J Korean Foot Ankle Soc.
2017 Mar;21(1):27-32. 10.14193/jkfas.2017.21.1.27.
Tricortical-allobone Grafting in Screw Fixation for Intra-articular Calcaneal Fracture via Ollier Approach
- Affiliations
-
- 1Department of Orthopedic Surgery, Sanggye Paik Hospital, Inje University School of Medicine, Seoul, Korea. youngos@paik.ac.kr
- 2Department of Orthopedic Surgery, Pusan National University Yangsan Hospital, Pusan National University School of Medicine, Yangsan, Korea.
- KMID: 2371971
- DOI: http://doi.org/10.14193/jkfas.2017.21.1.27
Abstract
- PURPOSE
Bone grafting is often necessary to maintain a reduction and prevent delayed collapse of reduced fracture in a treatment of severely displaced comminuted intra-articular calcaneal fractures. Herein, we analyzed the usefulness and necessary conditions to perform tricortical-allobone grafting in open reduction of calcaneal fracture via the Ollier approach.
MATERIALS AND METHODS
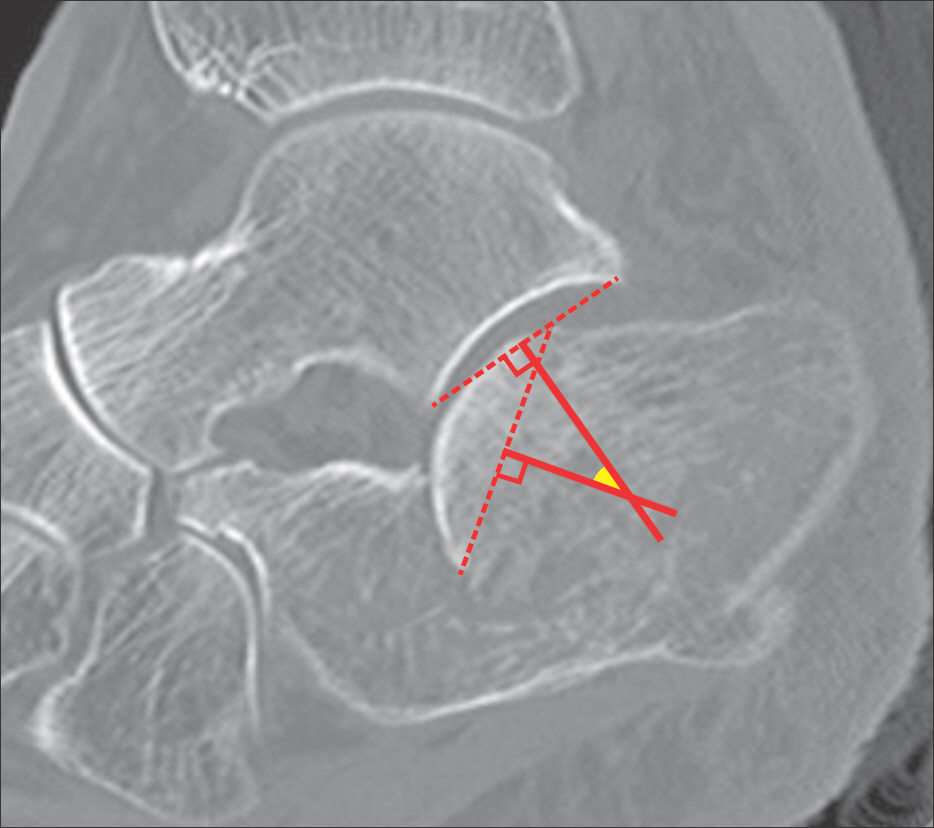
We performed a retrospective review of 57 intra-articular calcaneal fractures that underwent an operation via the Ollier approach between April 2009 and April 2015. They were divided into two groups: Group 1 (n=17) included those with tricortical-allobone grafts underneath the posterior facet fragment, and group 2 (n=40) included cases without a bone graft. We measured the Böhler angle, Gissane angle, height, and width of the calcaneus at preoperative, postoperative, and final follow-up radiograph. We measured the sagittal rotational angle of the posterior facet fragment of preoperative computed tomography to analyze the effect and necessary conditions for bone grafting. We also reviewed the clinical results by the American Orthopaedic Foot and Ankle Society (AOFAS) scale, visual analogue scale (VAS), and any complications.
