J Periodontal Implant Sci.
2015 Feb;45(1):23-29. 10.5051/jpis.2015.45.1.23.
Complication incidence of two implant systems up to six years: a comparison between internal and external connection implants
- Affiliations
-
- 1Department of Periodontics, Asan Medical Center, Seoul, Korea. shkimperio@amc.seoul.kr
- 2Department of Dentistry, University of Ulsan College of Medicine, Seoul, Korea.
- 3Department of Periodontology, Dental Research Institute, Seoul National University School of Dentistry, Seoul, Korea.
- KMID: 2027829
- DOI: http://doi.org/10.5051/jpis.2015.45.1.23
Abstract
- PURPOSE
This study was conducted to compare the cumulative survival rates (CSRs) and the incidence of postloading complications (PLCs) between a bone-level internal connection system (ICS-BL) and an external connection system (ECS).
METHODS
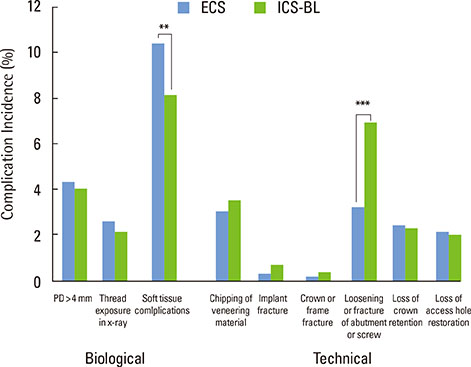
The medical records of patients treated with either a ICS-BL or ECS between 2007 and 2010 at Asan Medical Center were reviewed. PLCs were divided into two categories: biological and technical. Biological complications included >4 mm of probing pocket depth, thread exposure in radiographs, and soft tissue complications, whereas technical complications included chipping of the veneering material, fracture of the implant, fracture of the crown, loosening or fracture of the abutment or screw, loss of retention, and loss of access hole filling material. CSRs were determined by a life-table analysis and compared using the log-rank chi-square test. The incidence of PLC was compared with the Pearson chi-squared test.
RESULTS
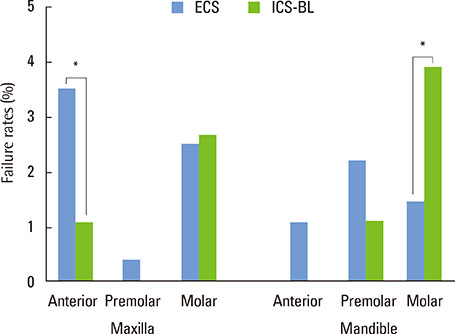
A total of 2,651 implants in 1,074 patients (1,167 ICS-BLs in 551 patients and 1,484 ECSs in 523 patients) were analyzed. The average observation periods were 3.4 years for the ICS-BLs and 3.1 years for the ECSs. The six-year CSR of all implants was 96.1% (94.9% for the ICS-BLs and 97.1% for the ECSs, P=0.619). Soft tissue complications were more frequent with the ECSs (P=0.005) and loosening or fracture of the abutment or screw occurred more frequently with the ICS-BLs (P<0.001).
CONCLUSIONS
Within the limitations of this study, the ICS-BL was more prone to technical complications while the ECS was more vulnerable to biological complications.
MeSH Terms
Figure
Cited by 1 articles
-
A 5-year prospective clinical study of Neobiotech implants for partially edentulous patients
Wilmart Labriaga, Ju-Hee Hong, Jin-Hong Park, Sang-Wan Shin, Jeong-Yol Lee
J Korean Acad Prosthodont. 2017;55(3):272-278. doi: 10.4047/jkap.2017.55.3.272.
Reference
-
1. Brånemark PI, Adell R, Breine U, Hansson BO, Lindström J, Ohlsson A. Intra-osseous anchorage of dental prostheses. I. Experimental studies. Scand J Plast Reconstr Surg. 1969; 3:81–100.2. Astrand P, Ahlqvist J, Gunne J, Nilson H. Implant treatment of patients with edentulous jaws: a 20-year follow-up. Clin Implant Dent Relat Res. 2008; 10:207–217.3. Lekholm U, Grondahl K, Jemt T. Outcome of oral implant treatment in partially edentulous jaws followed 20 years in clinical function. Clin Implant Dent Relat Res. 2006; 8:178–186.
Article4. Astrand P, Engquist B, Dahlgren S, Grondahl K, Engquist E, Feldmann H. Astra Tech and Brånemark system implants: a 5-year prospective study of marginal bone reactions. Clin Oral Implants Res. 2004; 15:413–420.
Article5. Becker W, Becker BE. Replacement of maxillary and mandibular molars with single endosseous implant restorations: a retrospective study. J Prosthet Dent. 1995; 74:51–55.
Article6. Brånemark PI, Zarb GA, Albrektsson T. Tissue-Integrated prostheses: osseointegration in clinical dentistry. Chicago, IL: Quintessence Publishing Co.;1985.7. Finger IM, Castellon P, Block M, Elian N. The evolution of external and internal implant/abutment connections. Pract Proced Aesthet Dent. 2003; 15:625–632.8. Misch K, Wang HL. Implant surgery complications: etiology and treatment. Implant Dent. 2008; 17:159–168.
