Bohan A, Peter JB. Polymyositis and dermatomyositis (second of two parts). N Engl J Med. 1975; 292(8):403–407. PMID: 1089199.6. Lundberg IE, Tjärnlund A, Bottai M, Werth VP, Pilkington C, Visser M, et al. 2017 European League Against Rheumatism/American College of Rheumatology classification criteria for adult and juvenile idiopathic inflammatory myopathies and their major subgroups. Ann Rheum Dis. 2017; 76(12):1955–1964. PMID: 29079590.7. Dimachkie MM, Barohn RJ, Amato AA. Idiopathic inflammatory myopathies. Neurol Clin. 2014; 32(3):595–628. PMID: 25037081.
Article8. Reed AM, Ytterberg SR. Genetic and environmental risk factors for idiopathic inflammatory myopathies. Rheum Dis Clin North Am. 2002; 28(4):891–916. PMID: 12506777.
Article9. Orbach H, Tanay A. Vaccines as a trigger for myopathies. Lupus. 2009; 18(13):1213–1216. PMID: 19880571.
Article10. Shoenfeld Y, Agmon-Levin N. ‘ASIA’ - autoimmune/inflammatory syndrome induced by adjuvants. J Autoimmun. 2011; 36(1):4–8. PMID: 20708902.
Article11. Stübgen JP. A review on the association between inflammatory myopathies and vaccination. Autoimmun Rev. 2014; 13(1):31–39. PMID: 24001753.
Article12. Wadman M. Public needs to prep for vaccine side effects. Science. 2020; 370(6520):1022. PMID: 33243869.
Article13. Ladislau L, Suárez-Calvet X, Toquet S, Landon-Cardinal O, Amelin D, Depp M, et al. JAK inhibitor improves type I interferon induced damage: proof of concept in dermatomyositis. Brain. 2018; 141(6):1609–1621. PMID: 29741608.
Article14. Waheed S, Bayas A, Hindi F, Rizvi Z, Espinosa PS. Neurological complications of COVID-19: Guillain-Barre syndrome following Pfizer COVID-19 vaccine. Cureus. 2021; 13(2):e13426. PMID: 33758714.
Article15. Li M, Yuan J, Lv G, Brown J, Jiang X, Lu ZK. Myocarditis and pericarditis following COVID-19 vaccination: Inequalities in age and vaccine types. J Pers Med. 2021; 11(11):1106. PMID: 34834458.
Article16. Maramattom BV, Philips G, Thomas J, Santhamma SG. Inflammatory myositis after ChAdOx1 vaccination. Lancet Rheumatol. 2021; 3(11):e747–e749. PMID: 34585145.
Article17. Theodorou DJ, Theodorou SJ, Axiotis A, Gianniki M, Tsifetaki N. COVID-19 vaccine-related myositis. QJM. 2021; 114(6):424–425. PMID: 33647971.
Article18. Godoy IRB, Rodrigues TC, Skaf A. Myositis ossificans following COVID-19 vaccination. QJM. 2021; 114(9):659–660. PMID: 34109386.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- New-onset Refractory Status Epilepticus after BNT162b2 mRNA COVID-19 Vaccination
- Adult-onset Still’s Disease after BNT162b2 mRNA COVID-19 Vaccine
- Ipsilateral Radial Neuropathy after COVID-19 mRNA Vaccination in an Immunocompetent Young Man
- BNT162b2 (Pfizer) mRNA Covid-19 Vaccine Induced De Novo Generalized Pustular Psoriasis
- mRNA COVID-19 Vaccine-Associated Subserosal Eosinophilic Gastroenteritis: A Case Report