RESULTS
According to the Sanders classification, there were 3 type-II fractures, 12 type-III fractures, and 2 type-IV fractures in Group 1; whereas in Group 2, there were 26 type-II fractures, 13 type-III fractures, and 1 type-IV fracture (p=0.002). Regarding the preoperative radiologic parameters, there were significant differences in the Böhler angle (p=0.006), Gissane angle (p=0.043), and rotational angle of the posterior facet fragment (p=0.001). No significant difference was observed in the preoperative calcaneal height and width, as well as postoperative radiologic parameters. There was no significant clinical difference between the two groups (p=0.546).
CONCLUSION
We suggest that a tricortical-allobone graft may be useful in open reduction and screw fixation via the Ollier approach for displaced intra-articular calcaneal fracture with a bony defect after reduction of collapsed posterior facet fragment. This graft can contribute to the stable reduction via a small approach, even without a plate.
MeSH Terms
Figure
Reference
-
1.Choi JC., Lee KS., Kim BS., Park BY., Cha JH. Open reduction and internal fixation of intraarticular calcaneal fractures by the extended lateral approach. J Korean Orthop Assoc. 1997. 32:370–5.
Article2.Jiang SD., Jiang LS., Dai LY. Surgical treatment of calcaneal fractures with use of beta-tricalcium phosphate ceramic grafting. Foot Ankle Int. 2008. 29:1015–9.3.Goulet JA., Senunas LE., DeSilva GL., Greenfield ML. Autogenous iliac crest bone graft. Complications and functional assessment. Clin Orthop Relat Res. 1997. 339:76–81.
Article4.Xia S., Lu Y., Wang H., Wu Z., Wang Z. Open reduction and internal fixation with conventional plate via L-shaped lateral approach versus internal fixation with percutaneous plate via a sinus tarsi approach for calcaneal fractures: a randomized controlled trial. Int J Surg. 2014. 12:475–80.5.Bae SY., Shin YK., Kim JO., Lee JH., Lee CW., Shin JH. Evaluation of rotational displacement of the posterior facet on the sagittal plane in computed tomographic images of calcaneal fractures. J Korean Fract Soc. 2005. 18:165–9.
Article6.Kim KW., Cho SG., Lee DY. Treatment of displaced intra-articular calcaneal fracture using ollier approach. J Korean Foot Ankle Soc. 2008. 12:174–9.7.Loucks C., Buckley R. Bohler’s angle: correlation with outcome in displaced intra-articular calcaneal fractures. J Orthop Trauma. 1999. 13:554–8.
Article8.Leung KS., Chan WS., Shen WY., Pak PP., So WS., Leung PC. Operative treatment of intraarticular fractures of the os calcis--the role of rigid internal fixation and primary bone grafting: preliminary results. J Orthop Trauma. 1989. 3:232–40.9.Leung KS., Yuen KM., Chan WS. Operative treatment of displaced intra-articular fractures of the calcaneum. Medium-term results. J Bone Joint Surg Br. 1993. 75:196–201.
Article10.Huang PJ., Huang HT., Chen TB., Chen JC., Lin YK., Cheng YM, et al. Open reduction and internal fixation of displaced intra-articular fractures of the calcaneus. J Trauma. 2002. 52:946–50.
Article111.Thornes BS., Collins AL., Timlin M., Corrigan J. Outcome of cal-caneal fractures treated operatively and non-operatively. the effect of litigation on outcomes. Ir J Med Sci. 2002. 171:155–7.
Article12.Sanders R., Fortin P., DiPasquale T., Walling A. Operative treatment in 120 displaced intraarticular calcaneal fractures. Results using a prognostic computed tomography scan classification. Clin Orthop Relat Res. 1993. 290:87–95.13.Stephenson JR. Treatment of displaced intra-articular fractures of the calcaneus using medial and lateral approaches, internal fixation, and early motion. J Bone Joint Surg Am. 1987. 69:115–30.
Article14.Letournel E. Open treatment of acute calcaneal fractures. Clin Orthop Relat Res. 1993. 290:60–7.
Article15.Sanders R. Displaced intra-articular fractures of the calcaneus. J Bone Joint Surg Am. 2000. 82:225–50.
Article16.Schnee CL., Freese A., Weil RJ., Marcotte PJ. Analysis of harvest morbidity and radiographic outcome using autograft for anterior cervical fusion. Spine (Phila Pa 1976). 1997. 22:2222–7.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Treatment of Displaced Intra-articular Calcaneal Fracture using Ollier Approach
- Operative Treatment of Intra-articular Calcaneal Fractures by Posterior Approaeh
- Operative Treatment of Calcaneal Fracture
- Management of Displaced Intra-articular Calcaneal Fracture
- The Effect of External Distractor on Recovery of B hler angle in Displaced Intraarticular Calcaneal Fractures