Clin Endosc.
2021 Jul;54(4):596-602. 10.5946/ce.2020.194.
Outcomes of Endoscopic Ultrasound-Guided Biliary Drainage in Patients Undergoing Antithrombotic Therapy
- Affiliations
-
- 1Department of Gastroenterology, Aichi Cancer Center Hospital, Nagoya, Japan
- 2Department of Endoscopy, Aichi Cancer Center Hospital, Nagoya, Japan
- KMID: 2518864
- DOI: http://doi.org/10.5946/ce.2020.194
Abstract
- Background/Aims
The Japan Gastroenterological Endoscopy Society (JGES) has published guidelines for gastroenterological endoscopy in patients undergoing antithrombotic treatment. These guidelines classify endoscopic ultrasound-guided biliary drainage (EUS-BD) as a high-risk procedure. Nevertheless, the bleeding risk of EUS-BD in patients undergoing antithrombotic therapy is uncertain. Therefore, this study aimed to assess the bleeding risk in patients undergoing antithrombotic therapy.
Methods
This single-center retrospective study included 220 consecutive patients who underwent EUS-BD between January 2013 and December 2018. We managed the withdrawal and continuation of antithrombotic agents according to the JGES guidelines. We compared the bleeding event rates among patients who received and those who did not receive antithrombotic agents.
Results
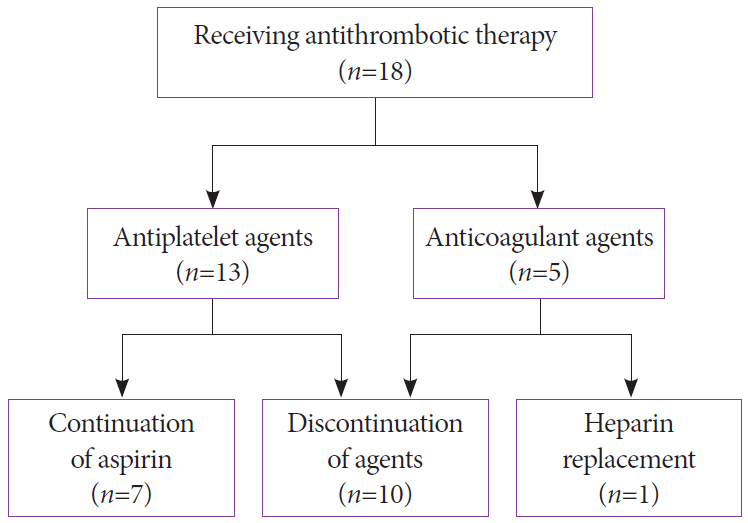
A total of 18 patients (8.1%) received antithrombotic agents and 202 patients (91.8%) did not. Three patients experienced bleeding events, with an overall bleeding event rate of 1.3% (3/220): one patient was in the antithrombotic group (5.5%) and two patients were in the non-antithrombotic group (0.9%) (p=0.10). All cases were moderate. The sole thromboembolic event (0.4%) was a cerebral infarction in a patient in the non-antithrombotic group.
Conclusions
The rate of EUS-BD-related bleeding events was low. Even in patients receiving antithrombotic therapy, the bleeding event rates were not significantly different from those in patients not receiving antithrombotic therapy.
Keyword
Figure
Reference
-
1. Veitch AM, Baglin TP, Gershlick AH, Harnden SM, Tighe R, Cairns S. Guidelines for the management of anticoagulant and antiplatelet therapy in patients undergoing endoscopic procedures. Gut. 2008; 57:1322–1329.
Article2. ASGE Standards of Practice Committee, Anderson MA, Ben-Menachem T, et al. Management of antithrombotic agents for endoscopic procedures. Gastrointest Endosc. 2009; 70:1060–1070.
Article3. Boustière C, Veitch A, Vanbiervliet G, et al. Endoscopy and antiplatelet agents. European Society of Gastrointestinal Endoscopy (ESGE) guideline. Endoscopy. 2011; 43:445–461.
Article4. Fujimoto K, Fujishiro M, Kato M, et al. Guidelines for gastroenterological endoscopy in patients undergoing antithrombotic treatment. Dig Endosc. 2014; 26:1–14.
