Ann Surg Treat Res.
2020 Jan;98(1):51-55. 10.4174/astr.2020.98.1.51.
Retrospective study on prevalence of recurrent inguinal hernia: a large-scale multi-institutional study
- Affiliations
-
- 1Department of Surgery, Seoul St. Mary's Hospital, College of Medicine, The Catholic University of Korea, Seoul, Korea.
- 2Department of Surgery, Incheon St. Mary's Hospital, College of Medicine, The Catholic University of Korea, Incheon, Korea.
- 3Department of Surgery, Daejeon St. Mary's Hospital, College of Medicine, The Catholic University of Korea, Daejeon, Korea.
- 4Department of Surgery, Uijeongbu St. Mary's Hospital, College of Medicine, The Catholic University of Korea, Uijeongbu, Korea.
- 5Department of Surgery, Eunpyeong St. Mary's Hospital, College of Medicine, The Catholic University of Korea, Seoul, Korea. hj@catholic.ac.kr
- KMID: 2466563
- DOI: http://doi.org/10.4174/astr.2020.98.1.51
Abstract
- PURPOSE
We conducted a multi-institutional analysis to establish the epidemiological characteristics of recurrent inguinal hernia following hernia repair in patients across 4 institutions in Korea.
METHODS
The retrospectively reviewed data included patient characteristics, hernia location, year of primary operation, type of hernia, timing of recurrence, primary operation type, and whether a mesh was used.
RESULTS
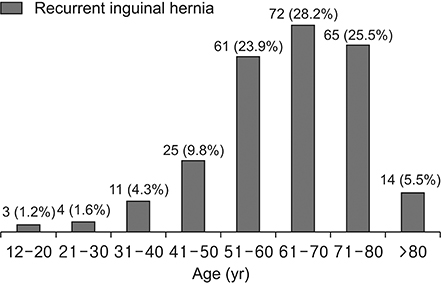
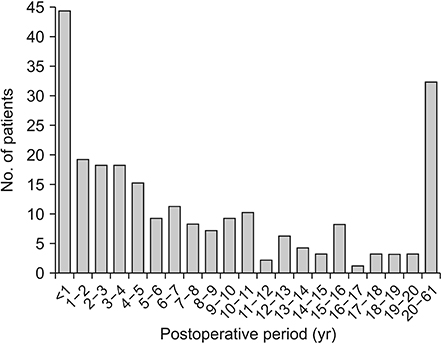
Among 4,604 patients who underwent hernia repair surgery, 255 patients (5.5%; 13 females and 242 males; mean age, 63 years) were found to have recurrent hernia from January 2010 to April 2017. Recurrent indirect inguinal and direct hernias were observed in 47.1% and 49.4% of the patients, respectively. The recurrence of hernias within 1 year of surgery was the highest at 17.25%. Early and late recurrences was observed in 23.5% and 66.5% of the patients, respectively. Among the patients, 81.6% underwent open hernia repair at the time of initial surgery.
CONCLUSION
Recurrence of hernia is most common in the first year after the initial surgery, and 23.5% of recurrent inguinal hernia was developed within 2 years. Patients underwent surgery after an average of 116 months (median value, 64 months) following the first operation. In patients with recurrent hernia, direct hernia was seen more frequent than indirect hernia whereas indirect hernia occurred more in patients with primary hernia.
Keyword
MeSH Terms
Figure
Reference
-
1. EU Hernia Trialists Collaboration. Repair of groin hernia with synthetic mesh: meta-analysis of randomized controlled trials. Ann Surg. 2002; 235:322–332.2. Bendavid R. Inguinal herniorrhaphy in women. Hernia. 2006; 10:103–104.
Article3. EU Hernia Trialists Collaboration. Mesh compared with non-mesh methods of open groin hernia repair: systematic review of randomized controlled trials. Br J Surg. 2000; 87:854–859.4. Scott NW, McCormack K, Graham P, Go PM, Ross SJ, Grant AM. Open mesh versus non-mesh for repair of femoral and inguinal hernia. Cochrane Database Syst Rev. 2002; (4):CD002197.5. Dahlstrand U, Wollert S, Nordin P, Sandblom G, Gunnarsson U. Emergency femoral hernia repair: a study based on a national register. Ann Surg. 2009; 249:672–676.6. Magnusson N, Nordin P, Hedberg M, Gunnarsson U, Sandblom G. The time profile of groin hernia recurrences. Hernia. 2010; 14:341–344.
Article7. Bay-Nielsen M, Nordin P, Nilsson E, Kehlet H;. Operative findings in recurrent hernia after a Lichtenstein procedure. Am J Surg. 2001; 182:134–136.
Article8. Sondenaa K, Nesvik I, Breivik K, Korner H. Long-term follow-up of 1059 consecutive primary and recurrent inguinal hernias in a teaching hospital. Eur J Surg. 2001; 167:125–129.9. Matthews RD, Anthony T, Kim LT, Wang J, Fitzgibbons RJ Jr, Giobbie-Hurder A, et al. Factors associated with postoperative complications and hernia recurrence for patients undergoing inguinal hernia repair: a report from the VA Cooperative Hernia Study Group. Am J Surg. 2007; 194:611–617.
Article10. Heller CA, Marucci DD, Dunn T, Barr EM, Houang M, Dos Remedios C. Inguinal canal “lipoma”. Clin Anat. 2002; 15:280–285.
Article11. Eklund AS, Montgomery AK, Rasmussen IC, Sandbue RP, Bergkvist LA, Rudberg CR. Low recurrence rate after laparoscopic (TEP) and open (Lichtenstein) inguinal hernia repair: a randomized, multicenter trial with 5-year follow-up. Ann Surg. 2009; 249:33–38.12. Han SR, Kim HJ, Kim NH, Shin S, Yoo RN, Kim G, et al. Inguinal hernia surgery in Korea. Ann Surg Treat Res. 2019; 97:41–47.13. Jansen PL, Klinge U, Jansen M, Junge K. Risk factors for early recurrence after inguinal hernia repair. BMC Surg. 2009; 9:18.
Article14. Burcharth J, Pommergaard HC, Bisgaard T, Rosenberg J. Patient-related risk factors for recurrence after inguinal hernia repair: a systematic review and meta-analysis of observational studies. Surg Innov. 2015; 22:303–317.15. Phillips EH, Rosenthal R, Fallas M, Carroll B, Arregui M, Corbitt J, et al. Reasons for early recurrence following laparoscopic hernioplasty. Surg Endosc. 1995; 9:140–144.
Article16. Lowham AS, Filipi CJ, Fitzgibbons RJ Jr, Stoppa R, Wantz GE, Felix EL, et al. Mechanisms of hernia recurrence after preperitoneal mesh repair. Traditional and laparoscopic. Ann Surg. 1997; 225:422–431.17. HerniaSurge Group. International guidelines for groin hernia management. Hernia. 2018; 22:1–165.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Clinical Analysis of Recurrent Inguinal Hernias
- An Adult Right-sided Bochdalek Hernia Accompanied with Hepatic Hypoplasia and Inguinal Hernia
- Clinical Characteristics of Inguinal Hernia in Children on Peritoneal Dialysis
- Clinical usefulness of laparoscopic total extraperitoneal hernia repair for recurrent inguinal hernia
- Amyand's Hernia with Periappendicular Abscess