Clin Endosc.
2021 May;54(3):432-435. 10.5946/ce.2020.146.
Gastric Angiolipoma Resected with Endoscopic Submucosal Dissection
- Affiliations
-
- 1Division of Gastroenterology, Department of Internal Medicine, Daegu Fatima Hospital, Daegu, Korea
- KMID: 2516325
- DOI: http://doi.org/10.5946/ce.2020.146
Abstract
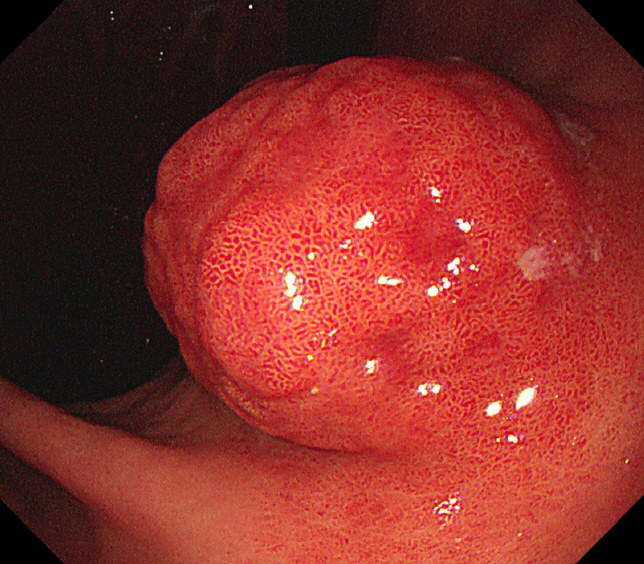
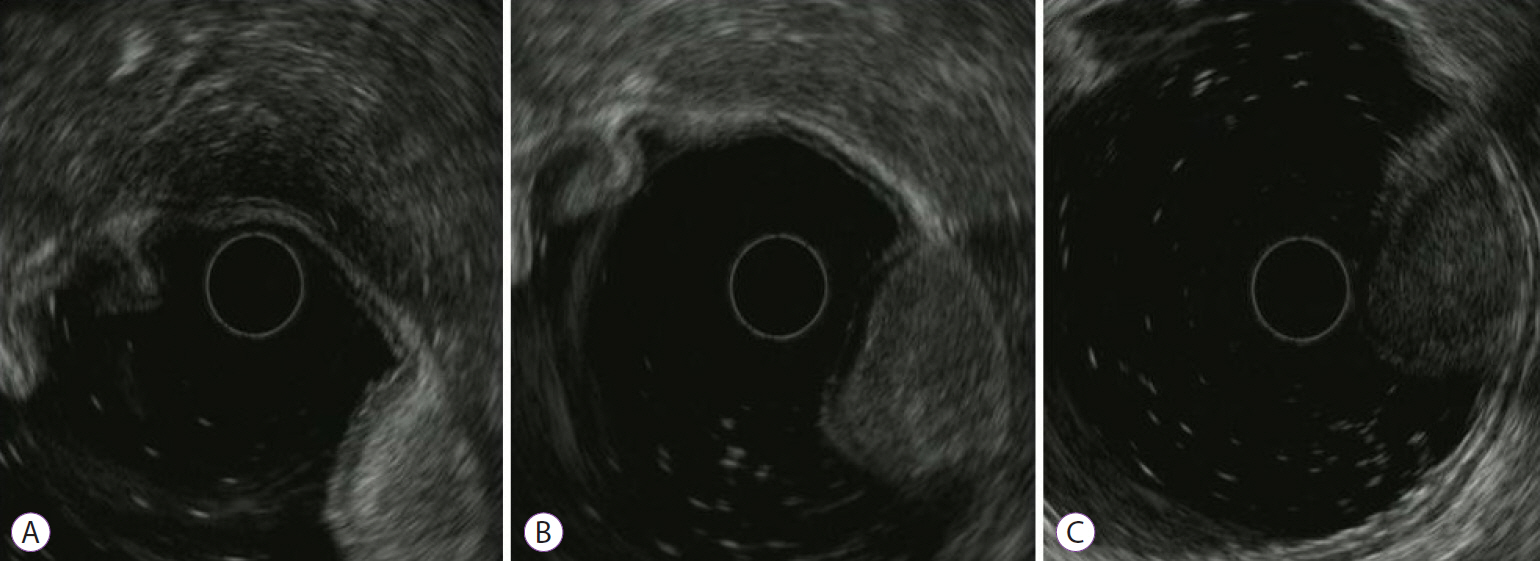
- Angiolipoma is a benign fatty neoplasm that has components of proliferating blood vessels. These types of lesions commonly occur in the subcutaneous tissue of the limbs and trunk. Angiolipoma in the gastrointestinal tract is extremely rare, and the final diagnosis generally depends on histological examination of the excised biopsy. In most previously reported cases, the lesions were diagnosed and treated with surgical management. In this study, we report a case of gastric angiolipoma of approximately 4 cm in size that was diagnosed and treated with endoscopic submucosal dissection.