Article5. Kien-Fong Vu C, Chang F, Doig L, Meenan J. A prospective control study of the safety and cellular yield of EUS-guided FNA or Trucut biopsy in patients taking aspirin, nonsteroidal anti-inflammatory drugs, or prophylactic low molecular weight heparin. Gastrointest Endosc. 2006; 63:808–813.
Article6. Inoue T, Okumura F, Sano H, et al. Bleeding risk of endoscopic ultrasound-guided fine-needle aspiration in patients undergoing antithrombotic therapy. Dig Endosc. 2017; 29:91–96.
Article7. Kawakubo K, Yane K, Eto K, et al. A prospective multicenter study evaluating bleeding risk after endoscopic ultrasound-guided fine needle aspiration in patients prescribed antithrombotic agents. Gut Liver. 2018; 12:353–359.
Article8. Polmanee P, Hara K, Mizuno N, et al. Outcomes of EUS-FNA in patients receiving antithrombotic therapy. Endosc Int Open. 2019; 7:E15–E25.
Article9. Okuno N, Hara K, Mizuno N, et al. Risks of transesophageal endoscopic ultrasonography-guided biliary drainage. International Journal of Gastrointestinal Intervention. 2017; 6:82–84.
Article10. Cotton PB, Eisen GM, Aabakken L, et al. A lexicon for endoscopic adverse events: report of an ASGE workshop. Gastrointest Endosc. 2010; 71:446–454.
Article11. Baron TH, Kamath PS, McBane RD. Antithrombotic therapy and invasive procedures. N Engl J Med. 2013; 369:1079–1080.
Article12. Douketis JD, Spyropoulos AC, Kaatz S, et al. Perioperative bridging anticoagulation in patients with atrial fibrillation. N Engl J Med. 2015; 373:823–833.
Article13. Li HK, Chen FC, Rea RF, et al. No increased bleeding events with continuation of oral anticoagulation therapy for patients undergoing cardiac device procedure. Pacing Clin Electrophysiol. 2011; 34:868–874.
Article14. Kato M, Uedo N, Hokimoto S, et al. Guidelines for gastroenterological endoscopy in patients undergoing antithrombotic treatment: 2017 appendix on anticoagulants including direct oral anticoagulants. Dig Endosc. 2018; 30:433–440.15. Ikarashi S, Katanuma A, Kin T, et al. Factors associated with delayed hemorrhage after endoscopic sphincterotomy: Japanese large single-center experience. J Gastroenterol. 2017; 52:1258–1265.
Article16. Hamada T, Yasunaga H, Nakai Y, et al. Bleeding after endoscopic sphincterotomy or papillary balloon dilation among users of antithrombotic agents. Endoscopy. 2015; 47:997–1004.
Article17. Isayama H, Nakai Y, Itoi T, et al. Clinical practice guidelines for safe performance of endoscopic ultrasound/ultrasonography-guided biliary drainage: 2018. J Hepatobiliary Pancreat Sci. 2019; 26:249–269.
Article18. Okuno N, Hara K, Mizuno N, et al. Efficacy of the 6-mm fully covered self-expandable metal stent during endoscopic ultrasound-guided hepaticogastrostomy as a primary biliary drainage for the cases estimated difficult endoscopic retrograde cholangiopancreatography: a prospective clinical study. J Gastroenterol Hepatol. 2018; 33:1413–1421.19. Matsumoto S, Hara K, Mizuno N, et al. Risk factor analysis for adverse events and stent dysfunction of endoscopic ultrasound-guided choledochoduodenostomy. Dig Endosc. 2020; 32:957–966.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Recent development of endoscopic ultrasound-guided biliary drainage
- Endoscopic ultrasound-guided biliary drainage in malignant distal biliary obstruction
- Endoscopic ultrasound-guided biliary drainage in malignant hilar obstruction
- Advances in Endoscopic Ultrasound-Guided Biliary Drainage: A Comprehensive Review
- Endoscopic Ultrasound-Guided Hepaticogastrostomy: Technical Review and Tips to Prevent Adverse Events