J Korean Foot Ankle Soc.
2019 Sep;23(3):110-115. 10.14193/jkfas.2019.23.3.110.
Result of Staged Operation in Ruedi-Allgower Type II and III Open Tibia Pilon Fractures with Severe Comminution
- Affiliations
-
- 1Department of Orthopaedic Surgery, College of Medicine, Chosun University, Gwangju, Korea. leejy88@chosun.ac.kr
- KMID: 2458012
- DOI: http://doi.org/10.14193/jkfas.2019.23.3.110
Abstract
- PURPOSE
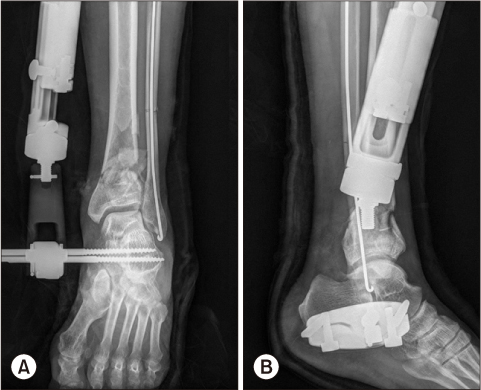
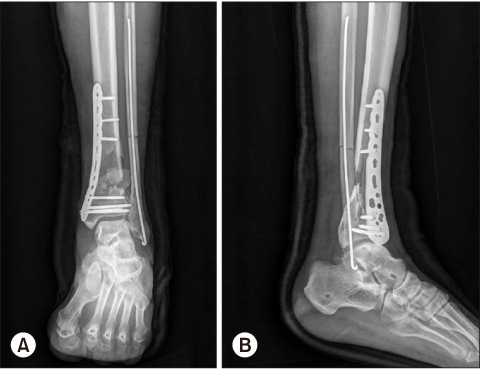
This study analyzed the clinical and radiological results of Reudi-Allgower type II and III open tibia pilon fracture patients who underwent plate fixation after the recovery of a soft tissue injury after external fixation.
MATERIALS AND METHODS
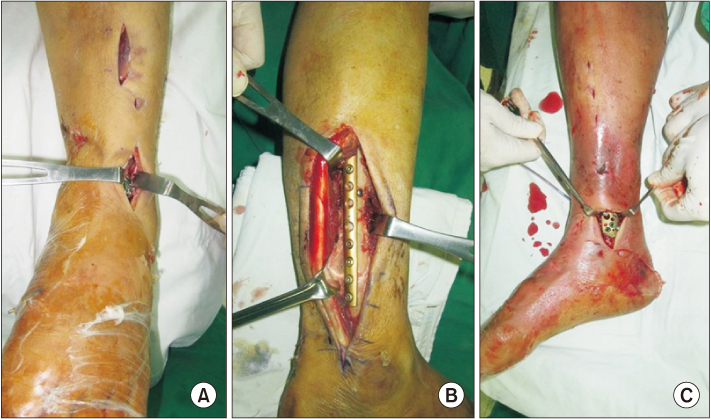
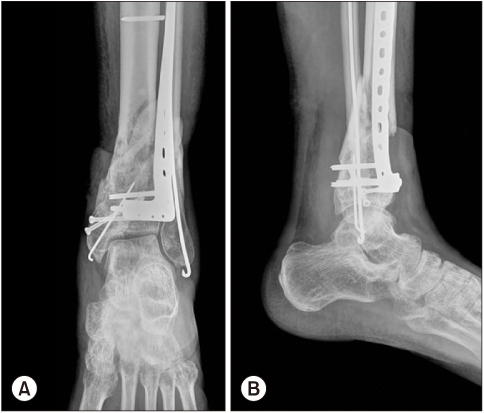
From 2010 to 2015, this study analyzed 14 patients who were treated for open tibial pilon fractures and could be followed up at least one year. The mean age was 49 years and the average follow-up period was 19 months. An emergency operation was performed for external fixation and open wounds, and secondary surgery was performed for definitive fixation using a plate. The radiological and clinical evaluations were analyzed retrospectively. Complications, such as post-traumatic osteoarthritis and wound infections were also analyzed.
RESULTS
The mean duration between two-staged surgery was 21 days and the mean bone union time was 9.2 months. Three cases of delayed union and one case of nonunion were reported. The malunion did not occur in all cases. The average American Orthopaedic Foot and Ankle Society (AOFAS) score was 68 points. A limitation of the ankle motion occurred in all cases. In four cases, wound infections due to initial open wounds occurred; one patient underwent a below the knee amputation due to chronic osteomyelitis. Post-traumatic arthritis occurred in 10 cases.
CONCLUSION
Severe comminuted tibial plateau open fractures of Reudi-Allgower type II and III, which are high-energy injuries that result in extensive soft tissue damage, have a higher incidence of complications, such as ulcer problems and osteomyelitis, than closed tibia plateau fractures. Post-traumatic arthritis is the most common complication of tibia plateau open fractures, and staged surgery is recommended because of the relatively satisfactory clinical results.