Figure
Reference
-
1. Lin JJ, Lin F. Two entities in angiolipoma. A study of 459 cases of lipoma with review of literature on infiltrating angiolipoma. Cancer. 1974; 34:720–727.2. Kacar S, Kuran S, Temucin T, Odemis B, Karadeniz N, Sasmaz N. Rectal angiolipoma: a case report and review of literature. World J Gastroenterol. 2007; 13:1460–1465.
Article3. Lou XH, Chen WG, Ning LG, Chen HT, Xu GQ. Multiple gastric angiolipomas: a case report. World J Clin Cases. 2019; 7:778–784.
Article4. Jensen EH, Klapman JB, Kelley ST. Angiolipoma of the esophagus: a rare clinical dilemma. Dis Esophagus. 2006; 19:203–207.
Article5. Dixon AY, McGregor DH, Lee SH. Angiolipomas: an ultrastructural and clinicopathological study. Hum Pathol. 1981; 12:739–747.
Article6. Okuyama T, Yoshida M, Watanabe M, Kinoshita Y, Harada Y. Angiolipoma of the colon diagnosed after endoscopic resection. Gastrointest Endosc. 2002; 55:748–750.
Article7. Howard WR, Helwig EB. Angiolipoma. Arch Dermatol. 1960; 82:924–931.
Article8. DeRidder PH, Levine AJ, Katta JJ, Catto JA. Angiolipoma of the stomach as a cause of chronic upper gastrointestinal bleeding. Surg Endosc. 1989; 3:106–108.
Article9. Nam YH, Park SC, Kim HJ, et al. Angiolipoma of the stomach presenting with anaemia. Prz Gastroenterol. 2014; 9:371–374.
Article10. McGregor DH, Kerley SW, McGregor MS. Case report: gastric angiolipoma with chronic hemorrhage and severe anemia. Am J Med Sci. 1993; 305:229–235.
Article11. Hunt J, Tindal D. Solitary gastric Peutz-Jeghers polyp and angiolipoma presenting as acute haemorrhage. Aust N Z J Surg. 1996; 66:713–715.
Article12. Jung IS, Jang JY, Ryu CB, et al. Angiolipoma of the duodenum diagnosed after endoscopic resection. Endoscopy. 2004; 36:375.
Article13. Chen YY, Soon MS. Preoperative diagnosis of colonic angiolipoma: a case report. World J Gastroenterol. 2005; 11:5087–5089.
Article14. Tang X, Tan Y, Liu D. Angiolipoma: a rare esophageal submucosal tumor. Gastrointest Endosc. 2017; 86:399–400.
Article15. Ferrozzi F, Tognini G, Bova D, Pavone P. Lipomatous tumors of the stomach: CT findings and differential diagnosis. J Comput Assist Tomogr. 2000; 24:854–858.
Article16. Pih GY, Kim DH. Endoscopic ultrasound-guided fine needle aspiration and biopsy in gastrointestinal subepithelial tumors. Clin Endosc. 2019; 52:314–320.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- The Histologic Discrepancy before and after Endoscopic Submucosal Dissection of Gastric Adenoma and Early Gastric Cancer
- Pathology of Endoscopic Submucosal Dissection; How Do We Interpret?
- Pathological Interpretation of Gastric Tumors in Endoscopic Submucosal Dissection
- The Clinical Accuracy of Endoscopic Ultrasonography and White Light Imaging in Gastric Endoscopic Submucosal Dissection
- Perforation of a Gastric Tear during Esophageal Endoscopic Submucosal Dissection under General Anesthesia