J Korean Fract Soc.
2008 Oct;21(4):286-291. 10.12671/jkfs.2008.21.4.286.
A Comparison between Minimally Invasive Plate Osteosynthesis & Interlocking Intramedullary Nailing in Distal Tibia Fractures
- Affiliations
-
- 1Department of Orthopedic Surgery, Hallym University Sacred Hospital, College of Medicine, Hallym University, Anyang, Korea. sysong@hallym.or.kr
- KMID: 1480917
- DOI: http://doi.org/10.12671/jkfs.2008.21.4.286
Abstract
-
PURPOSE: To compare the effectiveness between minimally invasive plate osteosynthesis (MIPO) and interlocking IM nailing in the treatment of distal tibia fracture without involvement of ankle joint retrospectively.
MATERIALS AND METHODS
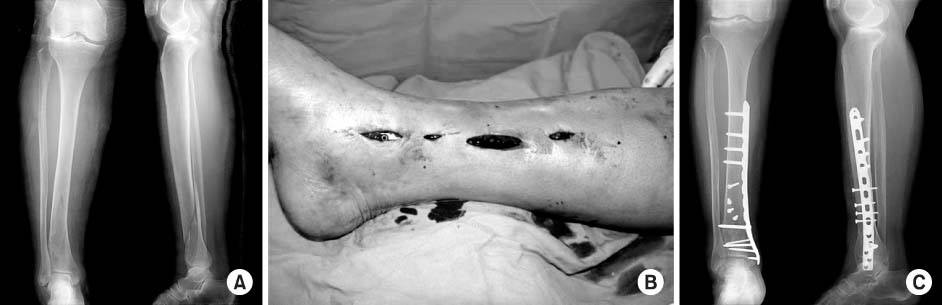
38 patients with distal tibia fracture from Jan. 2004 to Oct. 2005 were divided into two groups. Minimum follow-up was for 12 months. Group MIPO consisted of 18 patients were treated with MIPO and group Nail consisted of 20 patients were treated with interlocking intramedullary nail. The results were compared between two groups by assessing bony union time and operation time. Clinical evaluation was evaluated by Olerud score.
RESULTS
The mean bony union time was 14.4 weeks (12~17 weeks) in group MIPO and 16.7 weeks (13~19 weeks) in group Nail (p=0.011). The mean operation time was 1.05 hours (0.6~1.6 hours) in group MIPO and 0.74 hours (0.4~1.1 hours) in group Nail (p=0.044). The Olerud score was 83.8 (75~100) in group MIPO and was 89.6 (70~100) in group Nail (p=0.075). In Complication, group MIPO showed one metal failure and two skin irritations, group Nail showed three superficial wound infections.
CONCLUSION
MIPO was the shorter bony union time and the longer operation time than the interlocking intramedullary nailing. There were no significant differences between the two groups in clinical results.
Keyword
Figure
Cited by 2 articles
-
Analysis of the Result Treated with Locking Compression Plate-Distal Tibia and Zimmer Periarticular Locking Plate in Distal Tibia Fracture
Jun-Young Lee, Sang-Ho Ha, Sung-Won Cho, Sung-Hae Park
J Korean Fract Soc. 2013;26(2):118-125. doi: 10.12671/jkfs.2013.26.2.118.Intramedullary Nailing of Distal Tibial Fractures with Percutaneous Reduction by Pointed Reduction Forceps
Jae-Kwang Hwang, Chung-Hwan Kim, Young-Joon Choi, Gi-Won Lee, Hyun-Il Lee, Tae-Kyung Kim
J Korean Fract Soc. 2014;27(2):144-150. doi: 10.12671/jkfs.2014.27.2.144.
Reference
-
1. Asche G. Results of the treatment of femoral and tibial fractures following interlocking nailing and plate osteosynthesis. A comparative retrospective study. Zentralbl Chir. 1989; 114:1146–1154.2. Bone LB, Johnson KD. Treatment of tibial fractures by reaming and intramedullary nailing. J Bone Joint Surg Am. 1986; 68:877–887.