Keyword
MeSH Terms
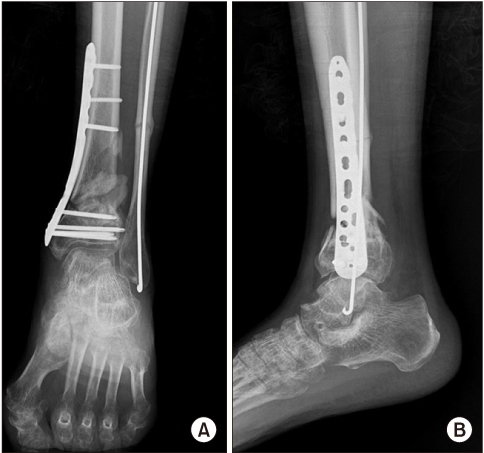
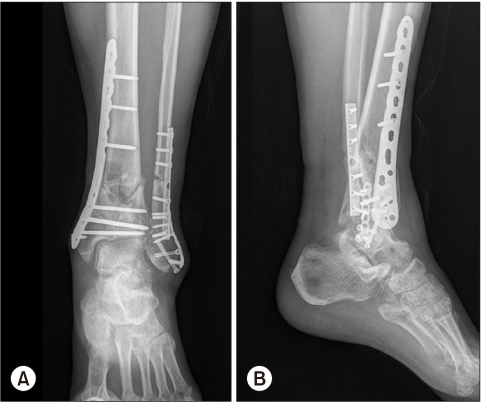
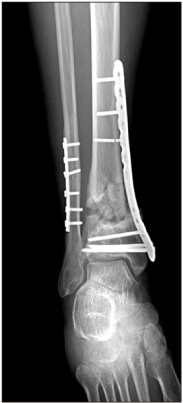
Figure
Reference
-
1. Abelseth G, Buckley RE, Pineo GE, Hull R, Rose MS. Incidence of deep-vein thrombosis in patients with fractures of the lower extremity distal to the hip. J Orthop Trauma. 1996; 10:230–235.
Article2. Barbieri R, Schenk R, Koval K, Aurori K, Aurori B. Hybrid external fixation in the treatment of tibial plafond fractures. Clin Orthop Relat Res. 1996; (332):16–22. DOI: 10.1097/00003086-199611000-00004.
Article3. Blauth M, Bastian L, Krettek C, Knop C, Evans S. Surgical options for the treatment of severe tibial pilon fractures: a study of three techniques. J Orthop Trauma. 2001; 15:153–160.
Article4. Rüedi TP, Allgöwer M. The operative treatment of intra-articular fractures of the lower end of the tibia. Clin Orthop Relat Res. 1979; (138):105–110.
Article5. Gustilo RB, Anderson JT. Prevention of infection in the treatment of one thousand and twenty-five open fractures of long bones: retrospective and prospective analyses. J Bone Joint Surg Am. 1976; 58:453–458.
Article6. Milner SA. A more accurate method of measurement of angulation after fractures of the tibia. J Bone Joint Surg Br. 1997; 79:972–974.
Article7. Mast JW, Spiegel PG, Pappas JN. Fractures of the tibial pilon. Clin Orthop Relat Res. 1988; (230):68–82.
Article8. McNamara MG, Heckman JD, Corley FG. Severe open fractures of the lower extremity: a retrospective evaluation of the Mangled Extremity Severity Score (MESS). J Orthop Trauma. 1994; 8:81–87.9. Rommens PM, Claes P, De Boodt P, Stappaerts KH, Broos PL. [Therapeutic procedure and long-term results in tibial pilon fracture in relation to primary soft tissue damage]. Unfallchirurg. 1994; 97:39–46. German.10. Howard JL, Agel J, Barei DP, Benirschke SK, Nork SE. A prospective study evaluating incision placement and wound healing for tibial plafond fractures. J Orthop Trauma. 2008; 22:299–305. discussion 305–6. DOI: 10.1097/BOT.0b013e318172c811.
Article11. Babis GC, Vayanos ED, Papaioannou N, Pantazopoulos T. Results of surgical treatment of tibial plafond fractures. Clin Orthop Relat Res. 1997; (341):99–105.
Article12. Bourne RB, Rorabeck CH, Macnab J. Intra-articular fractures of the distal tibia: the pilon fracture. J Trauma. 1983; 23:591–596. DOI: 10.1097/00005373-198307000-00008.13. Conroy J, Agarwal M, Giannoudis PV, Matthews SJ. Early internal fixation and soft tissue cover of severe open tibial pilon fractures. Int Orthop. 2003; 27:343–347. DOI: 10.1007/s00264-003-0486-1.
Article14. Danoff JR, Saifi C, Goodspeed DC, Reid JS. Outcome of 28 open pilon fractures with injury severity-based fixation. Eur J Orthop Surg Traumatol. 2015; 25:569–575. DOI: 10.1007/s00590-014-1552-7.
Article15. Ketz J, Sanders R. Staged posterior tibial plating for the treatment of Orthopaedic Trauma Association 43C2 and 43C3 tibial pilon fractures. J Orthop Trauma. 2012; 26:341–347. DOI: 10.1097/BOT.0b013e318225881a.
Article16. Ma CH, Yu SW, Tu YK, Yen CY, Yeh JJ, Wu CH. Staged external and internal locked plating for open distal tibial fractures. Acta Orthop. 2010; 81:382–386. DOI: 10.3109/17453674.2010.487244.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Clinical Evaluation for the Tibial Pilon Fractures
- Treatment of Tibial Pilon Fracture Applied by Biologic Principle
- Treatment of Articular Fracture of the Distal Tibia (Pilon Fracture) with Limited Open Reduction and External Fixator
- A Clinical Analysis of the Tibial Pilon Fractures with Open Reduction
- A Clinical Study of tibial Pilon Fractures