Korean J Hematol.
2012 Mar;47(1):74-76. 10.5045/kjh.2012.47.1.74.
Asymptomatic pneumatosis intestinalis following chemotherapy for B lymphoblastic leukemia with recurrent genetic abnormalities in an adolescent patient
- Affiliations
-
- 1Department of Internal Medicine, CHA Bundang Medical Center, CHA University, Seongnam, Korea.
- 2Division of Hemato-Oncology, Department of Internal Medicine, CHA Bundang Medical Center, CHA University, Seongnam, Korea. sychong@cha.ac.kr
- KMID: 2251974
- DOI: http://doi.org/10.5045/kjh.2012.47.1.74
Abstract
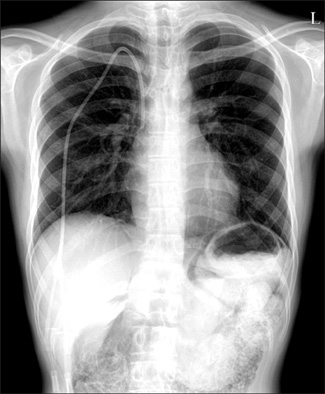
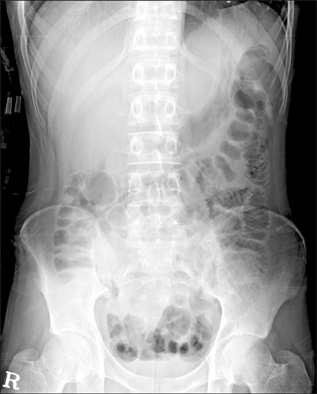
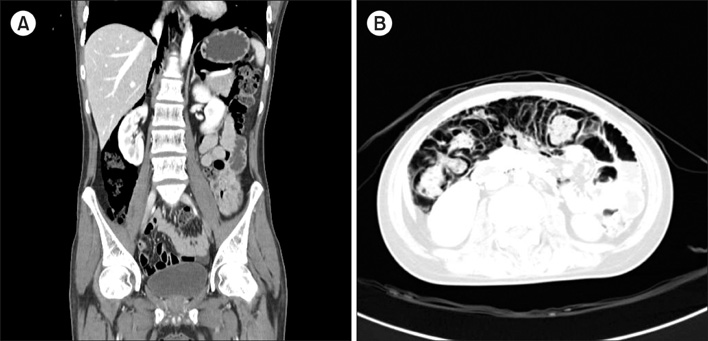
- Pneumatosis intestinalis (PI) is a rare condition characterized by multiple pneumocysts in the submucosa or subserosa of the bowel. Here, we report a rare case of asymptomatic PI after chemotherapy induction in an 18-yr-old man with B lymphoblastic leukemia with recurrent genetic abnormalities. The patient was treated conservatively and recovered without complications. The possibility of PI should be considered as a complication during or after chemotherapy for hematologic malignancies. Conservative treatment should be considered unless there are complications, including peritonitis, bowel perforation, and severe sepsis.
Keyword
MeSH Terms
Figure
Reference
-
1. St Peter SD, Abbas MA, Kelly KA. The spectrum of pneumatosis intestinalis. Arch Surg. 2003. 138:68–75.
Article2. Hashimoto S, Saitoh H, Wada K, et al. Pneumatosis cystoides intestinalis after chemotherapy for hematological malignancies: report of 4 cases. Intern Med. 1995. 34:212–215.
Article3. Candelaria M, Bourlon-Cuellar R, Zubieta JL, Noel-Ettiene LM, Sanchez-Sanchez JM. Gastrointestinal pneumatosis after docetaxel chemotherapy. J Clin Gastroenterol. 2002. 34:444–445.
Article4. Shih IL, Lu YS, Wang HP, Liu KL. Pneumatosis coli after etoposide chemotherapy for breast cancer. J Clin Oncol. 2007. 25:1623–1625.
Article5. Kung D, Ruan DT, Chan RK, Ericsson ML, Saund MS. Pneumatosis intestinalis and portal venous gas without bowel ischemia in a patient treated with irinotecan and cisplatin. Dig Dis Sci. 2008. 53:217–219.
Article6. Lee WI, Jang JJ, Hong SI, et al. Pneumatosis cystoides intestinalis with intestinal volvulus. J Korean Surg Soc. 2009. 76:321–325.
Article7. Heng Y, Schuffler MD, Haggitt RC, Rohrmann CA. Pneumatosis intestinalis: a review. Am J Gastroenterol. 1995. 90:1747–1758.8. Bae SH, Hwang JY, Kim DK, et al. A case of pneumatosis intestinalis in refractory acute precursor B-cell lymphoblastic leukemia-lymphoma. Korean J Med. 2011. 80:482–485.9. Caudill JL, Rose BS. The role of computed tomography in the evaluation of pneumatosis intestinalis. J Clin Gastroenterol. 1987. 9:223–226.
Article10. Connor R, Jones B, Fishman EK, Siegelman SS. Pneumatosis intestinalis: role of computed tomography in diagnosis and management. J Comput Assist Tomogr. 1984. 8:269–275.11. Federle MP, Chun G, Jeffrey RB, Rayor R. Computed tomographic findings in bowel infarction. AJR Am J Roentgenol. 1984. 142:91–95.
Article12. Schindera ST, Triller J, Vock P, Hoppe H. Detection of hepatic portal venous gas: its clinical impact and outcome. Emerg Radiol. 2006. 12:164–170.
Article13. Fisher JK. Computed tomography of colonic pneumatosis intestinalis with mesenteric and portal venous air. J Comput Assist Tomogr. 1984. 8:573–574.
Article14. Ho LM, Paulson EK, Thompson WM. Pneumatosis intestinalis in the adult: benign to life-threatening causes. AJR Am J Roentgenol. 2007. 188:1604–1613.
Article15. Day DL, Ramsay NK, Letourneau JG. Pneumatosis intestinalis after bone marrow transplantation. AJR Am J Roentgenol. 1988. 151:85–87.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- A Case of Pneumatosis Intestinalis in Refractory Acute Precursor B-Cell Lymphoblastic Leukemia-Lymphoma
- A Case of Pneumatosis Cystoides Intestinalis in a Patient with Chronic Diarrhea and Abdominal Pain
- A Case of Recurrent Pneumatosis Cystoides Intestinalis Associated with Recurrent Pneumoperitoneum
- A Case of Primary Pneumatosis Cystoides Intestinalis in a Patient with Chronic Abdominal Pain
- A Case of Pneumatosis Cystoides Intestinalis in a Patient with Systemic Lupus Erythematosus