Article3. Chang SA, Ahn HS, Byun YS, Kim JH, Bang HH, Kwon DY. Minimally invasive plate osteosynthesis in unstable fractures of the distal tibia. J Korean Fracture Soc. 2005; 18:155–159.
Article4. Dehne E. Ambulatory treatment of the fractured tibia. Clin Orthop Relat Res. 1974; 105:192–201.
Article5. Hahn D, Bradbury N, Hartley R, Radford PJ. Intramedullary nail breakage in distal fractures of the tibia. Injury. 1996; 27:323–327.
Article6. Helfet DL, Shonnard PY, Levine D, Borrelli J Jr. Minimally invasive plate osteosynthesis of distal fractures of the tibia. Injury. 1997; 28:suppl 1. A42–A48.
Article7. Im GI, Kim DY, Shin JH, Youn KS, Cho WH. Comparative analysis of interlocking nail and anatomical plate in the treatment of distal tibial fracture. J Korean Soc Fract. 1999; 12:632–637.
Article8. Krettek C, Stephan C, Schandelmaier P, Richter M, Pape HC, Miclau T. The use of Poller screws as blocking screws in stabilizing tibial fractures treated with small diameter intrameduallary nails. J Bone Joint Surg Br. 1999; 81:963–968.9. Na HY, Park YJ, Ko SH, Choi WS, Lee YS, Yoon KD. Comparative analysis of interlocking IM nailing and LC-DCP fixation in the treatment of distal tibial fracture. J Korean Soc Fract. 2002; 15:152–158.
Article10. Oh CW, Kyung HS, Park IH, Kim PT, Ihn JC. Distal tibial metaphyseal fractures treated by percutaneous plate osteosynthesis. Clin Orthop Relat Res. 2003; 408:286–291.
Article11. Olerud C, Molander H. A scoring scale for symptom evaluation after ankle fracture. Arch Orthop Trauma Surg. 1984; 103:190–194.
Article12. Park KC, Park YS. Minimally invasive plate osteosynthesis for distal tibial metaphyseal fracture. J Korean Fract Soc. 2005; 18:264–268.
Article13. Song SJ, Cho DY, Yoon HK, Shin DE, Kim JH, Kim TH. Interlocking intramedullary nailing in the distal metaphyseal fractures of the tibia. J Korean Fract Soc. 2005; 18:275–280.
Article14. Teeny SM, Wiss DA. Open reduction and internal fixation of tibial plafond fractures. Variables contributing to poor results and complications. Clin Orthop Relat Res. 1993; 292:108–117.15. Weller S, Hontzsch D, Frigg R. Epiperiostal, percutaneous plate osteosynthesis. A new minimally invasive technique with reference to "biological osteosynthesis". Unfallchirurg. 1998; 101:115–121.16. Wyrsch B, McFerran MA, McAndrew M, et al. Operative treatment of fractures of the tibial plafond. A randomized, prospective syudy. J Bone Joint Surg Am. 1996; 78:1646–1657.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- A Comparison of the Results between Intramedullary Nailing and Minimally Invasive Plate Osteosynthesis in Distal Tibia Fractures
- Comparative Study Using of Treatment with Minimally Invasive Plate Osteosynthesis Using Periarticular Plate and Interlocking Intramedullary Nailing in Distal Tibia Fractures
- Comparison of Results between Minimally Invasive Plate Fixation and Antegrade Intramedullary Nailing of Recon-Type in Low-Energy Injury Distal Femoral Shaft Fractures
- Treatment of the Fracture of Distal Tibia with the Intramedullary Nailing (Comparison between Ender and Interlocking Nailing)
- Comparative Study of Intramedullary Nailing and Plate for Metaphyseal Fractures of the Distal Tibia