Article9. Sutter F, Weber HP, Sorensen J, Belser UC. The new restorative concept of the ITI dental implant system: design and engineering. Int J Periodontics Restorative Dent. 1993; 13:409–431.10. Maeda Y, Satoh T, Sogo M. In vitro differences of stress concentrations for internal and external hex implant-abutment connections: a short communication. J Oral Rehabil. 2006; 33:75–78.
Article11. Cha HS, Kim YS, Jeon JH, Lee JH. Cumulative survival rate and complication rates of single-tooth implant; focused on the coronal fracture of fixture in the internal connection implant. J Oral Rehabil. 2013; 40:595–602.
Article12. Binon PP, McHugh MJ. The effect of eliminating implant/abutment rotational misfit on screw joint stability. Int J Prosthodont. 1996; 9:511–519.13. Dailey B, Jordan L, Blind O, Tavernier B. Axial displacement of abutments into implants and implant replicas, with the tapered cone-screw internal connection, as a function of tightening torque. Int J Oral Maxillofac Implants. 2009; 24:251–256.14. Kim KS, Lim YJ, Kim MJ, Kwon HB, Yang JH, Lee JB, et al. Variation in the total lengths of abutment/implant assemblies generated with a function of applied tightening torque in external and internal implant-abutment connection. Clin Oral Implants Res. 2011; 22:834–839.
Article15. Lee JH, Kim DG, Park CJ, Cho LR. Axial displacements in external and internal implant-abutment connection. Clin Oral Implants Res. 2014; 25:e83–e89.
Article16. Gracis S, Michalakis K, Vigolo P, Vult von Steyern P, Zwahlen M, Sailer I. Internal vs. external connections for abutments/reconstructions: a systematic review. Clin Oral Implants Res. 2012; 23:Suppl 6. 202–216.
Article17. Papaspyridakos P, Chen CJ, Chuang SK, Weber HP, Gallucci GO. A systematic review of biologic and technical complications with fixed implant rehabilitations for edentulous patients. Int J Oral Maxillofac Implants. 2012; 27:102–110.18. Buser D, von Arx T, ten Bruggenkate C, Weingart D. Basic surgical principles with ITI implants. Clin Oral Implants Res. 2000; 11:Suppl 1. 59–68.
Article19. van Steenberghe D, De Mars G, Quirynen M, Jacobs R, Naert I. A prospective split-mouth comparative study of two screw-shaped self-tapping pure titanium implant systems. Clin Oral Implants Res. 2000; 11:202–209.
Article20. Jung RE, Zembic A, Pjetursson BE, Zwahlen M, Thoma DS. Systematic review of the survival rate and the incidence of biological, technical, and aesthetic complications of single crowns on implants reported in longitudinal studies with a mean follow-up of 5 years. Clin Oral Implants Res. 2012; 23:Suppl 6. 2–21.21. Romeo E, Storelli S. Systematic review of the survival rate and the biological, technical, and aesthetic complications of fixed dental prostheses with cantilevers on implants reported in longitudinal studies with a mean of 5 years follow-up. Clin Oral Implants Res. 2012; 23:Suppl 6. 39–49.
Article22. Koo KT, Lee EJ, Kim JY, Seol YJ, Han JS, Kim TI, et al. The effect of internal versus external abutment connection modes on crestal bone changes around dental implants: a radiographic analysis. J Periodontol. 2012; 83:1104–1109.
Article23. Pjetursson BE, Thoma D, Jung R, Zwahlen M, Zembic A. A systematic review of the survival and complication rates of implant-supported fixed dental prostheses (FDPs) after a mean observation period of at least 5 years. Clin Oral Implants Res. 2012; 23:Suppl 6. 22–38.
Article24. Lazzara RJ, Porter SS. Platform switching: a new concept in implant dentistry for controlling postrestorative crestal bone levels. Int J Periodontics Restorative Dent. 2006; 26:9–17.25. Astrand P, Engquist B, Dahlgren S, Engquist E, Feldmann H, Grondahl K. Astra Tech and Brånemark System implants: a prospective 5-year comparative study. Results after one year. Clin Implant Dent Relat Res. 1999; 1:17–26.
Article26. Squier RS, Psoter WJ, Taylor TD. Removal torques of conical, tapered implant abutments: the effects of anodization and reduction of surface area. Int J Oral Maxillofac Implants. 2002; 17:24–27.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Effects of abutment angulation and type of connection on the fracture strength of zirconia abutments
- Long-term effect of implant-abutment connection type on marginal bone loss and survival of dental implants
- Concept and application of implant connection systems: Part II. Placement and restoration of external connection implant and tissue level implant
- Three-dimensional finite element analysis of stress distribution and preload of different connection types implant with initial clamping
- Effect of casting procedure on screw loosening of UCLA abutment in two implant-abutment connection systems